Evidence-based therapy for addiction refers to treatment methods that are backed by scientific evidence, often through controlled, randomized studies. These therapies have undergone rigorous testing and evaluation to determine their effectiveness in treating substance abuse and addiction.
The Types of evidence-based therapies commonly used in addiction treatment range from Medication-Assisted Treatment (MAT) to Cognitive Behavioral Therapy (CBT), and Dialectical Behavior Therapy (DBT), among others.
The Benefits Of Evidence-Based Therapy For Addiction include higher success rates in long-term recovery, individualized treatment plans, and scientifically proven techniques designed to address the root causes of addiction.
What Are The Types Of Evidence-Based Therapies?

Each of these therapies is backed by scientific research demonstrating its effectiveness in treating addiction. These aren’t one-size-fits-all solutions but rather a toolbox from which healthcare providers can select the most appropriate treatment for an individual’s specific needs.
Medication-Assisted Treatment (MAT) is one of the most effective types of evidence-based therapy for addiction, particularly for opioids, alcohol, and nicotine. It involves using medications alongside behavioral therapy to manage withdrawal symptoms and reduce cravings.
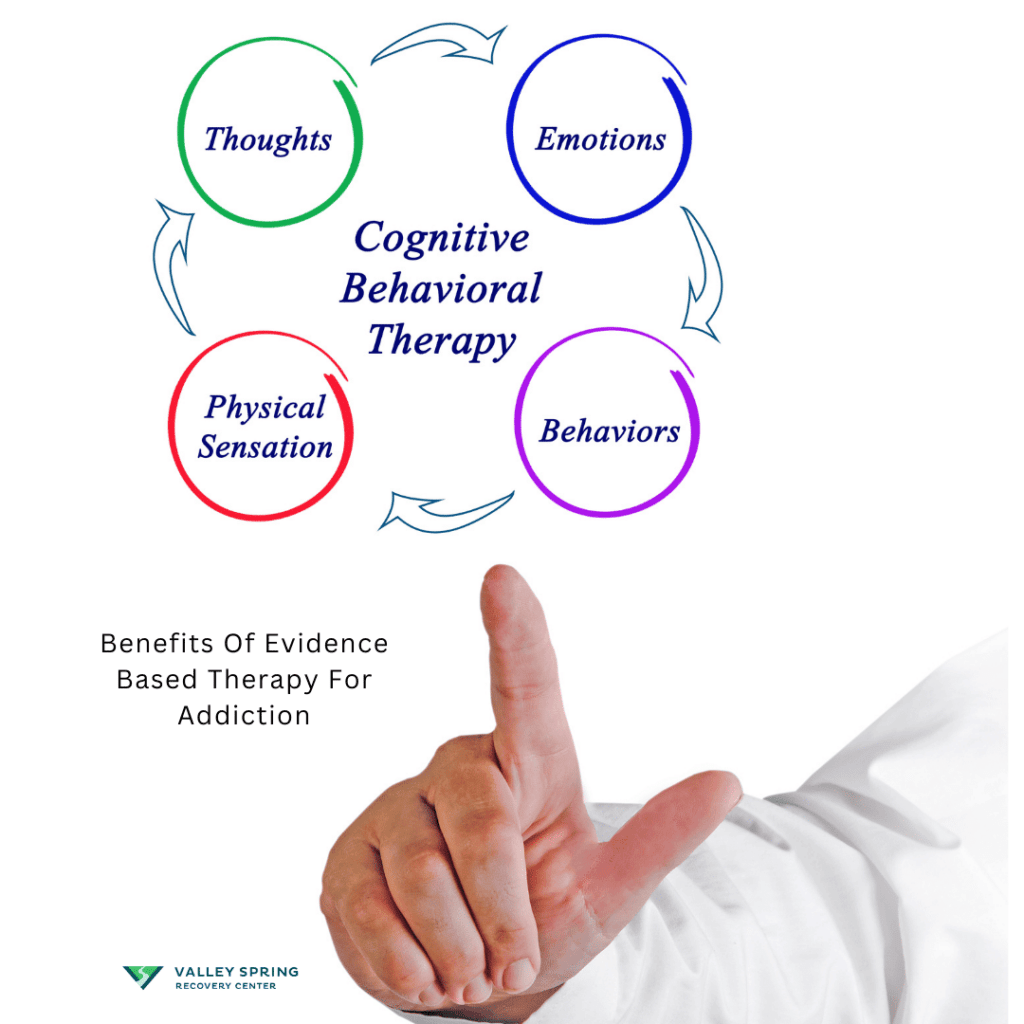
Cognitive Behavioral Therapy (CBT) addresses the negative thought patterns and behaviors that lead to substance abuse. It equips individuals with coping mechanisms and problem-solving skills, aiming to prevent relapse.
Dialectical Behavior Therapy (DBT) is often used for individuals with emotional regulation issues or borderline personality disorder alongside substance abuse. It teaches mindfulness and emotional regulation skills to help manage stress and reduce dependence on substances.
Motivational Interviewing (MI) is a patient-centered approach designed to spark motivation to change. It focuses on resolving ambivalence to facilitate the stages of change and recovery.
Contingency Management (CM) is a behavioral therapy that uses reward-based incentives to encourage sobriety and attendance in treatment programs. Patients might receive vouchers or other small rewards for negative drug tests, for example.
| Type of Therapy | Description | Primary Uses | Pros | Cons |
|---|---|---|---|---|
| Medication-Assisted Treatment (MAT) | Uses FDA-approved medications alongside counseling and behavioral therapies. | Opioid, Alcohol, and Tobacco Addiction | Highly effective in reducing withdrawal symptoms and cravings. | Medication costs and the potential for misuse of the prescribed drugs. |
| Cognitive Behavioral Therapy (CBT) | Short-term, goal-oriented therapy that changes patterns of thinking and behavior. | Various Substance and Behavioral Addictions | Equips individuals with practical skills to identify triggers and develop coping mechanisms. | Requires active participation and introspection, which might be challenging for some individuals. |
| Contingency Management (CM) | Involves giving tangible rewards to encourage drug-free behavior. | Stimulant and Opioid Addiction, Treatment retention | Highly effective in promoting initial abstinence and retaining clients in treatment. | Controversial due to the use of external motivators, such as money or prizes. |
| Motivational Interviewing (MI) | Client-centered approach that elicits and strengthens the individual’s own motivation for change. | Substance and Alcohol Abuse, Treatment readiness | Helps clients articulate their own reasons for change, increasing engagement. | Less directive, may not be suitable for clients who need a more structured approach. |
What Determines If A Therapy Is Evidence-Based?
Controlled, randomized studies are the gold standard for establishing a therapy as evidence-based. In these studies, participants are randomly assigned to either a treatment group receiving the therapy in question or a control group receiving a placebo or standard treatment. The outcomes are then rigorously measured and compared.
Peer-reviewed publications add another layer of credibility. For a therapy to be considered evidence-based, it usually needs to be published in a reputable, peer-reviewed journal where experts in the field have scrutinized the methodology and results.
Replicability is a key feature of evidence-based therapy. The results of the initial studies need to be replicable by independent researchers under similar conditions. This ensures that the therapy’s effectiveness is not a one-time occurrence but is generalizable to a broader population.
Long-term efficacy is critical in the field of addiction treatment. Not only should the therapy prove effective in the short term, but it should also demonstrate long-lasting benefits, reducing rates of relapse and leading to sustained recovery.
Professional Endorsement often comes after a body of evidence has accumulated. Medical and psychological associations, based on comprehensive reviews of the research, may officially endorse a therapy as being evidence-based.
What Are The Benefits of Evidence-Based Therapy?
The benefits of evidence-based therapy are multi-faceted, offering both quantitative and qualitative improvements in addiction treatment. They provide a roadmap to recovery that is substantiated by research, personalizing the path for each individual while utilizing techniques that have been verified for their effectiveness.
Higher Success Rates in Long-Term Recovery are one of the most compelling advantages of evidence-based therapy. Because these therapies have been rigorously tested, they are more likely to yield beneficial outcomes, including lower relapse rates and improved quality of life over the long term.
Individualized Treatment Plans can be more accurately formulated using evidence-based approaches. These therapies often include diagnostic tools and methods that allow for a more personalized treatment plan, tailored to the specific needs and circumstances of each patient.
Scientifically Proven Techniques are employed in evidence-based therapy, ensuring that the treatment is more than just ‘trial and error.’ These methods have undergone extensive research and testing, proving their efficacy in treating addiction and improving mental health.
Greater Cost-Effectiveness is another benefit. Although the initial cost of evidence-based therapies might be higher, their proven effectiveness often results in lower overall healthcare costs, including fewer hospital admissions and less need for ongoing treatment.
Enhanced Accountability comes from the structured nature of evidence-based therapy, which often includes regular assessments and progress tracking. This allows both the therapist and the patient to monitor the treatment’s effectiveness and make necessary adjustments.
What Are The Downsides of Evidence-Based Therapy?
Limited Scope of Treatment is one of the most common criticisms of evidence-based therapy. These approaches focus on what has been scientifically validated, which might exclude potentially beneficial but less-studied or alternative treatments.
Lack of Personalization can sometimes be an issue. Evidence-based therapies often employ standardized treatment plans that may not be fully adaptable to every individual’s unique circumstances or co-occurring conditions.
Cost and Accessibility are significant concerns. Some evidence-based therapies, especially newer or specialized ones, can be expensive and may not be covered by insurance. Moreover, professionals trained in these therapies may be limited in certain geographical areas.
Time-Intensive Nature of some therapies could be a drawback for some people. Therapies like Cognitive Behavioral Therapy (CBT) may require a substantial time commitment, which can be challenging for those who have obligations like work, school, or family.
Treatment Resistance is another issue to consider. Not every individual responds to evidence-based treatments, and some may find these methods unhelpful or uncomfortable, potentially discouraging further treatment-seeking behavior.
Where Can You Get Evidence-Based Therapy For Addiction?
Acquiring evidence-based therapy for addiction may depend on several factors, including geographic location, financial resources, and specific treatment needs. However, the growing awareness of the effectiveness of these treatments is leading to broader availability across different healthcare settings.

Certified Rehab Centers are among the most reliable places to find evidence-based therapy options. Look for facilities that are accredited by recognized organizations such as the Commission on Accreditation of Rehabilitation Facilities (CARF) or the Joint Commission. These institutions are more likely to employ scientifically-validated treatment methods. According to Statista, In 2020, there were 16,066 substance abuse rehab centers in the United States.
Specialized Therapists and Counselors often provide evidence-based therapies in private practices or within multi-disciplinary healthcare settings. Many are specialists in addiction therapy and have received advanced training in evidence-based techniques.
Telehealth Services have expanded the availability of evidence-based therapy for addiction, offering virtual sessions with qualified therapists. Telehealth treatment for addiction can be particularly beneficial for those who are geographically isolated or unable to attend in-person treatment due to the ongoing COVID-19 pandemic or other constraints.
Outpatient Clinics sometimes offer evidence-based treatments as part of their menu of services. These clinics can be a more flexible option for those who need to balance treatment with other commitments like work or family.
Community Health Centers and Public Health Clinics are increasingly incorporating evidence-based therapies into their treatment programs, making these therapies more accessible to a broader demographic, including those with financial constraints.
Who Invented The Term Evidence-Based Therapy?
The term “evidence-based therapy” didn’t originate from a single individual but rather evolved from the broader movement toward evidence-based medicine, and subsequently, evidence-based practice (EBP) in psychology and allied health fields. According to the Oxford Research Encyclopedias, EBP signifies a transition from naïve empiricism, characterized by unstructured observations of patient change, to systematic empiricism, which involves refining those observations through rigorous research methods. This methodological shift in psychology has its roots partially in the development of randomization methods that emerged in the early 20th century.
In American psychology, EBP is often described as a “three-legged stool,” with the legs representing high-quality treatment outcome evidence, clinical expertise, and patient preferences and values. The research component of this model is usually ranked in a hierarchy of evidentiary certainty, with randomized controlled trials and meta-analyses at the top. The concept has also led to the identification of empirically supported treatments, which are specific psychotherapies proven effective for particular psychological conditions.
Despite its significant influence, the concept of evidence-based therapy is not without its critics and remains a subject of scientific controversy. Some argue that the research supporting EBP is less compelling than what its proponents claim. Nonetheless, it has profoundly impacted the field of psychology and therapy, emphasizing the importance of empirical research in the evaluation and application of therapeutic methods.
When did evidence-based therapy become popular?
Evidence-based therapy gained significant traction in the 1990s, although the roots of the approach can be traced back to earlier years. The term “evidence-based medicine” was coined in a program for medical students at McMaster University in Canada in the early 1990s. Shortly after, the concept spread to other disciplines, including psychology and mental health treatment. The movement emphasized the use of scientific research and clinical evidence to inform treatment decisions, as opposed to relying solely on clinical expertise and traditional approaches.
By the late 1990s and early 2000s, professional organizations like the American Psychological Association began to emphasize the importance of using evidence-based practices. Over time, it became increasingly common for insurance providers to require evidence-based treatments for reimbursement, further promoting the adoption of these methods. The movement has continued to grow, fueled by advancements in research methods and data analytics, and is now considered the standard approach for various psychological and medical conditions, including addiction treatment.
Is Evidence-Based Therapy Effective?

Evidence-based therapy has garnered substantial empirical support for its efficacy in treating various psychological conditions, including addiction and mental health disorders. Early research advocating for evidence-based approaches can be traced back to the 1990s, when the field started emphasizing the integration of clinical expertise with the best available research. Publications like the Journal of Consulting and Clinical Psychology have since published reviews affirming the superior outcomes of evidence-based methods when compared to traditional treatments lacking empirical support.
A seminal meta-analysis in the Psychological Bulletin further strengthened the case for evidence-based therapy, revealing statistically significant improvements in conditions like depression, anxiety, and PTSD. The effectiveness of evidence-based therapy extends across different modalities, including Cognitive Behavioral Therapy (CBT), Medication-Assisted Treatment (MAT), and Dialectical Behavior Therapy (DBT).
In recent years, advancements in neuroscience have further bolstered the standing of evidence-based approaches. A 2021 study in the Journal of Substance Abuse Treatment showed that evidence-based interventions, particularly when tailored to individual needs, led to better long-term recovery outcomes for patients with substance use disorders.
Not only does evidence-based therapy show marked effectiveness in treating conditions, but it also excels in relapse prevention. According to a paper in the American Journal of Psychiatry, patients undergoing evidence-based treatment methods experienced fewer relapses and a higher quality of life compared to those on standard treatments. Overall, the growing body of research confirms that evidence-based therapy offers a robust and versatile framework for treating a wide array of psychological disorders.
How Does Evidence-Based Therapy Integrate with Other Treatments?
Evidence-based therapy is often part of a multi-faceted treatment plan that may include medication, lifestyle changes, and other therapeutic techniques. The integration of multiple treatment modalities enhances the effectiveness and provides a more holistic approach to addiction recovery.
Can Evidence-Based Therapy Help with Co-Occurring Disorders?
Yes, many Evidence-Based Therapies are designed to address not only addiction but also co-occurring mental health disorders like depression or anxiety. This makes them particularly effective for individuals dealing with multiple issues simultaneously.
How Long Does a Typical Evidence-Based Therapy Session Last?
The duration of a therapy session can vary depending on the type of Evidence-Based Therapy and the specific needs of the patient. However, most sessions last between 45 to 60 minutes. The total length of the treatment also varies and is tailored to individual needs.
Is Online Evidence-Based Therapy Effective?
Recent studies suggest that online or telehealth versions of Evidence-Based Therapies can be just as effective as in-person sessions. This makes them a viable option for those who may have difficulty accessing traditional healthcare services.
What Qualifications Should a Therapist Have to Provide Evidence-Based Therapy?
Therapists providing Evidence-Based Therapy should have relevant educational qualifications, such as a Master’s or Doctorate in psychology, social work, or a related field. Additionally, they should have specialized training and certification in the specific Evidence-Based Therapy they are offering.
Why is Medication-Assisted Treatment Considered An Evidence-Based Therapy Since It Uses Medication?
Medication-assisted treatment (MAT) is often classified as an evidence-based therapy because it meets the key criteria of being supported by empirical research and scientific evidence. The term “evidence-based” refers to interventions that have undergone rigorous scientific evaluation and have been proven to be effective. In the case of MAT, numerous studies have demonstrated its efficacy in treating substance use disorders, particularly opioid addiction.
Integration with Behavioral Therapies: MAT is not solely about medication; it is a comprehensive approach that combines FDA-approved medications with behavioral therapies and counseling. This multi-faceted treatment model aligns with the principles of evidence-based therapy, which often involves a combination of treatments tailored to individual needs.
Scientific Validation: The medications used in MAT, such as Methadone, Buprenorphine, and Naltrexone, have been rigorously tested through clinical trials and have been found to be effective in reducing withdrawal symptoms, cravings, and the rates of relapse. This scientific validation is a cornerstone of what makes a therapy “evidence-based.”
Standardized Guidelines: MAT is administered following standardized guidelines that healthcare providers adhere to, ensuring a consistent level of care. These guidelines are based on extensive research and are regularly updated to reflect new findings, another hallmark of evidence-based practice.
Adaptability: Like other evidence-based therapies, MAT can be adapted to meet the individual needs of each patient. Healthcare providers will often adjust medication dosages and incorporate different forms of behavioral therapy based on the patient’s progress, making it a flexible yet evidence-based approach.
Holistic Treatment: MAT addresses both the physiological and psychological aspects of addiction, offering a more holistic treatment solution. This aligns with the principles of evidence-based therapy, which often involves a multi-disciplinary approach to treatment.
Sources
Total number of substance abuse treatment facilities in the U.S. from 2003 to 2020, Statista. Accessed [August 24th, 2023] https://www.statista.com/statistics/450281/total-number-of-substance-abuse-treatment-facilities-in-the-us/
History Of Evidence Based Therapy, Oxford Research Dictionary. Accessed [August 25th, 2023] https://oxfordre.com/psychology/display/10.1093/acrefore/9780190236557.001.0001/acrefore-9780190236557-e-633
Ben Fisher
All author postsShare This Post










