Alcoholic liver cirrhosis, also known as alcoholic cirrhosis, is an advanced stage of alcohol liver disease that occurs due to chronic alcohol abuse. This results in significant scarring and generally irreversible damage to the liver. The condition is influenced by oxidative stress, the immune response, gut microbiome changes, and genetics.
Alcoholic cirrhosis starts with fatty liver also known as steatosis, proceeds to steatohepatitis typified by liver inflammation, and culminates in alcohol cirrhosis characterized by excessive liver damage.
Signs and symptoms of alcohol liver disease are fatigue, weakness, abdominal pain, jaundice, dry mouth, dark urine, spider angiomas, and persistent thirst.
Diagnosing alcohol-induced liver cirrhosis involves health history intake, a physical exam, liver function tests, coagulation blood tests, imaging tests, and liver biopsy.
Treating alcohol-related cirrhosis involves abstinence from alcohol, detox, medication, psychotherapy, dietary, and lifestyle changes. In addition, social support from groups or services helps improve life expectancy and manage complications.
What is Alcohol Liver Cirrhosis?
Alcoholic liver cirrhosis or alcohol cirrhosis, refers to a severe condition marked by irreversible scarring of the liver as a result of long-term, excessive alcohol abuse. According to a 2023 study by Patel R, “Alcoholic Liver Disease”, by StatPearls Publishing, alcoholic liver cirrhosis is an advanced stage of alcoholic liver disease. At this stage, the damage to the liver is irreversible but if the person stops drinking alcohol, further damage is prevented.
Alcohol-induced liver damage starts with ethanol creating oxidative stress and the formation of acetaldehyde, which damages liver cells and triggers an inflammatory response. Continuous cell injury and destruction due to ongoing alcohol abuse leads to progressive fibrosis, as the liver’s regenerative capacity is unable to keep up which eventually leads to cirrhosis.
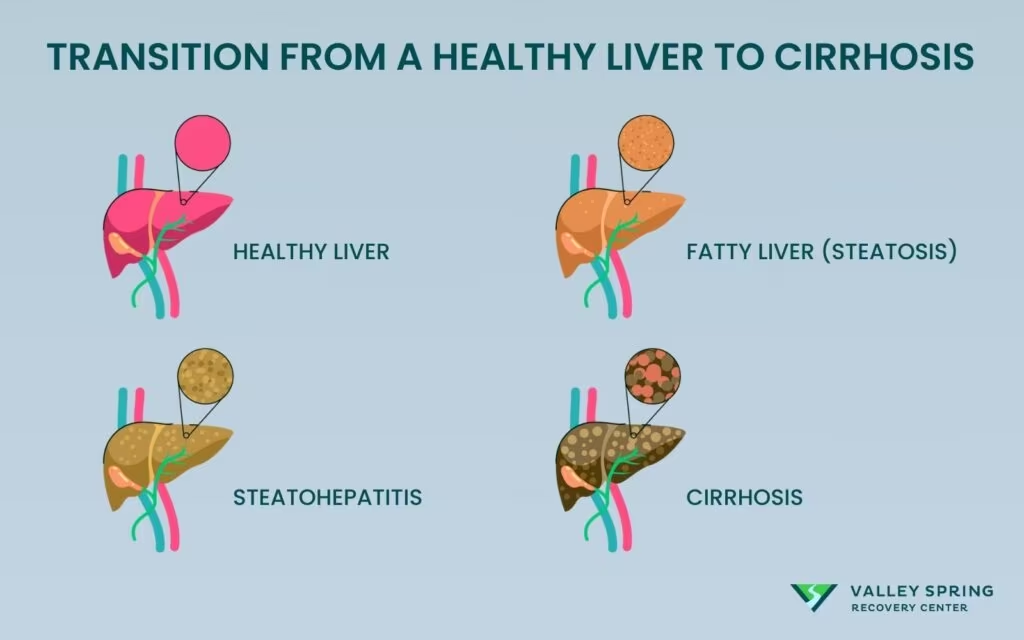
How Does The Condition Progress From a Healthy Liver to Cirrhosis?
The condition starts with fatty liver also known as steatosis, proceeds to steatohepatitis typified by liver inflammation, and culminates in alcohol cirrhosis characterized by excessive liver damage.
Alcohol abuse is a global healthcare concern. According to the article “Alcohol”, by the World Health Organization (WHO), alcohol consumption causes the deaths of 3 million people yearly around the world. It also contributes to poor health, and disabilities of many more. The WHO estimates that alcohol contributes to about 5.1 percent of the global sickness burden.
Alcohol-related liver disease usually develops over a long time. According to a 2017 study by Osna, N. A., “Alcoholic Liver Disease: Pathogenesis and Current Management”, published in the Alcohol Research: Current Reviews journal the process typically consists of four stages:
- Fatty liver (steatosis): It is marked by heavy accumulation of fats around liver cells (hepatocytes). At this stage, the condition is harmless as long as it does not proceed to the next phase.
- Steatohepatitis: This is the second stage involving inflammation of the liver. It occurs when the person continues with their alcohol-drinking behavior. At this stage, the liver is severely inflamed.
- Cirrhosis: This is the advanced stage of alcohol liver disease. Vascular alterations and excessive scaring of the liver typify it. If no intervention measures are taken, liver failure follows shortly.
Cirrhosis usually develops after a decade or more of alcohol abuse, often diagnosed around the age of 60. Interestingly, alcohol abusers concurrently present overlapping stages of liver disease due to long-standing alcohol abuse.
What Are The Symptoms of Alcohol Liver Disease?
Signs and symptoms of alcohol liver disease are fatigue, weakness, abdominal pain, jaundice, dry mouth, dark urine, spider angiomas, and persistent thirst.
The 2023 study by Patel lists symptoms of alcoholic cirrhosis as:
Early Symptoms
- Fatigue and Weakness: One of the earliest signs of cirrhosis is a general sense of tiredness and weakness. The fatigue is profound and often affects daily activities and overall quality of life.
- Poor Appetite and Weight Loss: Individuals experience a significant decrease in appetite, leading to unintended weight loss. This symptom is often coupled with nausea and vomiting, further contributing to malnutrition.
- Mild Pain or Discomfort: Discomfort or mild pain in the upper right side of the abdomen, where the liver is located, is another early sign. This pain is usually persistent and varies in intensity.
- Itchy Skin: Pruritus, or severe itching, is common and particularly bothersome. It results from the buildup of bile products in the skin due to impaired liver function.
- Muscle Loss and Cramps: As cirrhosis progresses, muscle wasting and cramps occur, further debilitating the patient.
- Sexual Problems: Men usually experience impotence, shrinking of the testicles, and swelling of the breasts (gynecomastia), while women notice irregular menstrual cycles.
Advanced Symptoms
As liver function deteriorates, more severe symptoms emerge, reflecting significant liver damage:
- Jaundice: This is characterized by a yellowing of the skin and the whites of the eyes due to the accumulation of bilirubin, a byproduct of the breakdown of red blood cells that the liver no longer processes effectively.
- Bruising and Bleeding Easily: The liver produces proteins that help in blood clotting. Damage to the liver impairs this function, leading to easy bruising and abnormal bleeding.
- Confusion and Cognitive Issues: Known as hepatic encephalopathy, this includes symptoms like confusion, memory loss, difficulty thinking clearly, personality changes, and sleep disturbances. It results from the liver's inability to detoxify substances that affect brain function.
- Ascites: This is the accumulation of fluid in the abdomen, causing noticeable swelling and discomfort. It results from portal hypertension, where increased pressure in the liver's blood vessels forces fluid to leak into the abdominal cavity.
- Edema: Swelling in the legs, ankles, and feet due to fluid retention is common, again due to impaired liver function and portal hypertension.
- Variceal Bleeding: Enlarged veins (varices) in the esophagus, stomach, or intestines burst and bleed, leading to potentially life-threatening internal bleeding.
- Dark Urine: Urine becomes darker as the liver's ability to process bilirubin declines, leading to its increased presence in the bloodstream and subsequently the urine.
- Pale or Clay-Colored Stools: This occurs due to the reduced excretion of bilirubin into the bile and the intestines, affecting stool color.
- Severe Itching: This symptom becomes more pronounced in advanced stages and is often a significant cause of discomfort for patients.
- Spider Angiomas: These are small, spider-like blood vessels visible under the skin, particularly on the upper body.
- Palmar Erythema: Redness of the palms is another symptom indicative of advanced liver disease.
- Hormonal Changes: In men, this includes impotence, testicular atrophy, and gynecomastia due to hormonal imbalances caused by liver dysfunction.
How is Alcoholic Cirrhosis Diagnosed?
Diagnosing alcohol-induced liver cirrhosis involves health history intake, a physical exam, liver function tests, coagulation blood tests, imaging tests, and liver biopsy.
1. Health History Intake
According to the 2003 study by Marsano, L. S., “Diagnosis and Treatment of Alcoholic Liver Disease and Its Complications”, published in the Alcohol Research & Health journal, diagnosing alcoholic cirrhosis involves a thorough health history intake, particularly regarding habitual alcohol abuse. In addition, the physician is also likely to conduct a physical exam, and liver function and coagulation blood tests
2. Imaging Tests
According to the article ”How to Diagnose Cirrhosis”, from the US Department of Veteran Affairs,
imaging studies such as abdominal ultrasound, CT scans, and MRIs are the commonly used techniques for detecting fatty build-up in the liver, splenomegaly (enlarged spleen), shrunken right lobe of the liver, and ascites. Among these, MRI provides the most accurate quantification of fatty build-up, enabling early intervention and potentially reversing the disease.
3. Liver Biopsy
The gold standard in diagnosing cirrhosis is a liver biopsy, which reveals key features such as regenerative nodules surrounded by fibrous bands. It’s often required for asymptomatic compensated cirrhosis, while those with decompensated cirrhosis showing symptoms do not always need a biopsy. Additional risk stratification in patients with suspected cirrhosis is provided by hepatic venous pressure gradient (HVPG) testing. This offers insights into the severity of portal hypertension and the impact of alcohol abstinence on disease progression.
What Are The Risk Factors For Developing Alcoholic Liver Disease
Risk factors for developing alcoholic liver disease include quantity, and quality of alcohol consumption, genetic background, gender, and lifestyle choices.
1. Quantity And Duration Of Alcohol Consumption
According to the 2023 study by Patel, the quantity and duration of alcohol consumption rank highest among the risk factors for developing alcoholic liver disease. Binge drinking, which refers to the habit of drinking more than 4 to 5 drinks in a row at least once in 7 days, causes the accumulation of fats in the liver, leading to alcohol cirrhosis. It’s important to note that around 20% to 25% of heavy drinkers develop alcoholic cirrhosis, contributing significantly to cirrhosis-related deaths globally.
2. Lifestyle choices
Lifestyle choices like sedentary life, leading to obesity and high-fat diets, along with coexisting conditions such as type 2 diabetes increase the risk of developing alcohol-related liver disease.
- Obesity and high-fat diet: According to the article “Alcohol-Related Liver Disease”, from the University of Michigan Health, obesity, being overweight, and eating a high-fat diet increase the risk of developing alcohol liver disease due to a build-up of fat in the liver. Normally, fat cells produce acids which cause reactions and eventually destroy healthy liver cells.
- Malnutrition: Chronic alcohol abusers often experience malnutrition because alcohol reduces the body’s ability to absorb nutrients. In addition, most alcohol abusers prioritize drinking over eating.
3. Genetics
Genetic backgrounds, such as the ability of a person to break down alcohol determine if they are likely to develop fatty liver and alcoholic cirrhosis.
What are The Treatment Approaches For Alcohol Abuse-Related Cirrhosis
Treating alcoholic cirrhosis involves abstinence from alcohol, detox, medication, psychotherapy, dietary, and lifestyle changes. According to a 2011 study by Frazier, T. H., et al, “Treatment Of Alcoholic Liver Disease”, published in Therapeutic Advances in Gastroenterology, abstaining from alcohol consumption is the first line of treatment.
Complete abstinence from alcohol
Abstinence from alcohol is the first step in treating alcoholic cirrhosis. This significantly reduces the risk of decompensation and destruction of the liver across all stages of the disease.
Detox
According to a 1998 study by Hayashida, M, “An Overview of Outpatient and Inpatient Detoxification”, Alcohol Health and Research World journal, the goal of detoxification is to flush out the alcohol from the addict and achieve a substance-free state. Detox makes it easy to deal with withdrawal symptoms, and treat other co-occurring conditions including cirrhosis.

- Medications: According to a 2023 study by Stokłosa, I., et al, “Medications for the Treatment of Alcohol Dependence, Current State of Knowledge and Future Perspectives from a Public Health Perspective”, medication such as Naltrexone, Disulfiram, and Acamprosate are prescribed to manage withdrawal symptoms and prevent cravings for alcohol.
- Psychotherapy: According to a 2021 study by Patel AK, “Treatment of Alcohol Use Disorder”, published in the JAMA Network journal, cognitive behavior therapy (CBT) focuses on changing your thought and behavioral patterns to help manage alcohol cravings and triggers.
- Dietary changes: These include vitamin supplementation to support overall liver health. Foods that are high in omega-3 fatty acids help to reduce withdrawal symptoms. In addition, they need magnesium-rich foods to help manage muscle spasms and cramps.
- Antioxidant therapy: Alcoholic liver disease is closely associated with oxidative stress. According to a 2011 study by Singal, A. K., et al, “Antioxidants as Therapeutic Agents for Liver Disease”, published in the Official Journal of the International Association for the Study of the Liver, antioxidant therapy is considered an effective approach in the treatment of acute and chronic alcoholic hepatitis.
Compounds such as S-adenosylmethionine (SAMe) and polyenylphosphatidylcholine (PPC) are used to reduce oxidative stress in the liver and improve liver function, potentially preventing further cirrhosis progression. Supplementing zinc is also essential as its deficiency can worsen liver injury, emphasizing the importance of correcting nutritional deficiencies in patients with alcohol-induced liver cirrhosis.
- Liver transplant: According to a 1996 study by Van Thiel, D. H., “Liver Transplantation for Alcoholics with Terminal Liver Disease”, published in the Alcohol Health and Research World journal, patients with end-stage liver disease, particularly those with alcoholic liver disease, need a liver transplant. In a world of continuous advancements, research into new treatments, including molecular pathogenesis-targeted therapies, offers hope for improved outcomes in the future.
- Social support: Patient support is a vital piece of the puzzle. Support groups, such as Alcoholics Anonymous, and services like SAMHSA’s National Helpline or local alcohol support services, provide critical assistance for individuals seeking to quit alcohol and manage their liver disease effectively.
What is The Impact of Abstinence on Cirrhosis Prognosis?
According to the 2014 study by Xie YD., “Effect Of Abstinence From Alcohol On Survival Of Patients With Alcoholic Cirrhosis: A Systematic Review And Meta-Analysis” abstinence significantly improves the survival of people with alcohol liver cirrhosis. Abstinence from alcohol is the cornerstone in the management of alcohol-related liver disease, significantly contributing to the prevention of further liver damage and enhancing chances of liver recovery.
Are There Other Causes Of Liver Cirrhosis Except Alcohol And Drugs?
Yes, there are other causes of cirrhosis. According to the NIDDK article “ Cirrhosis”, there are other causes of cirrhosis including accumulation of fat around the liver commonly known as non-alcoholic fatty liver disease. This commonly occurs due to obesity, type 2 diabetes, and metabolism problems. In addition, liver cirrhosis occurs due to hepatitis C or hepatitis B virus infection, and autoimmune diseases cause cirrhosis.
How Much Alcohol Can I Safely Drink?
The 2020-2025, “Drinking Levels Defined” Dietary Guidelines for Americans the U.S. Department of Health and Human Services and U.S. Department of Agriculture, recommend 2 drinks for adult males and 1 drink for adult females daily.
Can Your Liver Heal Itself From Cirrhosis?
While the liver has a lot of capacity to regenerate itself, this only happens when it is healthy. However, once cirrhosis develops, the liver has limited ability to regenerate. According to the 2024 article “ Cirrhosis of the Liver: Symptoms, Stages & Treatment”, from WebMD, cirrhosis is a treatable condition, but not curable. Normally, the goal of treatment is to stop further damage to the liver and prevent complications caused by the damage already caused.
If I Have Cirrhosis, Does It Mean I Have Liver Cancer Too?
No, these are two distinct conditions. However, cirrhosis predisposes you to liver cancer but not vice versa. According to the article “Liver Cancer”, from Mayo Clinic, cirrhosis, which involves extensive scarring of the liver, is a risk factor for liver cancer.