Drug Addiction: Definition, Symptoms, Causes, Effects and Treatment

Drug addiction, officially recognized as a substance use disorder, affects approximately 19.7% of adults in the United States, according to 2023 data from the Substance Abuse and Mental Health Services Administration (SAMHSA). This condition is characterized by an uncontrollable urge to use drugs despite the significant harmful consequences it leads to. The roots of addiction are diverse, influenced by genetic predispositions, environmental factors, and psychological conditions, making it a complex issue that transcends socioeconomic boundaries.
Individuals suffering from drug addiction experience a range of symptoms, including persistent cravings, withdrawal symptoms, and a loss of control over drug use.
The causes of drug addiction include a combination of biological, environmental, and psychological factors that interact to increase vulnerability to substance dependency. Genetic predispositions make individuals more susceptible, while exposure to environments where drug use is normalized reinforces addictive behaviors. Stress, trauma, or mental health issues like anxiety lead individuals to turn to substances as a coping mechanism.
The effects of abusing substances are profound, impacting physical health through conditions like liver damage and mental health by increasing risks of disorders such as depression. Economically and socially, the repercussions are equally severe, affecting relationships and employment stability.
Treatment typically involves a combination of detoxification, rehabilitation programs, and therapy, emphasizing the necessity for a supportive and comprehensive approach to facilitate effective recovery.

This article has been enhanced with input from the Medical Director and Addiction Psychiatrist at Valley Spring Recovery Center, Dr. Michael Olla.
Check the end of each section for extra information from him.
What Is Drug Addiction?
Drug addiction, clinically recognized as substance use disorder, is a chronic, relapsing brain condition that compels an individual to seek and use drugs despite adverse consequences. This disorder is characterized by significant alterations in the brain’s structure and function, which lead to compulsive behaviors, impaired judgment, and prioritization of drug use. Extensive research, including findings from the National Institute on Drug Abuse (NIDA) in their March 2022 report “Drugs and the Brain,” explains how addiction manipulates the brain’s reward system. It significantly increases dopamine levels—a neurotransmitter linked to pleasure and reward—reinforcing the behavior to use drugs and creating a difficult-to-break cycle of addiction.
These profound brain changes affect various neural circuits, especially those related to reward, stress, and self-control. According to a study by Goldstein RZ and Volkow ND published in “Nature Reviews Neuroscience” in 2011, these changes persist well beyond the cessation of drug use, impacting an individual’s ability to make decisions and regulate behaviors long-term.
The prevalence of drug addiction varies significantly across different regions in the United States, influenced by local factors such as the availability of substances and access to treatment facilities. For instance, the New Jersey Department of Health’s 2022 statistics reveal that approximately 8% of adults in the state suffer from a substance use disorder, illustrating the significant impact of this chronic condition at a local level.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
What Is The Difference Between Drug Abuse And Addiction?
The difference between drug abuse and addiction is that drug abuse is the voluntary misuse of substances that deviates from social or medical norms. In contrast, addiction is a chronic, relapsing brain disorder marked by compulsive drug seeking and use despite adverse consequences. Drug abuse involves taking substances in harmful ways—for example, consuming higher doses of prescription opioids than advised to intensify euphoric effects—which increases the risk of physical harm and dependency.
Addiction is characterized by long-lasting changes in brain circuits related to reward, stress, and self-control, making it difficult to abstain without intervention. While drug abuse may appear sporadic and precede addiction, addiction itself involves profound physiological and psychological reliance, with adaptations such as altered neurotransmission and epigenetic changes that sustain cravings, marking the transition from harmful substance use to full-blown addiction and necessitating comprehensive treatment approaches.
What Is The Difference Between Drug Dependence And Addiction?

The difference between drug dependence and addiction is that drug dependence is the body’s physiological adaptation to sustained drug use, exhibiting tolerance and withdrawal symptoms without compulsive behavior, while addiction is a complex brain disorder marked by compulsive drug-seeking despite harmful consequences. Dependence results from long-term exposure to drugs, including psychoactive medications, beta-blockers, and antidepressants, and manifests as manageable physical responses. Abrupt cessation of such drugs triggers withdrawal without addictive behavior.
Addiction involves significant, lasting changes in brain circuits related to reward, motivation, and memory, leading to behavioral, physiological, and psychological symptoms such as powerful cravings and loss of control over drug use. The DSM-5 now distinguishes these conditions by focusing on behavioral symptoms to enhance diagnostic accuracy and treatment efficacy, an update supported by the American Psychiatric Association.
What Is The Difference Between Drug Tolerance And Dependence?
The difference between drug tolerance and dependence includes physiological adaptations requiring increased dosage to achieve initial effects (tolerance) versus the body’s physical and psychological reliance resulting in withdrawal symptoms when drug use stops (dependence).
Drug tolerance is the body’s diminished response to a drug over time, requiring higher doses to achieve the same effect. Tolerance alone does not necessarily lead to dependence but occurs as part of the dependence process. Drug dependence is marked by the development of withdrawal symptoms when drug use is reduced or stopped, indicating a physical and psychological reliance on the substance.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
What Is The Difference Between Drug Addiction And Alcoholism?
The difference between drug addiction and alcoholism lies primarily in their legal status and societal perceptions – while alcoholism involves dependency on a legal and socially accepted substance, drug addiction typically involves illegal substances that carry a greater stigma, though both conditions share similar neurobiological mechanisms affecting the brain’s reward system.
Drug addiction is a complex disorder characterized by compulsive drug seeking and use despite harmful consequences. It involves significant changes in brain circuits involved in reward, stress, and self-control. These changes persist long after the cessation of drug use, making recovery challenging.
Drug addiction encompasses a variety of substances, each affecting the brain differently. For example, cocaine stimulates the central nervous system, creating a quick, intense euphoria, leading to severe psychological dependence and intense withdrawal symptoms without physical markers (National Institute on Drug Abuse, 2022).Treatment approaches thus vary; alcohol use disorder withdrawal symptoms require pharmacological management to ensure safety, reflecting these critical differences as highlighted in the 2022 Cycle of Alcohol Addiction report published by The National Institute on Alcohol Abuse and Alcoholism, NIAAA.
What Is The Difference Between Behavioral Addictions And Drug Addictions?
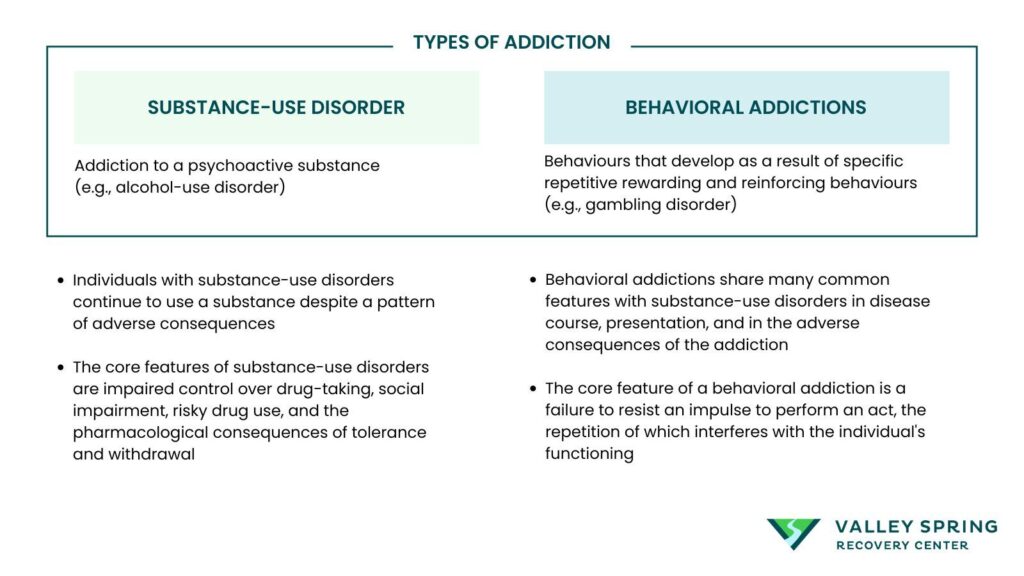
The difference between behavioral addictions and drug addictions lies in how they affect the brain – while behavioral addictions involve compulsive activities that naturally trigger the brain’s reward system without chemical substances, drug addictions involve the direct chemical alteration of brain function and structure through substance use, though both types activate similar reward pathways and require comprehensive treatment approaches.
Behavioral addiction refers to a compulsion to engage in activities that trigger the brain’s reward systems without involving substance consumption. Common examples include gambling, internet addiction, shopping, and excessive video gaming. For instance, gambling addiction involves repetitive behavior despite adverse consequences, driven by the desire to experience the thrill and potential reward of winning. These activities produce similar neurological responses to those induced by drugs, such as increased dopamine levels, which reinforce the behavior (Alavi, Seyyed Salman, et al., 2012).

What Are the Signs and Symptoms of Substance Use Disorder?
The signs and symptoms of substance use disorder include persistent cravings, withdrawal symptoms like anxiety and tremors, loss of control over consumption, and neglect of daily responsibilities. Physical and behavioral changes manifest through altered sleep patterns, mood swings, and declining personal care.
The most common signs of drug addiction are listed below.
- Persistent Use and Increased Tolerance: One of the most obvious signs of addiction is the need to consume increasingly larger amounts of the substance to achieve the same effects once felt at lower doses. For instance, an individual might start by taking a small dose of opioids for pain but gradually needs to increase the dose to achieve the same pain relief or euphoria (DSM-5).
- Withdrawal Symptoms: As the body becomes accustomed to the substance, discontinuation leads to physical and psychological withdrawal symptoms, such as nausea, shaking, anxiety, and irritability. This is particularly common with alcohol and benzodiazepines, where withdrawal is severe and, in some cases, life-threatening. Withdrawal manifests as both physical and psychological symptoms. Physical symptoms might include headaches, muscle pain, and sweating, while psychological symptoms could encompass anxiety, depression, and insomnia. Withdrawal indicates physical dependence and is a driving factor behind continued use due to the discomfort and difficulty associated with stopping.
- Loss of Control Over Use: Despite intentions to control or reduce their usage, individuals find themselves unable to do so. An example of loss of control is highlighted by Dr Michael Olla, who states, “Spending excessive time acquiring the substance of choice, using it, and recovering from its effects without regard for other responsibilities is a clear sign of addiction.”
- Craving: Cravings are powerful, intense urges to use a substance and are a psychological hallmark of addiction. The desire or urge to use the substance becomes powerful and overpowers other thoughts and responsibilities. These are triggered by exposure to drug-related cues, stress, or emotional distress, leading to relapse.
- Failure to Fulfill Obligations: Substance addiction leads to a neglect of responsibilities at work, home, or school, significantly impairing daily functioning and relationships.
- Continued Use Despite Problems: Individuals persist in using the substance even when it causes or exacerbates social or interpersonal problems.
- Social Withdrawal: As addiction deepens, individuals abandon hobbies, social activities, and occupational responsibilities that were once important to them, further isolating themselves.
- Hazardous Use: Engaging in risky behaviors, such as driving under the influence of operating machinery while impaired, indicates a disregard for safety directly related to substance use.
- Continued Use Despite Health Issues: Individuals continue using substances despite clear evidence of physical or psychological harm caused or worsened by their use.
- Changes in Appearance: Noticeable neglect in personal grooming and general physical decline are signs of chronic substance use.
- Altered Energy Levels: Users experience bursts of hyperactivity or, conversely, periods of extreme fatigue, depending on the substance used.
- Mood Swings: Extreme and sudden changes in mood, ranging from euphoria to intense irritability or sadness, indicative of substance use and withdrawal cycles.
- Denial: Individuals frequently underestimate the extent of their substance use or its impact, rationalizing or minimizing the severity to others and themselves.
- Secrecy and Deception: To hide their addiction, individuals might lie about their whereabouts, activities, and substance use, potentially leading to further social isolation and trust issues within personal relationships.
- Financial and Legal Troubles: Excessive spending on substances, debt accumulation, or legal issues related to substance use, such as arrests for DUI, are critical red flags.
- Engagement in Dangerous Activities: Addiction leads to engagement in increasingly risky activities necessary to obtain the substance or as part of its use.
- Ignoring Negative Consequences: Persisting in substance use despite obvious detrimental effects on health, relationships, and overall well-being underscores the compulsive nature of addiction.
The DSM-5 specifies that the presence of at least two of these symptoms within 12 months indicates a substance use disorder. The severity of the disorder is gauged by the number of criteria met: mild (2-3 criteria), moderate (4-5 criteria), and severe (6 or more criteria). This framework helps in recognizing the depth and extent of addiction, guiding healthcare professionals toward the most appropriate treatment and support strategies.
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
What Are The Causes Of Drug Addiction?
The causes of drug addiction encompass biological determinants, environmental catalysts, psychological and emotional triggers, and developmental and behavioral factors, highlighting the complex interplay of genetics, upbringing, mental health, and early substance exposure, according to the 2024 NIDA report titled “Drug Misuse and Addiction.”
- Biological Determinants: Genetic factors significantly influence an individual’s predisposition to substance dependency. A combination of genetic variables directly impacts vulnerability to addiction. Moreover, neurodevelopmental factors, notably the ongoing development of the prefrontal cortex in adolescents, heighten the risk of substance dependency, especially with early substance exposure.
According to Ducci, F.’s 2012 study, ‘The genetic basis of addictive disorders.’, 40-70% of addiction variation is attributed to genetic factors. Heritability estimates for cocaine dependence are 0.7, indicating that 70% of the variation is genetic. Twin concordance ratios for addiction are higher for monozygotic twins, with a ratio of 2.5 for cocaine dependence. The HTR2B gene is associated with impulsive aggression and addiction, and carriers are more likely to engage in violent behavior while intoxicated, with family history being a significant risk factor. - Environmental Catalysts: The environment plays a crucial role in determining the likelihood of addiction. Peer groups that promote substance misuse encourage similar behaviors in others. A family history of drug abuse intensifies this risk. Additionally, socioeconomic barriers, such as limited access to education and healthcare, increase susceptibility to addiction. These environmental influences are pivotal during critical developmental stages, shaping an individual’s addiction risk.
- Psychological and Emotional Triggers: Continuous stress and negative life events are significant psychological triggers for substance dependency. Disorders like Post-Traumatic Stress Disorder (PTSD), depression, and anxiety frequently accompany addiction, necessitating a dual-diagnosis approach for effective treatment. Peer pressure, along with physical and sexual abuse, early drug exposure, stress, and the role of parental guidance, profoundly influences an individual’s risk of substance use and addiction.
According to Guliyev, C.’s 2021 study, ‘Comparison of Individuals With and Without the Risk of Post-Traumatic Stress Disorder in Terms of Substance Use Features and Psychological Problems According to Their Substance Preferences.’, Individuals with alcohol-substance use disorders, opioid use disorder, cannabis use disorder, and alcohol use disorder showed PTSD frequencies of 29.8% (n = 162), 29.2% (n = 98), 33.3% (n = 13), and 35.7% (n = 20) respectively. Participants with PTSD symptoms scored higher in substance use features, diagnosis, life impact of substance use, cravings, addiction severity, difficulty in anger control, excitement-seeking behaviors, safe behavior deficiency, depression, and anxiety. - Developmental and Behavioral Factors: Early initiation of substance use markedly increases the risk of developing a long-term dependency. Certain personality traits or disorders predispose individuals to addiction. A comprehensive understanding of these diverse risk factors offers a holistic perspective on susceptibility to addiction, highlighting the complex interaction between biological, environmental, and psychological factors.
What Are The Effects of Drug Addiction?
The effects and consequences of drug addiction are far-reaching and profoundly impact nearly every part of an individual’s life, affecting their physical health, emotional well-being, relationships, and even their standing in society.
- Physical Health: One of the most immediate effects of drug addiction is physical health. Depending on the drug abused, individuals experience a range of health issues including liver damage, respiratory problems, cardiovascular diseases, stroke, cancer, and infectious diseases like HIV/AIDS from shared injection equipment. According to Santibanez, S. S.’s 2006 study, ‘Update and overview of practical epidemiologic aspects of HIV/AIDS among injection drug users in the United States.’, Injection Drug Users (IDUs) account for approximately 32% of new HIV diagnoses in the United States. IDUs range from approximately 1.4 million in 1998 to around 1.6 million by the end of 2023. This group has collectively accounted for the second-highest number of AIDS cases over a quarter-century, with specific state-level reductions ranging from 22% to 62%.
- Mental Health: Drug addiction co-occurs with a range of mental health issues, such as depression, anxiety, and schizophrenia. drug abuse exacerbates mental health conditions, creating a vicious cycle that’s difficult to break.
- Relationships: Addiction strains relationships with loved ones due to erratic or violent behavior, neglect of responsibilities, and other negative consequences of drug use. This leads to isolation from family and friends, creating a further emotional toll.
- Economic Impact: The financial burden of sustaining a drug habit leads to job loss and homelessness. The cost of purchasing the drug, coupled with reduced productivity and increased healthcare expenses, causes financial strain. According to Florence, C. S.’s 2016 study, ‘The Economic Burden of Prescription Opioid Overdose, Abuse, and Dependence in the United States, 2013.’, the economic burden of addiction in the United States amounts to $78.5 billion, with health care and drug abuse treatment costs making up an approximate 36.8% ($28.9 billion) of the total. Health care, drug abuse treatment, and criminal justice costs account for around 25% of the total economic burden and lost productivity accounts for a significant portion as well. On a smaller scale, the cost difference for patients diagnosed with opioid abuse or dependence when covered by Medicare, private insurance, or Medicaid is approximately $17,000, $15,500, and $13,700 respectively. Additionally, over $7.3 billion in state and local government funding is allocated for criminal justice activities related to addiction.
- Legal Consequences: Drug addiction leads to a host of legal problems, including arrest, incarceration, and a lifelong criminal record, which in turn affects employment prospects and social standing.
- Social Stigma: The societal perception of drug addicts is negative, which leads to stigmatization and further isolation. These social stigmas make it more difficult for individuals to seek help and exacerbate the emotional toll of addiction.
- Overall Quality of Life: Ultimately, drug addiction significantly lowers the user’s quality of life, leading to a loss of interest in activities that once brought joy, and many times leads to overdose and premature death.
What Are The Stages Of Drug Addiction?
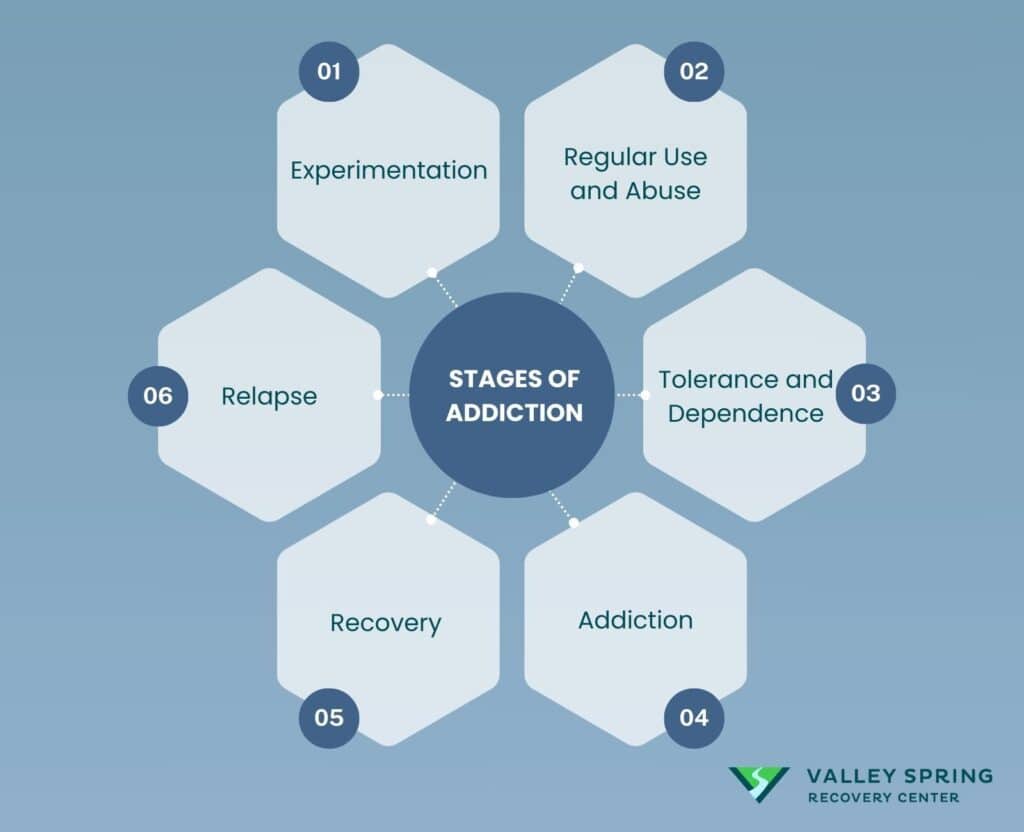
The stages of drug addiction include initial substance experimentation, progressive regular consumption, developing tolerance, compulsive usage patterns, treatment and healing, and potential setbacks during recovery. Understanding these distinct phases helps identify where someone might be in their journey with substance use.
Here are the key stages of drug addiction in detail below:
- Experimentation: Experimentation is typically the first stage of addiction, where individuals use substances occasionally out of curiosity, peer pressure, or to seek pleasure. During this phase, use is infrequent and, in some cases, does not progress any further. The National Institute on Drug Abuse (NIDA, 2020) notes that genetic factors significantly affect whether an individual moves beyond this stage.
- Regular Use and Abuse: As use becomes more frequent, the transition from experimentation to regular use and then to abuse occurs. This stage is characterized by the increasing priority given to substance use over other activities despite the awareness of adverse consequences. For some, substance use becomes a key method for coping with problems or emotions, escalating the risk of progressing to more severe stages.
- Tolerance and Dependence: Continuous and increased substance use leads to tolerance, where the body requires higher doses of the substance to achieve the initial effects. Dependence is psychological or physical, indicating that the body has adapted to the substance’s presence. Withdrawal symptoms will appear if substance use is reduced or stopped, signaling physical dependence.
- Addiction: Addiction is marked by the inability to stop using the substance despite harmful physical, psychological, and social consequences. At this stage, the use is compulsive and out of control. Addiction impacts various aspects of an individual’s life, including relationships, work, and health.
- Recovery: Recovery involves actively engaging in addiction treatment and recovery activities to overcome addiction. This includes therapy, medication-assisted treatment, and support groups. Recovery is an ongoing process and requires lifelong commitment and support to maintain sobriety.
- Relapse: Relapse is not uncommon and should be considered a part of the process rather than a failure. It occurs when an individual returns to substance use after a period of abstinence and highlights the need for continued or adjusted treatment strategies.
Are you covered for treatment?
Valley Spring Recovery Center is an approved provider for Blue Cross Blue Shield and Cigna, while also accepting many other major insurance carriers.
Check Coverage Now!What Are The Most Common Types of Drug Addiction?
The most common types of drug addiction include substances like opioids (oxycodone, hydrocodone, and heroin), cocaine, methamphetamine, cannabis (marijuana), alcohol, and benzodiazepines (such as Valium and Xanax). These drugs are prevalent due to their availability, potency, and the euphoric effects they induce, making them highly addictive and, in some cases, expensive.
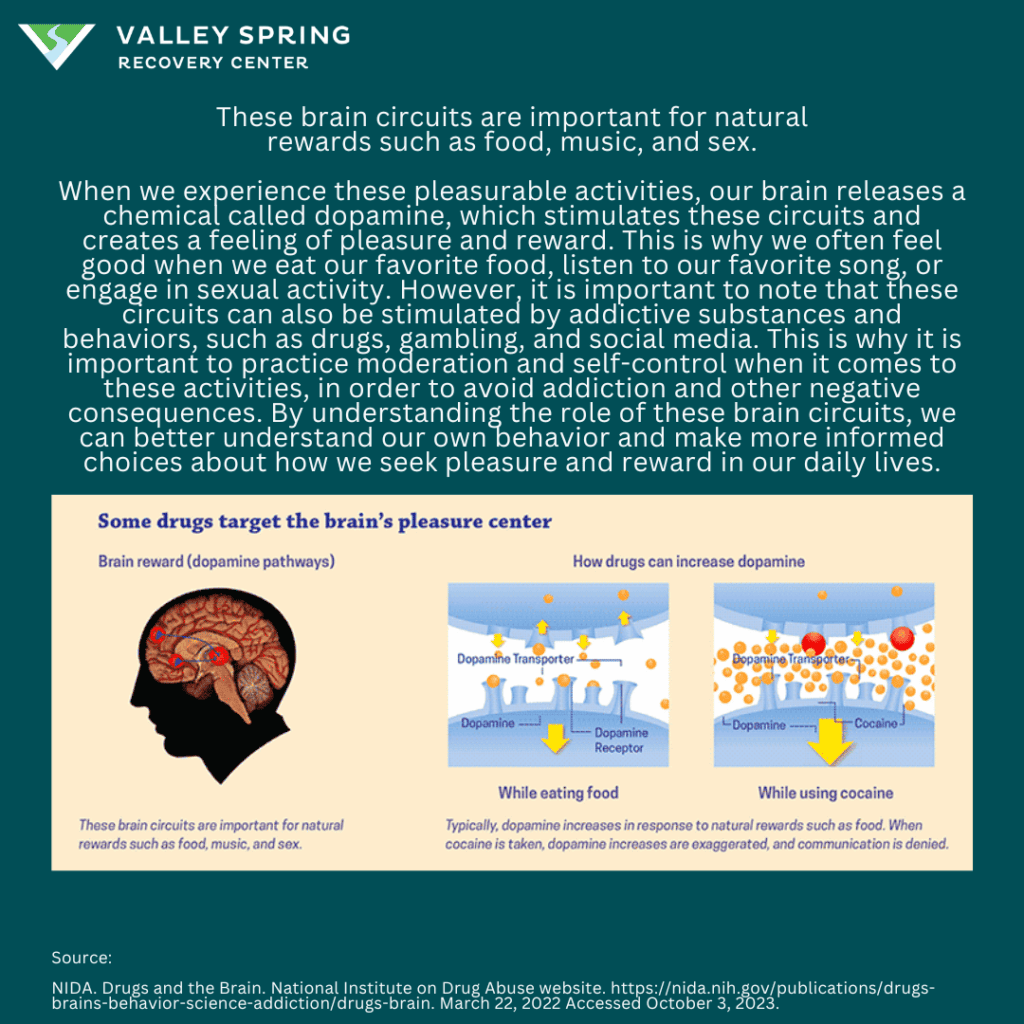
Drugs are addictive because they manipulate the brain’s reward system, releasing large amounts of dopamine, a neurotransmitter linked to pleasure and reinforcement. This dopamine surge creates a strong association between the drug and the pleasurable experience, driving individuals to repeatedly seek out the drug to achieve the same effect. Over time, this alters the brain’s natural dopamine production, making it difficult to experience pleasure from everyday activities and leading to a cycle of compulsive drug use despite negative consequences, a core feature of addiction.
Alcohol Use Disorder (AUD)

Alcohol use disorder (AUD) is a medical condition characterized by an impaired ability to stop or control alcohol use despite adverse social, occupational, or health consequences. It is medically defined as a brain disease influenced by genetic, environmental, and psychological factors that are mild, moderate, or severe, according to a 2020 report on Alcohol’s effects on health by the National Institute of Alcohol Abuse and Alcoholism (NIAAA). Alcohol Use Disorder is referred to as alcohol abuse, alcohol dependence, alcohol addiction, and alcoholism.
According to the 2022 National Survey on Drug Use and Health and the Center for Behavioral Health Statistics and Quality’s 2022 study, 28.8 million adults aged 18 and older (11.2% of this age group) suffered from AUD in 2021. An estimated 753,000 adolescents ages 12 to 17 (2.9% of this age group) had AUD during this time frame.
The effects of Alcohol Use Disorder (AUD) lead to devastating long-term health consequences, including liver diseases such as cirrhosis and hepatitis, cardiovascular problems, psychiatric disorders such as depression and anxiety, and social problems including unemployment and relationship issues. The World Health Organization 2022 fact sheet on alcohol reveals Alcohol Use Disorder is the world’s third-largest risk factor for disease and mortality, responsible for an estimated 3 million deaths globally each year, representing 5.3% of all deaths. According to Dr Michael Olla, an addiction psychiatrist, treatment for alcohol use disorder includes a combination of therapies, medication, and support groups. Detoxification under medical supervision is the first step, followed by behavioral therapies like cognitive-behavioral therapy (CBT) and motivational enhancement therapy (MET). Medications such as naltrexone, acamprosate, and disulfiram are also used to help reduce drinking and prevent relapse. Support from organizations such as Alcoholics Anonymous (AA) offers a community-based approach to recovery, emphasizing peer support and accountability.
Tobacco and Nicotine Addiction

Tobacco or nicotine addiction, clinically referred to as tobacco use disorder, is a condition marked by the compulsive use of tobacco products, primarily driven by the body’s dependence on nicotine. This chemical is highly addictive, affecting the same brain pathways as heroin and cocaine. The Centers for Disease Control and Prevention (CDC) 2020 report highlights that nicotine addiction is the most prevalent form of chemical dependence in the United States. It alters brain chemistry, making quitting smoking exceptionally challenging.
The health impacts of nicotine addiction are severe and widespread, affecting nearly every organ in the body. It is particularly detrimental to the cardiovascular and respiratory systems, leading to diseases such as chronic obstructive pulmonary disease (COPD) and heart disease. According to the World Health Organization (WHO, 2021), tobacco use causes more than 8 million deaths per year worldwide, including both smokers and non-smokers exposed to second-hand smoke. Cigarette smoking alone kills more than 480,000 Americans each year, according to the U.S. Department of Health and Human Services Office on Smoking and Health 2014 research.
Addressing nicotine addiction requires a multi-pronged treatment approach that includes Nicotine Replacement Therapy (NRT) products like gums, patches, and lozenges, which are commonly used to mitigate withdrawal symptoms and decrease the urge to smoke. Non-nicotine medications such as bupropion and varenicline have also been effective in helping individuals quit by targeting the brain’s nicotine receptors.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
Opioid Addiction/Opioid Use Disorder

Opioid addiction is a severe medical condition characterized by an uncontrollable urge to use opioid drugs despite harmful consequences to one’s health and well-being. Opioids, which include both illegal drugs like heroin and prescription pain relievers such as oxycodone and morphine, act on the nervous system to produce pain-relieving and euphoric effects. According to the National Institute on Drug Abuse (NIDA, 2020), opioid addiction disrupts significant aspects of life, leading to physical and psychological dependence that requires more than willpower to overcome.
The opioid epidemic has become a public health crisis, especially in the United States. The Centers for Disease Control and Prevention (CDC, 2022) reports that nearly 70,000 Americans died from opioid-related overdoses in 2021 alone. This statistic highlights the urgent need for effective intervention strategies and broader public awareness about the dangers of opioid misuse.
The health consequences of opioid addiction are profound and life-threatening. Chronic use leads to nausea, constipation, respiratory depression, and psychological disorders such as depression and anxiety. Treatment for opioid use disorder is comprehensive and includes both medications and behavioral counseling. Medication-assisted treatment (MAT) is considered the gold standard, using medications such as methadone, buprenorphine, and naltrexone to reduce withdrawal symptoms and cravings. These treatments are most effective when combined with behavioral therapies that address the underlying causes of addiction, according to the Substance Abuse and Mental Health Services Administration (SAMHSA, 2022). Support groups and community resources also play a crucial role in recovery, providing ongoing support to prevent relapse.
Benzodiazepines Addiction
Benzodiazepine addiction develops through compulsive use of medications like diazepam, lorazepam, and alprazolam, commonly prescribed for anxiety and insomnia. Research shows dependency forms within 2-4 weeks, particularly with high doses or extended use.
Physical symptoms include drowsiness, confusion, and impaired coordination, while psychological effects manifest as cravings and tolerance development. According to CDC data, 16% of opioid overdose deaths involve benzodiazepines, highlighting their danger.
According to Maust, D. T.’s 2019 study, ‘Benzodiazepine Use and Misuse Among Adults in the United States.’, 30.6 million US adults (12.6%) reported past-year benzodiazepine use, with 25.3 million using as prescribed and 5.3 million reporting misuse, accounting for 17.2% of overall use. The highest prescribed use was among ages 50-64 (12.9%), while ages 18-25 had the highest misuse rate (5.2%). Notably, benzodiazepine misuse is strongly associated with prescription opioid and stimulant misuse/dependence, highlighting key risk factors for this behavior.
Treatment strategies for benzodiazepine addiction require medical supervision during detox, followed by behavioral therapy and counseling to address underlying causes. Alternative medications are prescribed for anxiety management while addressing co-occurring disorders, which remains crucial for successful recovery.
Barbiturates Addiction
Barbiturate addiction is a dangerous dependence on sedative-hypnotic drugs that affects the central nervous system, causing relaxation and euphoria. These substances pose a significant overdose risk and trigger severe withdrawal symptoms when stopped. Though modern medicine has largely replaced barbiturates with safer alternatives, they remain hazardous for those accessing them illegally or through outdated prescriptions.
The addiction creates both physical and psychological dependence, with the body developing tolerance and experiencing withdrawal when usage stops. Sudden discontinuation is life-threatening, potentially causing seizures and delirium. Chronic use leads to cognitive decline, severe mood changes, and organ damage.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, 2021 study, ‘Barbiturates. In LiverTox: Clinical and Research Information on Drug-Induced Liver Injury.’, phenobarbital is the most dangerous barbiturate due to its potential to cause severe hypersensitivity reactions, including DRESS syndrome, Stevens-Johnson syndrome, and toxic epidermal necrolysis, which is life-threatening and require immediate medical intervention.
Professional medical supervision is essential for barbiturate addiction treatment, requiring carefully monitored detoxification and comprehensive therapy to address root causes. Given the risks of fatal withdrawal complications, recovery must occur under strict medical oversight in appropriate healthcare settings.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
Stimulant Addiction
Stimulant addiction refers to the compulsive use of substances that increase activity in the brain and nervous system, enhancing alertness and energy. Common stimulants include prescription medications such as amphetamines (Adderall, Ritalin) and illicit drugs like cocaine and methamphetamine. As noted in the National Institute on Drug Abuse’s 2020 report, stimulants significantly affect neurotransmitters in the brain, which contributes to the high potential for addiction and abuse.
The use of stimulants leads to severe psychological and physical health issues. Psychologically, it causes paranoia, increased aggression, and, in some cases, severe mental health disorders like psychosis. Physically, stimulants raise heart rate and blood pressure, which leads to cardiovascular problems, including heart attacks, as mentioned in a study published by the American Heart Association in 2021. Chronic use also results in neurological damage and a decline in physical health due to malnutrition and lack of sleep.
Treating stimulants like cocaine and methamphetamine addiction involves a combination of pharmacological and behavioral interventions. There are currently no FDA-approved medications to treat addiction to cocaine or methamphetamine, making behavioral therapies like cognitive-behavioral therapy and contingency management crucial, as highlighted in the Substance Abuse and Mental Health Services Administration’s 2022 guidelines on behavioral health treatments. Support groups and inpatient or outpatient treatment programs also provide necessary support for stimulant abuse, as these environments help prevent relapse and address the underlying causes of addiction.
Cannabis and Marijuana Addiction

Cannabis addiction, termed cannabis use disorder or marijuana use disorder, is characterized by the compulsive use of cannabis despite adverse consequences in personal, professional, or social contexts. According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), as referenced in a 2022 report by the National Institute on Drug Abuse (NIDA), cannabis addiction is increasingly prevalent due to higher potency strains and greater societal acceptance.
Long-term cannabis use leads to significant health issues, including respiratory problems from smoking, altered brain development in younger users, and cognitive impairments affecting memory and attention. A 2021 study by the American Psychological Association highlights that chronic users might experience mental health problems such as anxiety and depression and, in some cases, the onset of psychosis.
The treatment of marijuana addiction typically involves behavioral therapies, as there are no FDA-approved medications for its treatment. Cognitive-behavioral therapy (CBT), motivational enhancement therapy (MET), and support groups are effective in managing withdrawal symptoms and reducing cannabis use. The Substance Abuse and Mental Health Services Administration (SAMHSA, 2023) underscores the importance of tailored treatment plans that address both psychological and behavioral aspects of addiction.
Hallucinogen Addiction
Hallucinogen addiction encompasses the habitual use of substances like LSD, psilocybin, and MDMA that alter perceptions, thoughts, and emotions. Hallucinogens do not cause physical dependency but create psychological dependence. The National Institute on Drug Abuse (NIDA, 2020) states that frequent hallucinogen use leads to tolerance, requiring higher doses for the same effects.
Hallucinogens profoundly impact mental health. Users experience intense, distressing alterations in perception, mood, and thought, known as hallucinogen-persisting perception disorder (HPPD), according to findings in the Journal of Psychopharmacology (2022). Risky behaviors during hallucinogenic experiences result in accidents and injuries. Treatment for hallucinogen addiction is supportive and psychotherapeutic since there are no specific medications to counteract the effects of hallucinogens. Psychological support, such as psychotherapy and counseling, is critical in helping individuals understand and change their substance use behaviors. Group therapy also provides peer support and decreases the stigma associated with addiction, as detailed by the American Psychiatric Association’s practice guidelines (2021).
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
Prescription Drugs addiction
Prescription drug addiction involves the compulsive use of medications prescribed by a doctor, taken in a way or for reasons not intended by the prescriber. This includes taking someone else’s medication, taking a higher dose than prescribed, or using the medication for its euphoric or calming effects.
According to Zajacova, A.’s 2023 study, ‘Prevalence and correlates of prescription opioid use among US adults, 2019-2020.’, 11.9% of the general population used prescription opioids, with rates increasing to 29.3% among those with chronic pain and 41.2% among those with high-impact chronic pain. The South showed 40% higher usage rates than the Northeast, while prescription opioid use declined by 9% from 2019 to 2020. Usage was higher among women, adults aged 45-64, and those experiencing food insecurity or unemployment, while lower rates were observed among immigrants and uninsured individuals. No significant differences were found between rural and urban areas.
Prescription drug addiction develops with various prescription drugs, including opioid painkillers like oxycodone, stimulants like Adderall, and sedatives like Xanax. Prescription drugs, even when used as directed, lead to physical dependence. Misuse of prescription drugs significantly increases the risk of addiction. Abruptly quitting triggers unpleasant or dangerous withdrawal symptoms, depending on the drug and the level of dependence. Long-term misuse of prescription drugs results in serious health consequences that affect various organs and systems in the body.
Treatment for prescription drug addiction requires a multifaceted approach. This includes medically supervised detoxification, especially for opioids and sedatives, to manage withdrawal symptoms safely. Therapy, support groups, and relapse prevention strategies are also crucial components of a comprehensive treatment plan, addressing the underlying causes of addiction and helping individuals develop coping mechanisms to maintain long-term recovery.
Inhalant Addiction
Inhalant addiction involves the compulsive use of volatile substances that produce chemical vapors, which are inhaled to induce psychoactive effects. This form of addiction is particularly dangerous due to the toxic nature of the substances involved. The National Institute on Drug Abuse (NIDA, 2020) categorizes inhalants as among the most harmful substances, especially to adolescents, who make up the majority of users.
Inhalants cause immediate and severe damage to the heart, kidneys, brain, and liver. The American Medical Association (AMA, 2021) reports that sudden sniffing death syndrome is a significant risk resulting from heart failure following abuse of inhalants. Chronic exposure also leads to long-term cognitive deficits and neurological damage.
Treatment strategies for inhalant addiction include detoxification, medical management of withdrawal symptoms, and extensive rehabilitation programs. Because inhalant withdrawal is particularly severe, close medical supervision is advised during detox. Behavioral interventions, including cognitive-behavioral therapy and family counseling, play essential roles in treatment plans, helping to address the root causes of addiction and promote long-term recovery, as per the guidelines from the American Society of Addiction Medicine (ASAM, 2023).
What Are the Most Commonly Used Drug Addiction Screening Tests?
The most commonly used drug addiction screening tests are DAST-10, CRAFFT, SBIRT, Urine Drug Test (UDT), NIDA Quick Screen, and more.
Drug addiction screening tests are tools used to identify individuals who are struggling with substance use disorders. These tests help healthcare professionals evaluate the extent of substance use and determine the appropriate level of care. Below are some of the most widely used drug addiction screening tests, along with their definitions, processes, and usages.
Are you covered for treatment?
Valley Spring Recovery Center is an approved provider for Blue Cross Blue Shield and Cigna, while also accepting many other major insurance carriers.
Check Coverage Now!DAST-10

The Drug Abuse Screening Test (DAST-10) is a brief, self-report tool used to screen for drug abuse or dependence in adults.
Patients answer 10 yes-or-no questions related to drug use in the past year. The questions cover various aspects of substance use, including its impact on social, occupational, psychological, and physical functioning.
The Drug Abuse Sreening Test (DAST-10) is widely used in clinical settings to quickly assess the likelihood of drug abuse problems. It helps identify individuals who may benefit from further evaluation or intervention.
CRAFFT

The CRAFFT Screening Test is a brief, behavioral health screening tool for adolescents to assess high-risk alcohol and other drug use disorders.
The test consists of six questions designed to identify risky behaviors and the consequences of substance use. It includes an acronym (Car, Relax, Alone, Forget, Friends, Trouble) to remind clinicians of the questions.
CRAFFT is commonly used in schools, pediatric offices, and primary care settings to detect early signs of drug abuse among adolescents and young adults.
SBIRT

Screening, Brief Intervention, and Referral to Treatment (SBIRT) is a comprehensive, integrated approach to the delivery of early intervention and treatment services for persons with substance use disorders.
SBIRT involves three steps: Screening using standardized tools, Brief Intervention to provide feedback and advice, and Referral to Treatment for those who need specialized care.
SBIRT is implemented in various healthcare settings, including emergency departments, primary care offices, and community clinics, to identify and intervene with patients at risk for drug abuse.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
Urine Drug Test (UDT)

Urine Drug Tests (UDTs) are laboratory analyses of a urine sample to detect the presence of drugs and their metabolites.
A urine sample is collected and analyzed using immunoassay screening followed by confirmatory tests, such as gas chromatography-mass spectrometry (GC-MS) or high-performance liquid chromatography (HPLC).
UDTs are widely used in clinical and forensic settings, including workplace drug testing, addiction treatment monitoring, and criminal justice cases.
NIDA Quick Screen

The National Institute on Drug Abuse (NIDA) Quick Screen is a brief screening tool designed to identify substance use disorders in primary care settings.
Patients are asked a series of questions about their use of tobacco, alcohol, illicit drugs, and prescription drugs for non-medical reasons in the past year.
The NIDA Quick Screen is used to quickly identify patients who may need further assessment or intervention for substance use disorders.
CAGE Questionnaire
The CAGE Questionnaire is a brief, four-item screening tool used to identify potential alcohol problems.
Patients are asked four questions about their drinking habits: Have you ever felt you should Cut down on your drinking? Have people Annoyed you by criticizing your drinking? Have you ever felt Guilty about drinking? Have you ever had a drink first thing in the morning (an Eye-opener)?
The CAGE Questionnaire is commonly used in primary care and mental health settings to quickly screen for alcohol use disorders.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
MAST
The Michigan Alcohol Screening Test (MAST) is one of the oldest and most widely used tools for detecting alcohol dependency.
The MAST consists of 22 questions about the patient’s drinking behavior and its impact on their life. Responses are scored to determine the likelihood of an alcohol use disorder.
The MAST is used in both clinical and research settings to identify individuals with alcohol dependency and to assess the severity of their condition.
What Are Treatments for Drug Addiction?

Treatment for drug addiction encompasses a range of approaches like detox, inpatient rehab, hospitalization, outpatient treatment, telehealth, therapy, Intensive outpatient programs, and more. These addiction treatments are designed to help individuals stop using drugs and address mental, physical, and behavioral symptoms to achieve lasting recovery and sobriety.
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), effective treatment addresses multiple needs of the individual, not just their drug use. Below are the common types of drug addiction treatment options offered by drug and alcohol rehab centers, along with their definitions, advantages, disadvantages, and typical usage durations, enhanced with the ASAM Criteria guidelines on levels of care.
1. Medical Detox
Medical detox is the initial phase of addiction treatment, where substances are safely removed from the body under medical supervision. This process ensures physical stabilization, manages severe withdrawal symptoms, and prepares individuals for further therapeutic interventions. The importance of medical detox cannot be overstated, as withdrawal symptoms are severe and even life-threatening. The ASAM Criteria defines this level of treatment intensity as Level 4: Medically Managed Intensive Inpatient Services, which provides 24-hour medically directed evaluation and care.
The advantages of medical detox include physical stabilization, managing severe withdrawal symptoms, and preparing individuals for further treatment.
The disadvantages of medical detox are that it does not address the psychological aspects of addiction and needs to be followed by other treatments.
Medical detox typically lasts from a few days to two weeks, depending on the substance being abused and co-morbidities.
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
2. Inpatient Rehab
Inpatient rehab involves residential treatment where patients stay at a facility and receive intensive care. This type of treatment provides structured support, a sense of community, and comprehensive care that includes therapy, medical observation, detoxification, and holistic treatments. The controlled environment allows for constant monitoring and immediate intervention, which is beneficial for physical, mental, and emotional recovery. The ASAM Criteria include Level 3.7: Medically Monitored Intensive Inpatient Services and Level 3.5: Clinically Managed High-Intensity Residential Services.
The advantages of inpatient rehab are the comprehensive and continuous care provided, which is crucial for individuals with severe addictions.
The disadvantages of inpatient rehab include its cost and the requirement for patients to take time away from home, work, or school.
The duration of inpatient rehab varies based on the individual’s needs and progress, generally lasting from 30 to 90 days.
3. Partial Hospitalization Program (PHP)
A Partial Hospitalization Program (PHP), also known as “day treatment,” offers high-level medical and therapeutic care while allowing patients to live at home. PHP is an intensive form of outpatient care that provides a balance between treatment and daily life, making it ideal for individuals who need significant support but have a stable home environment. The ASAM Criteria defines this as Level 2.5: Partial Hospitalization Services, which provides 20 or more hours of service per week.
The advantages of PHP include receiving intensive care without overnight stays, which allows for a balance between treatment and daily life.
The disadvantages of PHP include the requirement for a strong support system at home, making it unsuitable for individuals with unstable living conditions.
PHP typically involves several hours of treatment per day, 3-5 days a week, for a few weeks to months.
4. Outpatient Treatment
Outpatient treatment provides therapy and counseling services without requiring patients to stay overnight at a facility. This flexible option is suitable for individuals who have a strong support system at home and need to continue with their daily responsibilities while receiving treatment. The ASAM Criteria defines this as Level 1.0: Outpatient Services, which provides less than 9 hours of service per week, and Level 1.5: Outpatient Therapy.
The advantages of outpatient treatment include a flexible schedule that accommodates work, school, and family commitments.
The disadvantages of outpatient treatment include its lower intensity, which is not suitable for severe addictions.
Outpatient treatment ranges from a few months to a year, with varying frequencies of therapy sessions.
Are you covered for treatment?
Valley Spring Recovery Center is an approved provider for Blue Cross Blue Shield and Cigna, while also accepting many other major insurance carriers.
Check Coverage Now!5. Telehealth
Telehealth is a delivery method for IOP and Outpatient treatment that takes place through online therapy sessions and consultations with healthcare providers. This approach makes treatment accessible from any location, which is especially beneficial for those with mobility issues or who live in remote areas.
The advantages of telehealth include its accessibility from any location, making it convenient for individuals with mobility issues or those residing in remote areas.
The disadvantages of telehealth include the lack of physical presence, which limits effectiveness for some individuals.
The duration of telehealth treatment for addiction varies based on individual needs and program structure.
6. Intensive Outpatient Program (IOP)
An Intensive Outpatient Program (IOP) provides a higher level of care than standard outpatient programs, with more frequent and longer therapy sessions. IOP is designed for individuals who need significant support but do not require 24/7 supervision. The ASAM Criteria defines this as Level 2.1: Intensive Outpatient Services, which provides 9 or more hours of service per week, and Level 2.7: Medically Managed Intensive Outpatient Services.
The advantages of IOP include intensive support while allowing patients to maintain daily responsibilities.
The disadvantages of IOP include the requirement for a high level of commitment and time management from the patient.
IOP drug rehab involves 9 or more hours of service per week through multiple sessions, lasting several hours each, over weeks to months.
7. Therapy
Therapy in addiction treatment includes individual, group, and family therapy sessions. These sessions address the psychological aspects of addiction, help develop coping skills, and foster support networks.
The advantages of therapy include addressing underlying issues contributing to addiction and providing tools for long-term recovery.
The disadvantages of therapy include slow progress and the need for active participation and honesty, which is challenging for some individuals.
Therapy is ongoing and continues for several months to years as part of aftercare, depending on the individual’s needs and progress.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
8. Holistic Treatment
Holistic treatment incorporates non-traditional therapies such as acupuncture, yoga, meditation, and art therapy. These treatments aim to treat the whole person, promoting overall well-being and stress reduction.
The advantages of holistic treatment include its comprehensive approach to health, addressing physical, mental, and emotional well-being.
The disadvantages of holistic treatment include the lack of scientific evidence for some holistic methods and potential issues with insurance coverage.
Holistic treatments are integrated into other treatment programs or used as supplementary treatments, with the duration varying based on individual needs.
9. Aftercare
Aftercare programs offer ongoing support and resources to maintain sobriety post-treatment. These programs are crucial for reducing the risk of relapse, providing a support network, and continuing skill-building for long-term recovery.
The advantages of aftercare include providing ongoing support, which helps individuals stay committed to their recovery.
The disadvantages of aftercare include the need for continuous commitment, which is challenging to maintain over time.
Aftercare typically involves regular meetings and support sessions, potentially lasting for several years
10. Recovery Residences
Recovery residences, referred to as sober living or transitional living homes, provide safe and healthy living environments that promote recovery from alcohol and other drug use. These are not formal treatment programs but offer peer support and accountability in a sober living environment.
The advantages of recovery residences include providing a supportive community, fostering accountability, and helping individuals transition back into daily life.
The disadvantages of recovery residences include not being a substitute for formal treatment programs and the potential requirement for residents to follow specific rules and guidelines.
The duration of stay in recovery residences varies from a few months to several years, depending on individual needs and progress.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
How Does Medication Play a Role in Treating Addiction and What is Medication-Assisted Treatment (MAT)?
Medications play a critical role in the treatment of drug addiction, primarily used to manage withdrawal symptoms, prevent relapse, and address co-occurring mental health conditions.
Medication-assisted treatment (MAT) combines the use of FDA-approved medications with counseling and behavioral therapies. This approach aims to treat the whole patient, addressing both the physical and psychological aspects of addiction.
MAT helps normalize brain chemistry, blocks the euphoric effects of alcohol and opioids, alleviates physiological cravings, and stabilizes body functions. It is particularly effective for opioid use disorder, alcohol use disorder, and smoking cessation.
Medications Used in MAT:
- Opioid Addiction:
- Methadone: Reduces cravings and withdrawal symptoms, taken daily under medical supervision.
- Buprenorphine: Partial opioid agonist that reduces cravings and withdrawal symptoms, with a lower risk of misuse.
- Naltrexone: Blocks the euphoric and sedative effects of opioids, preventing relapse.
- Alcohol Addiction:
- Disulfiram: Causes unpleasant reactions when alcohol is consumed, deterring individuals from drinking.
- Acamprosate: Helps maintain abstinence by reducing the desire to drink.
- Naltrexone: Reduces alcohol cravings and the pleasurable effects of drinking.
- Nicotine Addiction:
- Nicotine Replacement Therapy (NRT): Patches, gum, and lozenges that provide a controlled dose of nicotine to ease withdrawal symptoms.
- Bupropion: A non-nicotine medication that helps reduce cravings and withdrawal symptoms.
- Varenicline: Reduces cravings and withdrawal symptoms by targeting nicotine receptors in the brain.
What Are The Benefits Of Medication-assisted Treatment (Mat)?
The Benefits Of Medication-assisted Treatment (MAT) include essential biochemical stabilization, effective withdrawal management, and enhanced recovery focus. MAT offers comprehensive support through craving reduction, relapse prevention mechanisms, and treatment of co-occurring mental health conditions. These evidence-based interventions demonstrate improved retention rates, decreased substance use, and better employment outcomes.
Here are the benefits of Medication-Assisted Treatment (MAT) in detail below:
- Biochemical Support: MAT provides essential biochemical support to help patients stabilize physically and mentally during the early phases of recovery. By managing withdrawal symptoms and cravings, MAT enables individuals to focus on their recovery process without the constant distraction of physical discomfort.
- Relapse Prevention: Medications used in MAT, such as naltrexone for opioid and alcohol addiction, block the euphoric effects of these substances. This reduces the incentive to relapse, as the individual no longer experiences the same “high” from substance use.
- Treatment of Co-occurring Conditions: Many individuals with substance use disorders also suffer from co-occurring mental health conditions such as depression, anxiety, or PTSD. Medications used in MAT help address these conditions, providing a more holistic approach to treatment.
- Improved Outcomes: Research shows that MAT increases retention in treatment programs, decreases illicit opioid use, reduces criminal activity, and improves patients’ ability to gain and maintain employment. By addressing both the physical and psychological aspects of addiction, MAT contributes significantly to long-term recovery and overall well-being.
Medication-assisted treatment (MAT) plays a vital role in managing addiction. MAT integrates medications with counseling and behavioral therapies, addressing the complex interplay of physical dependence and psychological issues in substance use disorders. This approach stabilizes individuals during critical early recovery stages and supports long-term success by reducing relapse risk and improving overall mental health.
What Are The Addiction Statistics?
The drug addiction statistics in the United States have grown monumentally since 2020. Here are the key drug addiction statistics that reveal alarming trends across communities and industries in the United States:
- According to Bush, D. M., & Lipari, R. N.’s 2015 study, ‘Substance Use and Substance Use Disorder by Industry.’, In the workplace, 9.5% of full-time workers aged 18 to 64 reported having a substance use disorder (SUD) in the past year. This prevalence varies significantly across industries, with the accommodations and food services industry having the highest rate at 16.9%. In contrast, the lowest rates were found in education, health care, social assistance, and public administration sectors. The study also found that 8.7% of workers used alcohol heavily, with mining (17.5%) and construction (16.5%) industries showing the highest rates. Additionally, 8.6% used illicit drugs, with the highest rate (19.1%) in the accommodations and food services industry. The economic impact of substance use negatively affects U.S. industry through lost productivity, workplace accidents and injuries, employee absenteeism, low morale, and increased illness.
- According to Substance use & substance use disorders. In CDC Yellow Book 2024, in 2020, 40.3 million people aged 12 or older in the United States (14.5% of this population) reportedly had a substance use disorder (SUD) in the past year.
- According to the White House drug addiction statistics, addiction is responsible for $120 billion in lost productivity and $11 billion in healthcare costs alone. Health and Human Services states the annual economic impact of substance misuse is estimated to be $249 billion for alcohol misuse and $193 billion for illicit drug use.
What Are The Risks Of Drug Overdose as a Result of Drug Abuse?
The risks of overdosing on drugs are both significant and devastating, highlighted by escalating trends and sobering statistics that underscore the persistent challenge of drug overdose in the United States. According to the National Vital Statistics System, drug overdose deaths continue to rise, with a 14% increase from 2020 to 2021, resulting in 106,699 fatalities in the latter year. The pervasive impact of opioids, especially synthetic opioids other than methadone, remains the primary catalyst for these deaths, accounting for approximately 75.4% of all drug overdose fatalities in 2021.
Key Points on Drug Overdose Risks:
- Opioid Epidemic: In 2021, opioids were involved in 80,411 deaths, with synthetic opioids being the predominant factor. This category of drugs significantly influences the high rates of overdose deaths, reflecting their potent nature and widespread misuse.
- Increasing Rates with Psychostimulants: There is also an alarming increase in overdose deaths involving psychostimulants such as methamphetamine, compounded by the concurrent use of synthetic opioids.
- Impact of the COVID-19 Pandemic: The pandemic exacerbated the overdose crisis, contributing to a 30% spike in drug overdose deaths from 2019 to 2020. Factors such as increased stress, anxiety, and isolation have intensified substance use and the consequent risk of overdose.
- Preventability: A notable 92% of drug overdose deaths could potentially be prevented through measures like timely administration of naloxone, improved prescription practices, and vigilant monitoring of drug use.
- Demographic Vulnerabilities: The data reveals that middle-aged men are disproportionately affected, being more than twice as likely to die from a drug overdose compared to women. Among women, the highest number of overdose deaths occurs in the 44 to 54-year age group.
- Regional Variations: There have been significant regional fluctuations in overdose death rates, with marked increases in states like Washington, Oregon, Alaska, and Nevada and decreases in North Carolina, Wisconsin, Florida, and Georgia between 2022 and 2023.
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
What Does Drug Addiction Do To The Brain?
altering its reward, cognitive, and emotional circuits. Initially, substances with addictive potential hijack the brain’s reward system, flooding it with dopamine—a neurotransmitter linked to pleasure and reinforcement. It’s important to understand the science of drug addiction and the brain because the dopamine surge from ingesting drugs not only induces an intense feeling of euphoria but also reinforces the drug-taking behavior, setting the stage for a vicious cycle of addiction. Over time, the brain adapts to these dopamine spikes by reducing the responsiveness of the neural cells in the reward circuit, a phenomenon known as ‘tolerance.’
This adaptation diminishes the individual’s ability to derive pleasure from other life-affirming activities, such as social interaction, eating, or sexual activity, thereby narrowing their sources of pleasure to the drug itself. Moreover, long-term drug use extends its damaging effects to other neural circuits, impairing cognitive functions like learning, judgment, and decision-making while also affecting emotional regulation and stress response, which further differentiates a drug-addicted brain from a normal brain. Despite being cognizant of these adverse outcomes, the individual finds themselves ensnared in a self-perpetuating cycle of drug abuse, epitomizing the paradoxical and self-destructive nature of addiction.
How Do Drugs Interact With The Brain To Cause Addiction?
Drugs interact with the brain to cause addiction by targeting the brain’s reward system, flooding it with dopamine. This leads to repeated use, eventually causing changes in neural circuits that result in addiction. The brain’s reward center becomes used to receiving the dopamine spike that occurs when drugs are received into the system, making it harder and harder to stop, resulting in increased dependence.
frequently asked questions (FAQs) about Addiction
What is the Relationship Between Addiction and Mental Health?
The relationship between addiction and mental health reveals a complex interplay of psychological, biological, and social factors like concurrent mental health conditions, genetic predispositions, self-medicating behaviors, treatment complexities, and recovery hurdles. These interconnected elements demonstrate how mental wellness and substance use challenges often influence and reinforce each other, creating a cycle that requires comprehensive care and understanding. Here’s an in-depth look at this relationship:
-
Co-Occurrence: Mental health disorders and addiction often co-occur. This means that individuals struggling with addiction might also have one or more mental health conditions, such as depression, anxiety, or bipolar disorder, and vice versa.
-
Shared Risk Factors: Both mental health and addiction have shared genetic, environmental, and biological risk factors. For example, genetic predisposition, trauma, and chronic stress can increase the likelihood of both mental illness and addiction.
-
Cause and Effect: In some cases, mental health disorders might contribute to addiction. A person suffering from anxiety or depression has a higher liklihood of turning to drugs or alcohol as a form of self-medication. Conversely, chronic substance abuse can lead to mental health issues, as the effects of drugs and alcohol can alter brain chemistry and exacerbate underlying mental health symptoms.
-
Impact on Treatment: The interconnection between mental health and addiction necessitates an integrated approach to treatment. Treating one condition without addressing the other can hinder recovery. Dual-diagnosis treatment centers provide comprehensive care that addresses both mental health and substance abuse disorders simultaneously.
-
Recovery Challenges: The overlapping nature of mental health and addiction can make recovery more challenging. Symptoms of mental health disorders might trigger cravings and relapse, while withdrawal from substances might worsen mental health symptoms. Ongoing support and specialized care tailored to the individual’s specific needs are crucial.
-
Prevention and Early Intervention: Understanding the link between mental health and addiction emphasizes the importance of early intervention and prevention. Addressing mental health symptoms early, providing support, education, and therapy, can reduce the risk of developing an addiction.
-
Social and Societal Factors: Stigma surrounding both mental health and addiction can create barriers to seeking help. Encouraging open dialogue, reducing stigma, and providing accessible services are essential for supporting those affected by these interconnected issues.
How Does Addiction Impact the Workplace?
Addiction impacts the workplace through multiple significant channels, primarily leading to increased absenteeism, decreased productivity, and elevated healthcare costs across various industries. Laws addressing workplace substance abuse differ by jurisdiction, encompassing drug-free workplace policies, drug testing protocols, and Employee Assistance Programs (EAPs). Organizations must carefully balance their employees’ privacy rights while ensuring a safe and productive work environment, making legal compliance a critical priority.
How Do Family Dynamics Influence Addiction?
Family dynamics and relationships significantly influences an individual’s susceptibility to addiction. Dysfunctional family patterns, such as neglect, abuse, or lack of communication, increase the risk. In contrast, strong family support can be a powerful aid in recovery. Family therapy is often incorporated into treatment plans, allowing family members to understand addiction better and learn how to support their loved one effectively.
What is the Role of Support Groups in Addiction Recovery?
Support groups play a vital role in addiction recovery by providing a sense of community, empathy, encouragement, and accountability through organizations like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA). These groups create a non-judgmental space where individuals can share experiences and support one another on their recovery journey. The role of these support systems proves essential in maintaining sobriety and offers continuous care after formal treatment has ended.
How Does Addiction Affect Pregnancy?
Addiction during pregnancy can have serious health effects on both the mother and the unborn child, including preterm birth, low birth weight, developmental problems, and neonatal abstinence syndrome. Treatment for pregnant women with addiction often requires specialized care, focusing on both the mother’s health and the child’s development, including counseling, medical supervision, and carefully managed detoxification if necessary.
What Are the Cultural and Societal Influences on Addiction?
Cultural norms, societal pressures, and stigma can shape individual and community attitudes towards addiction. These influences affect prevalence, perception, treatment, and recovery. Understanding and addressing these factors requires a holistic approach to addiction, recognizing its complexity, and considering cultural competence and sensitivity in treatment and prevention efforts.
What Are the Latest Innovations in Addiction Treatment?
The latest innovations in addiction treatment include personalized therapy plans based on genetic and behavioral analysis, medication-assisted treatment that reduces cravings, telemedicine for remote access to care, and holistic approaches that integrate physical, mental, and spiritual wellness. These innovative solutions aim to provide more effective and accessible care tailored to the unique needs of each individual.
Who is Affected by Drug Addiction?
Drug addiction affects not just individuals but extends to families, workplaces, healthcare systems, and entire communities through emotional trauma, deteriorating relationships, reduced productivity, and increased societal costs. From strained family bonds and workplace disruptions to overwhelmed healthcare facilities and challenged law enforcement, substance abuse creates ripple effects across multiple social layers.
Drug addiction effects:
Family Members:
- Spouses, parents, and siblings endure emotional trauma and financial hardship
- Children suffer developmental and psychological challenges
- Extended family faces social stigma and relationship strain
Friends and Social Circles:
- Close friends experience betrayal of trust and emotional exhaustion
- Social relationships deteriorate due to unpredictable behavior
- Peer groups may struggle with enabling or codependency issues
Professional Environment:
- Employers face reduced workplace productivity
- Coworkers shoulder additional workload
- Business operations experience financial losses
Healthcare Infrastructure:
- Medical facilities manage increased patient load
- Emergency services handle addiction-related crises
- Treatment centers require expanded resources
Broader Society:
- Law enforcement deals with drug-related crimes
- Public health systems bear increased costs
- Communities face decreased safety and property values
Is Addiction a Disease or a Choice?
Addiction is a chronic relapsing disease of the brain. The subject is widely debated with many dissenting opinions, but according to doctors and medical research, drug addiction is a disease and not a choice. Drug addiction It’s characterized by compulsive substance use despite harmful consequences. While the initial decision to use a substance may be voluntary, repeated use can lead to changes in the brain that impair self-control and hamper the ability to resist cravings, making it a medical condition rather than a mere choice.
Not all behavioral addictions are classified as a disease though. The Diagnostic and Statistical Manual of Mental Disorders (DSM) recognized behavioral addictions for the first time in DSM-5 with gambling disorder, formerly pathological gambling, as the only non-substance-related disorder classified under the chapter of “Substance-Related and Addictive Disorders”.
What Are The Most Common Drug Addictions?
The most common drug addictions in the United States vary, with alcohol, nicotine, and marijuana topping the list due to their widespread legal status and social acceptance. Alcohol is particularly notable, with about 28.3 million people aged 12 or older reporting struggles with an alcohol use disorder as of 2020. Nicotine follows, with approximately 23.6 million Americans facing addiction, largely due to the legal status and accessibility of tobacco products. Marijuana also features prominently, with around 14.2 million Americans having a marijuana use disorder, a situation exacerbated by increasing legalization and social acceptability of the drug.
What Are The Most Expensive Illegal Drugs?
The most expensive illegal drugs are cocaine, heroin, and methamphetamine, with prices varying significantly based on their potency and associated risks. Cocaine ranks as the costliest, commanding $80 to $100 per gram due to high demand and trafficking dangers. Heroin stands as the second most expensive, priced at $15 to $20 per dose, largely due to its severe addiction potential and overdose risks. Methamphetamine prices range from $3 to $500 per dose, with cost variations depending on purity levels and form.
Where Is Addiction Treated?

Addiction is treated in diverse settings ranging from specialized facilities, hospitals, and community centers, utilizing evidence-based approaches like medical supervision, counseling, and therapeutic interventions. These treatment options include inpatient rehabilitation, outpatient programs, mental health clinics, and telehealth services, addressing both physical and psychological aspects of recovery.
Here is a comprehensive overview of the primary locations where addiction is treated:
- Inpatient Drug Rehabilitation Centers: Inpatient drug rehabilitation centers serve as the most conventional setting for addiction treatment. These facilities provide a structured environment with medical and psychological support. Inpatient centers include detoxification services, individual and group therapy, medication-assisted treatment, and aftercare planning. Residential rehab centers require individuals to reside on-site, while outpatient programs allow patients to live offsite.
- Hospital-Based Programs: Some hospitals offer specialized addiction treatment programs for cases requiring medical detoxification or co-occurring mental health conditions. Hospital-based programs provide a higher level of medical supervision compared to standard rehab centers.
- Mental Health Clinics: Specialized mental health clinics offer dual diagnosis treatment for individuals facing both addiction and mental health issues. These facilities provide integrated care that addresses both conditions simultaneously, improving long-term recovery chances.
- Community Health Centers: Community health centers deliver outpatient addiction treatment services, often at a lower cost. These centers provide medication-assisted treatment, counseling, and referral services for more intensive treatment if necessary.
- Telehealth Services: Telehealth services provide online platforms for addiction treatment, offering convenience for individuals unable to access traditional treatment centers due to geographical or financial constraints.
- Support Groups and 12-Step Programs: Organizations like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) offer peer-led support groups. While not substitutes for professional treatment, these groups provide beneficial supplementary support for many individuals.
- Holistic and Alternative Therapy Centers: Some individuals pursue holistic treatments such as acupuncture, yoga, and herbal medicine as adjunct therapies. While the efficacy of these methods remains under study, many individuals find them helpful in managing withdrawal symptoms and cravings.
Share This Post















