New York Mental Health Statistics

The COVID-19 pandemic impacted mental health in New York City. Even after three years, around one in three New Yorkers (31.5% as of March 2023) face depression or anxiety. This high rate hasn’t improved since May 2021. There are some groups that struggle more than others, including youths, people of color, people with low incomes, those without jobs, and those without enough food.
Mental health issues fluctuated during the pandemic. They peaked in February 2021 when two out of five New Yorkers (40.2%) reported anxiety or depression. Another spike occurred in September 2022, with 37.2% reporting poor mental health. Even with COVID-19 improving, statistics show that New York still struggles to support mental wellness across its varied communities. Offering mental health aid and resources remains crucial ahead. We’ll take a closer look at these mental health stats and examine the reasons behind this concerning trend.
Key Highlights
- Approximately one in five adult New Yorkers is likely to experience a mental health disorder each year.
- 8% of high school students in New York City have reported attempting suicide.
- Substance misuse-related consequences rank among the leading causes of premature death across all neighborhoods in NYC, resulting in approximately 1,800 deaths and over 70,000 emergency room visits annually among adults aged 18 to 64 due to alcohol use alone.
- Every month, 73,000 public high school students in NYC report feeling sad or hopeless.
- About 8% of adult New Yorkers experience symptoms of depression annually.
- Major depressive disorder constitutes the primary source of disability in NYC, with over half a million adults estimated to be affected at any given time, yet less than 40% seek treatment.
- The economic burden of depression and substance misuse in NYC amounts to an estimated $14 billion in annual productivity losses.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
Disparities in Mental Health Among New Yorkers
Depression and anxiety in New York City impact people differently based on factors like income, age, ethnicity, job loss, and food insecurity. During the first months of 2023, these differences were highly visible.
- Among New Yorkers earning under $25,000 yearly, 50.0% experienced anxiety or depression – more than double the 22.1% rate for those making over $100,000.
- Young adults aged 18-34 were also at higher risk, with 40.0% reporting poor mental health.
- Hispanic New Yorkers faced elevated challenges, with 41.0% experiencing anxiety or depression.
- Job loss during the pandemic correlated with greater distress, as 50.7% of those who lost employment income reported mental health issues.
- Food insufficiency was another major factor, with 57.4% of food-insecure New Yorkers reporting poor mental health versus only 29.2% of those with adequate food.
What Are The Mental Health Risks By Age Group in New York City?
The risk of mental illness can affect New Yorkers at any stage of their lives, but certain stages present greater challenges.
Early Years
- Childhood exposure to adverse events like domestic violence, neglect, abuse, financial strain, divorce, or unsafe neighborhoods is linked to chronic diseases and mental health threats in adulthood.
- These circumstances contribute to toxic stress, altering brain development and having a devastating lifelong impact.
- Adolescents exposed to childhood adversity are 2x as likely to develop mental disorders, with more exposures increasing the risk.
- Neighborhood violence alone can impair children’s cognitive performance.
- Experiencing two or more adverse childhood events increases depression, anxiety, and substance use by 2-8 times.
- Around 18% of children in New York State experienced multiple adverse family experiences, predicting poor mental and physical health later in life.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
Adolescence
- Over 25% of NYC public high school students felt persistently sad/hopeless, a predictor of depression.
- 10% reported dating violence, which is linked to 50% increased depressive symptoms and anxiety.
- Violence exposure increases the risk of the youth perpetrating violence by 35-144%.
- 7,000 NYC ER visits yearly involve underage alcohol use.
- 8% of students attempted suicide, doubling if bullied (18% experienced bullying).
- LGBT youth face higher bullying, suicide rates, and compounded racism/discrimination stressors.
Young Adulthood
- 3/4 of mental health/substance use disorders emerge by age 24.
- Among CUNY students, 19% had depression and 26% had significant anxiety; only 10% of depressed students got college counseling.
Parenthood
- Maternal depression affects 12% of NYC mothers and up to 20% of lower-income mothers postpartum.
- 1/3 of depressed mothers don’t seek help.
- Parent caregivers of chronically ill children face higher depression risk.
- Preventive parental interventions reduce children’s future mental disorder risk by 40%.
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
Adulthood
- Job loss, economic vulnerability, and divorce exacerbate mental illness.
- Intimate partner/domestic violence cut across all NYC demographics.
- Nearly 50% experienced psychological partner aggression; over 20% had PTSD symptoms.
Late Adulthood
- Depression rates are higher among elderly home care recipients (13.5%) and widowed (1/3).
- Elderly suicide rates are 50% higher than the general population.
- Substance use treatment needs may rise 70% as baby boomers age.
- Older caregivers of disabled individuals face higher psychological stress.
- 92 per 1,000 NYC seniors were elder abuse victims yearly.
The report highlights mental health vulnerabilities at all life stages but emphasizes opportunities for prevention and early intervention to build lifelong resilience.
Disparities in Access to Mental Healthcare in New York City
Many New Yorkers face difficulties getting quality mental healthcare. Though the city has many resources, there are major differences preventing equal access. Things like having insurance, your race/ethnicity, where you live, and your gender create barriers that affect some people more:
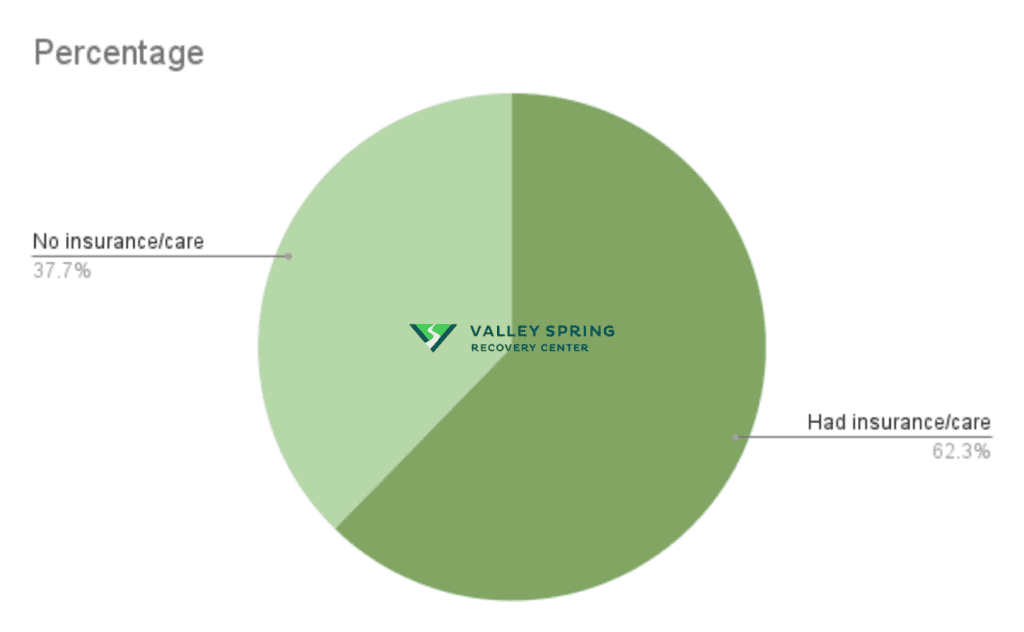
- Many New Yorkers do not have health insurance, making it difficult for them to access mental healthcare services. The following table shows the percentage of adults with mental health needs who received counseling or treatment within the past 12 months. Based on age-adjusted prevalence per 100,000 residents in 2015.
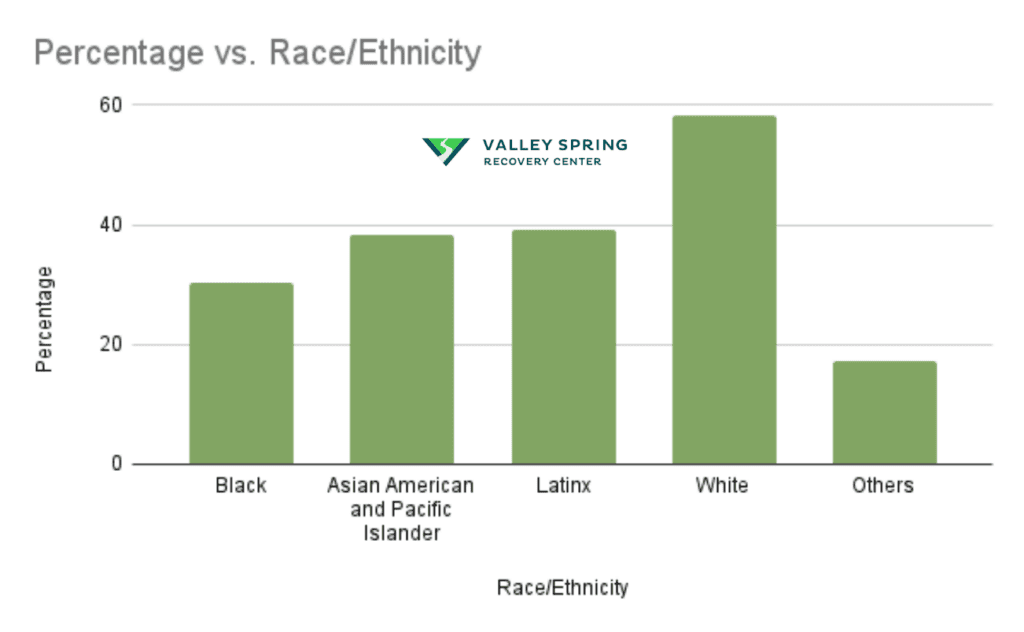
- Compared to White New Yorkers, those from Black, Latinx, Asian American, and Pacific Islander communities face greater challenges in connecting with mental health resources. The graph presents the prevalence rates of depression among different racial and ethnic groups.
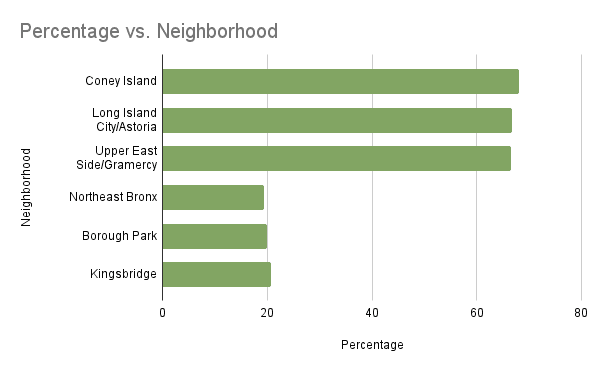
- Mental healthcare access varies significantly between New York neighborhoods. In the top three areas in the graph below, nearly 70% of those needing mental health treatment receive it. However, in the bottom three areas in the graph, only around 20% of those requiring mental health services can access them
- Among youth struggling with mental health issues, males across all racial and ethnic groups are less likely to receive the necessary mental healthcare support. The graph below highlights the percentage of youth with mental health needs who self-report connection to care, disaggregated by race/ethnicity and gender.
Are you covered for treatment?
Valley Spring Recovery Center is an approved provider for Blue Cross Blue Shield and Cigna, while also accepting many other major insurance carriers.
Check Coverage Now!What Are The Initiatives Addressing Mental Health in New York City and State?
The 2020 pandemic worsened mental health struggles. New York City responded with “Care, Community, Action: A Mental Health Plan for New York City.” It uses a public health approach, focusing on prevention, reducing harm, treatment, and recovery. With nearly $400 million invested, plus federal and state funds, the plan targets social, economic, racial, and cultural factors impacting mental health. Accountability measures track progress, though outside influences like housing policies also shape outcomes.
Furthermore, New York State’s $1 billion overhaul increases access to mental health care statewide, improves wait times, and reduces costs. This multi-year plan adds 700 inpatient beds, and funds community-based outpatient programs.
By 2019, ThriveNYC, NYC’s behavioral health initiative, will increase spending to $1.2 billion, hire 400 clinicians and provide direct care. These efforts unite government levels, highlighting prevention, intervention, and addressing health’s social factors to bolster mental wellness.
How do the New York mental health trends correlate with the addiction statistics?
The correlation between mental health trends and addiction statistics in New York City is significant and multifaceted, reflecting broader public health challenges exacerbated by the COVID-19 pandemic. Here’s a detailed exploration of how these mental health issues relate to substance use and addiction based on the comprehensive data and trends observed:
- Increased Mental Health Issues and Substance Use: The persistent high rates of depression and anxiety among New Yorkers, as highlighted by about one-third of the population experiencing these issues, correlate strongly with increased substance use. People often turn to alcohol and drugs as a coping mechanism for untreated mental health disorders, leading to higher rates of addiction.
- Impact of Socioeconomic Factors: The data reveals that mental health challenges are particularly pronounced among vulnerable populations, including those with lower incomes, unemployed individuals, and those facing food insecurity. These groups also show higher tendencies towards substance use, suggesting that economic hardships and lack of basic necessities are key contributors to both mental health decline and increased substance dependency.
- Youth and High-Risk Behaviors: The report indicates that 8% of high school students in New York City have attempted suicide, and a significant number report feeling sad or hopeless. This demographic is also at risk for substance use, as adolescents use alcohol and drugs to self-medicate against mental distress. Early exposure to adverse life events further escalates this risk, linking childhood trauma to higher rates of substance use and mental health disorders later in life.
- Substance Misuse and Premature Deaths: With substance misuse-related consequences being a leading cause of premature death across all NYC neighborhoods, there’s a clear indication that the mental health crisis is intertwined with the addiction crisis. Both are driving significant mortality rates and emergency room visits, underscoring the need for integrated health services that address both mental health and substance use comprehensively.
- Treatment Disparities and Access Issues: Despite the high prevalence of major depressive disorder and its designation as a primary source of disability in NYC, less than 40% of those affected seek treatment. There are similar statistical trends for drug addiction in New York, where there is a significant gap between those needing and those receiving help. This points to systemic barriers in healthcare access and stigma surrounding both mental health and addiction treatments.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
How does the mental health crisis influence substance use trends in NYC?
Economic pressures, ongoing social challenges, and untreated mental health conditions correlate with the New York substance abuse statistics. New Yorkers use substances as a form of self-medication, increasing addiction rates.
What are the implications of high suicide rates among youth for substance use?
High suicide rates among youth are often linked to underlying mental health issues, which are also risk factors for increased substance use, indicating a need for early mental health interventions to prevent addiction.
Why are substance misuse-related deaths considered a leading cause of premature death in NYC?
Substance misuse leads to a wide range of health complications, including fatal overdoses and long-term organ damage, significantly shortening life expectancy and increasing healthcare burden.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
How do socioeconomic factors like unemployment and food insecurity impact addiction rates?
Financial instability and lack of food security heighten stress and anxiety levels, which can lead to increased alcohol and drug use among affected populations as coping mechanisms.
What steps can be taken to address the dual challenges of mental health and substance addiction in NYC?
Integrating mental health and substance use services, expanding access to care, increasing community awareness, and reducing stigma are critical steps to address these intertwined public health challenges effectively.
Share This Post















