Dual diagnosis refers to the co-occurrence of both a mental health disorder and a substance use disorder in an individual. Common types include anxiety, depression, bipolar disorder, and schizophrenia, alongside substance use disorders involving alcohol, opioids, or stimulants.
Dual diagnosis of a mental health condition and substance use disorder occur in over 9.2 million adults in the united states. Individuals with mental illnesses are disproportionately more likely to suffer from substance use disorders, with nearly 40% of those with a substance use disorder also having a co-occurring mental illness.
(NSDUH 2019)
Symptoms differ but typically include mood swings, social withdrawal, cognitive difficulties, and erratic behavior. The causes of dual diagnosis disorders are mixed,in many cases a combination of genetic predisposition, environmental stressors, trauma, or chronic substance use exacerbating mental health disorders.
Treatment of dual diagnosis disorders focuses on integrated care that addresses both disorders simultaneously. It involves behavioral therapies, medication management, and support groups.Cognitive Behavioral Therapy (CBT) and motivational interviewing are often used to treat individuals with dual diagnosis disorders.Medications prescribed by psychiatrists or primary care doctors target mood stabilization or withdrawal management. Complete care ensures a more sustainable recovery path by focusing on the whole person, rather than just the symptoms of their conditions.
What Are Co-Occurring Disorders (Dual Diagnosis)?
Dual Diagnosis Disorders, also known as co-occurring disorders, refer to the simultaneous presence of both a mental health disorder and a substance use disorder in an individual. According to the Diagnostic and Statistical Manual of Mental Disorders DSM-5, dual diagnosis occurs when a person meets the diagnostic criteria for at least one Substance Use Disorder and one mental health disorder, such as depression, anxiety, or bipolar disorder. The research highlights that these disorders can interact, intensify the severity of both conditions, and complicate treatment efforts.
According to the research published in The National Institute on Drug Abuse explains that co-occurring disorders are common and can appear in various combinations. For example, a person with alcohol use disorder might also suffer from post-traumatic stress disorder (PTSD), or an individual struggling with opioid addiction might also experience generalized anxiety disorder.
Dual diagnosis can occur in multiple forms, including combinations of anxiety disorders, mood disorders, personality disorders, and substance addictions like alcohol, opioids, or cocaine. Because of the complex interaction between mental health and substance use, treatment requires integrated care that addresses both issues simultaneously for the best outcomes.
Co-occurring dual disorders are like having two challenges at once. It's not just the addiction you're battling; it could also be things like anxiety, depression, or other mental health issues.
Doctor Michael Olla.
How Common is Dual Diagnosis?
Dual diagnosis, or co-occurring disorders, is prevalent across the U.S. and affects a significant portion of the population. According to the research by the Substance Abuse and Mental Health Services Administration (SAMHSA), approximately 9.2 million adults in the U.S. experienced both a mental health disorder and a substance use disorder in 2018, reflecting nearly 4% of the adult population.
A study published by the National Institute on Alcohol Abuse and Alcoholism reports that among individuals with alcohol use disorder, around 20% to 50% also experience a co-occurring mental health condition such as depression or anxiety. According to the research Behavioral Health Barometer New Jersey, Volume 6 In New Jersey, the prevalence of co-occurring disorders is consistent with national trends. In 2020, approximately 45.9% of adults with a substance use disorder also had a mental illness, highlighting the critical need for integrated care.
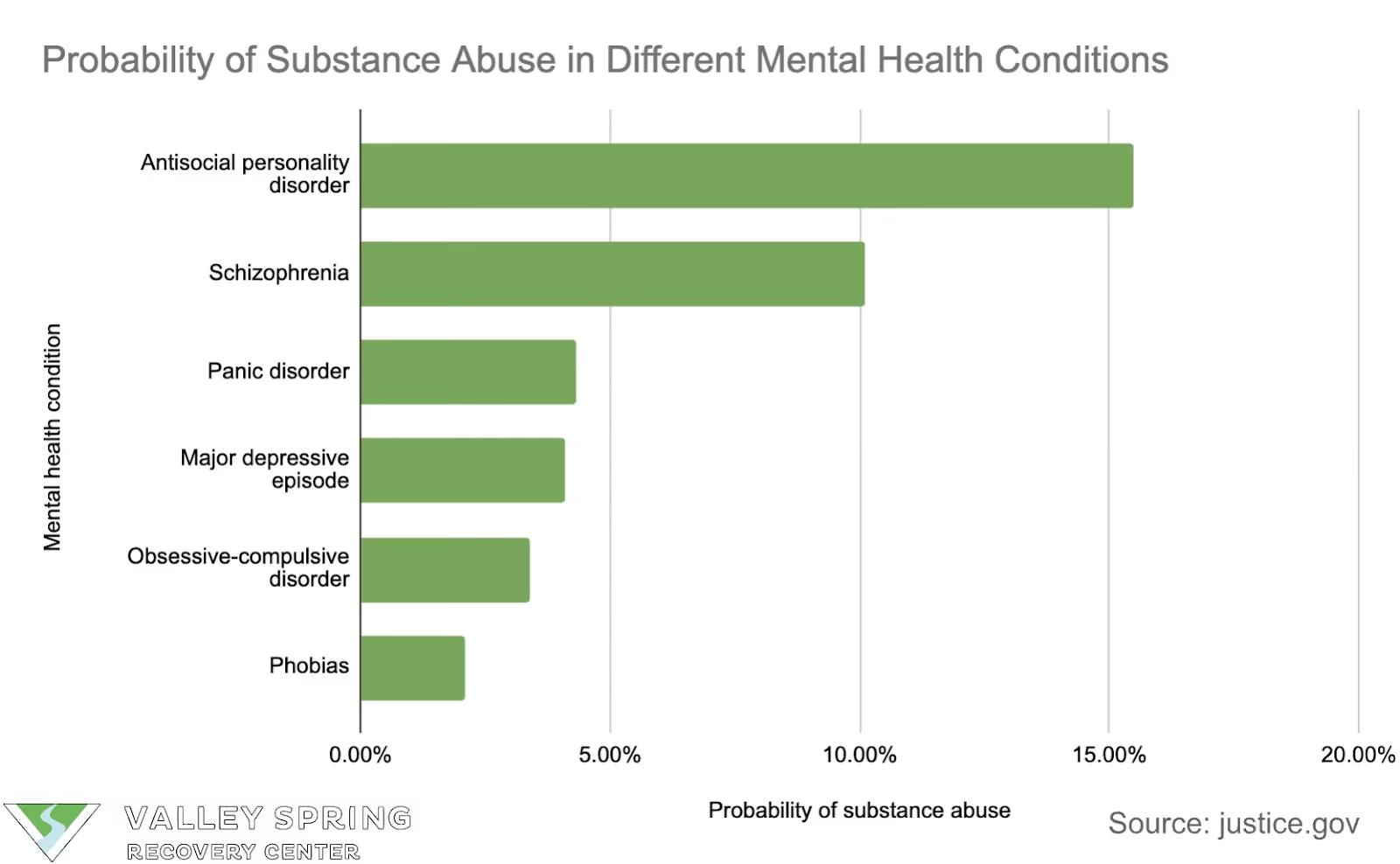
The prevalence of dual diagnosis in the United States is increasing, with significant impacts on healthcare due to the intertwining of mental health issues and substance abuse, exacerbated by factors like the COVID-19 pandemic.
- As per SAMHSA's 2022 National Survey on Drug Use and Health, roughly 21.5 million adults in the United States have a dual diagnosis.
- The number of people with both severe mental illness and substance use disorder increased from 1.0% (2.3 million people) in 2015 to 1.4% (3.6 million people) in 2019.
- As of 2022, nearly 44 percent of surveyed individuals in the United States diagnosed with a mental illness stated they had used an illicit drug within the past year.
- In 2019, 7.7 million adults experienced both mental health issues and substance use disorders simultaneously.
- Among the 20.3 million adults dealing with substance use disorders in 2019, 37.9% also dealt with mental illness. Out of the 42.1 million adults experiencing mental illness, 18.2% also struggled with a substance use disorder.
[bricks_template id="690"]
What are the types of Dual Diagnosis Disorders?
The types of dual-diagnosis disorders are meth addiction and psychosis, alcoholism and depression, drug addiction and anxiety, opioid addiction and PTSD (Post-Traumatic Stress Disorder), marijuana addiction and schizophrenia, benzodiazepine dependence, alcoholism and ADHD (Attention-Deficit Hyperactive Disorder), cocaine addiction and bipolar disorder, heroin addiction and borderline personality disorder (BPD), ecstasy (MDMA) addiction and social anxiety.
Below is the detail of these types:
Ecstasy (MDMA) Addiction and Social Anxiety: Ecstasy is frequently used for its euphoric and empathogenic effects, which can help individuals with social anxiety feel more connected and less inhibited. However, chronic MDMA use can lead to serotonin depletion, worsening social anxiety over time. es explanations on why each dual diagnosis occurs, associated risks, and how treatment approaches need to be tailored specifically for each issue:
Meth Addiction and Psychosis: Methamphetamine abuse can induce psychotic symptoms such as hallucinations, paranoia, and delusions. These episodes can persist long after meth use is discontinued, with chronic users more likely to experience prolonged psychosis. The link between meth use and psychosis is well-established. According to the research by SAMHSA, this connection significantly increases the risk of developing psychotic symptoms, which can make recovery even more challenging.
Alcoholism and Depression: Alcoholism often coexists with depression, as alcohol's depressant effects can exacerbate feelings of hopelessness and sadness. Many individuals with depression use alcohol to self-medicate, but this can worsen depressive symptoms and create a cycle of dependency. According to research published in the National Library of Medicine, about 30-50% of people with alcohol use disorder also suffer from major depressive disorder.
Drug Addiction and Anxiety: Individuals with anxiety disorders are more likely to abuse substances such as cocaine, amphetamines, or alcohol in an attempt to alleviate their symptoms. However, drug use can worsen anxiety, particularly during withdrawal, leading to heightened restlessness, panic attacks, and paranoia.
Opioid Addiction and PTSD: Veterans and trauma survivors often develop opioid addiction as they attempt to manage both physical pain and psychological distress from PTSD. The two disorders feed into each other, with opioids used to numb emotional pain, which can worsen trauma-related symptoms.
Marijuana Addiction and Schizophrenia: Chronic marijuana use, especially in young adults, has been linked to an increased risk of schizophrenia. While marijuana can provide temporary relief from anxiety and stress, it can also trigger psychosis and paranoia in vulnerable individuals.
Benzodiazepine Dependence and Anxiety: Benzodiazepines, such as Xanax or Valium, are prescribed to treat anxiety, but prolonged use can lead to physical dependency.Over time, higher doses may be needed, and withdrawal can result in rebound anxiety and panic attacks.
Alcoholism and ADHD: Individuals with ADHD may turn to alcohol as a way to cope with impulsivity, restlessness, and concentration difficulties. However, alcohol can worsen ADHD symptoms and increase the risk of developing a substance use disorder.
Cocaine Addiction and Bipolar Disorder: Cocaine is a stimulant that can intensify the manic episodes associated with bipolar disorder, leading to erratic and risky behavior. During depressive episodes, individuals may use cocaine to lift their mood, but this often exacerbates emotional instability.
Heroin Addiction and Borderline Personality Disorder (BPD): BPD is characterized by emotional dysregulation and impulsivity, which can drive individuals toward heroin use as a way to self-soothe intense feelings of emptiness or distress. Heroin use, in turn, often worsens the emotional instability associated with BPD.
| Substance Use Disorder | Mental Health Disorder | Why It Occurs | Risks | Treatment Approach |
|---|---|---|---|---|
| Meth Addiction | Psychosis | Methamphetamine can trigger or exacerbate psychotic symptoms such as delusions and hallucinations. | Increased severity of psychosis, higher risk of self-harm or harm to others. | Integrated treatment focusing on both psychosis management and addiction recovery, possibly including antipsychotic medications and behavioral therapies. |
| Prescription Drug Addiction | Anxiety | Anxiety disorders might lead individuals to misuse prescribed medications for quick relief. | Dependency on medication, worsening anxiety symptoms over time. | Cognitive Behavioral Therapy (CBT) combined with careful medication management and monitoring. |
| Alcoholism | Depression | Alcohol is used to self-medicate mood, but as a depressant, it can deepen depression symptoms. | Increased depressive episodes, suicidal tendencies. | Dual focus on treating depression and curbing alcohol dependence through psychotherapy and support groups. |
| Opioid Addiction | PTSD (Post-Traumatic Stress Disorder) | Opioids may be used to numb emotional and physical pain associated with traumatic memories. | Enhanced emotional numbing, increased risk of overdose. | Trauma-informed care alongside substance use treatment, including therapies like EMDR (Eye Movement Desensitization and Reprocessing). |
| Marijuana Addiction | Schizophrenia | Marijuana can precipitate psychosis in vulnerable individuals, particularly those predisposed to schizophrenia. | Potential for persistent psychotic disorders, difficulty in distinguishing reality. | Antipsychotic treatments and programs designed to reduce marijuana use and address the cognitive impacts of schizophrenia. |
| Benzodiazepines Dependence | Anxiety | Benzodiazepines are often prescribed for anxiety; however, they can lead to dependence and worsen anxiety over time. | Increased anxiety symptoms, potential for severe withdrawal symptoms. | Gradual tapering of the drug, along with therapy to manage anxiety without reliance on medication. |
| Alcoholism | ADHD (Attention-Deficit Hyperactive Disorder) | Individuals with ADHD may use alcohol to self-soothe the symptoms of impulsivity and hyperactivity. | Increased impulsivity and risky behaviors, potential for developing severe alcohol dependency. | Behavioral interventions and appropriate medications to manage ADHD symptoms, reducing the need for self-medication with alcohol. |
| Cocaine Addiction | Bipolar Disorder | Stimulant use during manic phases can be appealing due to increased energy and euphoria, leading to abuse. | Risk of extreme manic episodes and rapid cycling between moods. | Mood stabilizers and supervised detoxification, coupled with psychotherapy to address both bipolar disorder and substance abuse. |
| Heroin Addiction | Borderline Personality Disorder (BPD) | Heroin may be used to alleviate feelings of emptiness or emotional instability associated with BPD. | High risk of addiction, increased emotional and relationship instability. | Dialectical Behavior Therapy (DBT) to address emotional regulation and substance abuse treatment programs. |
| Ecstasy (MDMA) Addiction | Social Anxiety | MDMA is used to enhance sociability and reduce inhibitions in social settings. | Dependency leading to increased social anxiety, potential for neurotoxic effects. | Therapy focused on developing social skills without reliance on substances, combined with MDMA cessation programs. |
Why do Substance Use Disorder and Mental Disorder Occur Together?
Substance use disorders (SUDs) and mental health disorders often coexist due to a complex interplay of biological, psychological, and environmental factors. Vulnerability plays a key role, as both disorders share overlapping risk factors, including genetic predispositions and early exposure to trauma. Research from SAMHSA and the National Library of Medicine indicates that certain genetic variations can increase susceptibility to both mental health issues and addiction by affecting stress and reward pathways.
Additionally, mental health conditions like anxiety, depression, and PTSD can lead individuals to self-medicate with substances, which may escalate into abuse. For example, those with anxiety or mood disorders are twice as likely to develop SUDs compared to the general population. Conversely, chronic substance use can trigger or worsen mental health conditions, with drugs like methamphetamines and alcohol altering brain chemistry and increasing risks for psychosis, depression, or anxiety. This bidirectional relationship complicates treatment, highlighting the need for integrated approaches that address both conditions simultaneously for effective care.
What are the Symptoms of Dual Diagnosis Disorders?
Individuals with dual diagnosis disorders may experience symptoms like intense mood swings, ranging from extreme depression or anxiety to episodes of heightened irritability or paranoia. Cognitive impairments such as difficulty concentrating, memory problems, or confusion are common, along with behavioral changes like impulsivity, risk-taking, and neglect of responsibilities.
Physical symptoms may include sleep disturbances, changes in appetite, or frequent illness, often linked to substance use. The urge to keep using substances, even when it harms health or relationships increases the difficulty of dealing with both mental health issues and substance dependency at the same time. The symptoms of dual-diagnosis disorders are listed below:
Symptoms of Substance Use Disorders
The symptoms of substance use disorders are social withdrawal, behavioral changes, using substances in dangerous conditions, risky behaviors, loss of control, tolerance withdrawal, and dependency.
Below are the details of these symptoms:
- Social Withdrawal: Social withdrawal is the tendency to isolate oneself from friends, family, and social activities. Individuals often withdraw to hide their behavior or avoid judgment. This isolation can also result from a lack of interest in previously enjoyed activities due to the overwhelming focus on substance use.
- Behavioral Changes: Behavioral changes refer to significant shifts in how an individual acts, often becoming more secretive, aggressive, or erratic. These changes are typically linked to the compulsive nature of substance use, which alters priorities and can lead to neglecting responsibilities and self-care.
- Use in Dangerous Conditions: This symptom involves using substances in situations where it poses a physical risk, such as driving under the influence or operating machinery. The impaired judgment caused by substance use increases the likelihood of accidents, injuries, and harm to oneself or others.
- Risky Behaviors: Risky behaviors are actions that are impulsive and hazardous, such as engaging in unprotected sex, committing crimes, or taking extreme physical risks. These behaviors are often driven by a combination of the craving for substances and the altered brain functioning that reduces impulse control.
- Loss of Control: Loss of control is the inability to regulate or limit substance use, even when one has a desire to stop. Individuals may set limits on how much or how often they will use substances, but find themselves unable to stick to those boundaries due to the powerful urge for the substance.
- Tolerance and Withdrawal: Tolerance occurs when the body requires larger amounts of the substance to achieve the same effect, while withdrawal refers to the physical and psychological symptoms experienced when substance use is reduced or stopped. Common withdrawal symptoms include anxiety, nausea, sweating, and irritability.
- Dependency: Dependency refers to the physical and psychological reliance on a substance, where an individual feels they cannot function normally without it. Over time, substance use becomes a necessary part of daily life, making it difficult for the person to quit despite the negative consequences.
Symptoms of Mental Health Disorders
The symptoms of mental health disorders are extreme mood changes, cognitive difficulties, social avoidance, suicidal thoughts, and neglecting responsibilities. Below are key symptoms often associated with these disorders:
- Extreme Mood Changes: This refers to rapid or severe fluctuations in emotions, ranging from intense sadness to heightened irritability or excitement. Mood changes are common in disorders like depression, anxiety, and bipolar disorder, affecting the individual’s ability to maintain emotional stability.
- Cognitive Difficulties: Cognitive difficulties involve problems with thinking processes, such as trouble concentrating, memory loss, or confusion. These issues can arise in disorders like depression, schizophrenia, or anxiety, impairing the ability to make decisions or focus on tasks.
- Social Avoidance: Social avoidance is the tendency to withdraw from social interactions, which can stem from anxiety, fear of judgment, or feelings of worthlessness. Disorders such as social anxiety, depression, and PTSD often lead individuals to avoid friends, family, and social events.
- Suicidal Thoughts: Suicidal thoughts are persistent feelings of hopelessness and the desire to end one's life. These thoughts can occur in severe depression, bipolar disorder, and other mental health conditions, indicating a critical need for immediate intervention and support.
- Neglecting Responsibilities: This symptom involves failing to fulfill daily obligations, such as work, school, or personal care. Individuals with mental health disorders may struggle with motivation, energy, or the ability to stay organized, resulting in neglected duties and self-care.
What are the effects of Dual Diagnosis Disorders?
The common effects of dual diagnosis disorder are Emotional Breakdown and Physical Health Problems. Below is the detail of these effects:
- Emotional Breakdown: An emotional breakdown refers to a state of overwhelming stress, anxiety, or depression that leaves an individual unable to cope with daily life. In the case of dual diagnosis, substance use can intensify the symptoms of mental health disorders, worsening feelings of despair, irritability, and hopelessness. This constant emotional turmoil heightens the risk of mental health crises, such as suicidal ideation. According to research published in the New England Journal of Medicine, substance use disorders can exacerbate mental health conditions by altering brain function and increasing emotional dysregulation.
- Physical Health Problems: Substance use combined with untreated mental health conditions can lead to serious physical health problems like liver damage, cardiovascular diseases, neurological problems and many more. Chronic illnesses such as liver damage, cardiovascular disease, and respiratory issues are common, especially when substance use is prolonged. Mental health disorders can also cause neglect of self-care, poor nutrition, lack of exercise, and insufficient sleep, which further degrade physical health. According to the research published by the National Library of Medicine written by D.A. Regier individuals with dual diagnosis are at a higher risk for chronic physical conditions, and managing these can complicate treatment and recovery. Additionally, according to the research by Merikangas published in the national library of medicine, the co-occurrence of mental health and substance use disorders significantly increases the likelihood of severe health complications, leading to a reduced quality of life and shorter life expectancy.
What are the Causes of Dual Diagnosis Disorders?
The causes of dual diagnosis disorder include genetic factors, early exposure, brain chemistry, stress, peer influence, drug use, and a lack of timely intervention.
Below is the detail of these causes:
- Genetic Factors: Genetics play a significant role in dual diagnosis disorders. According to the research published by the National Institutes of Health, individuals with a family history of mental health conditions or addiction are at a higher risk due to inherited genetic predispositions.
- Early Life Experiences: Childhood trauma, abuse, or neglect can significantly increase the risk of developing both substance use and mental health disorders later in life. According to the research Traumatic Events in Dual Disorders: Prevalence and Clinical Characteristics early adverse experiences are closely linked to long-term psychological and addiction-related issues.
- Brain Chemistry: An imbalance in brain chemicals, such as dopamine and serotonin, can lead to mental health issues or addiction. These chemical disruptions can make an individual more vulnerable to developing both disorders.
- Stress: Chronic stress from work, relationships, or other life challenges is another key contributor. Heightened stress levels can exacerbate mental health issues, making individuals more prone to substance use as a coping mechanism.
- Peer Pressure: Surrounding oneself with peers who use substances can influence an individual’s decision to start using drugs or alcohol. This peer influence increases the risk of developing a substance use disorder and, when combined with an existing mental health condition, leads to dual diagnosis.
- Drug Use: Drug and alcohol use can alter brain chemistry and increase the likelihood of mental health problems. Over time, substance abuse interferes with the brain's normal functioning, making it more susceptible to disorders like anxiety, depression, or schizophrenia.
- Not Seeking Help: Failing to seek treatment for existing mental health issues can lead to self-medication through drugs or alcohol, which in turn increases the risk of addiction. Without professional intervention, the cycle of substance use and worsening mental health continues to escalate.
How is Dual Diagnosis Disorder Diagnosed?
Dual-diagnosis disorder is diagnosed through a comprehensive evaluation by healthcare professionals who specialize in mental health and substance use disorders. The process typically begins with a detailed patient history, including questions about substance use patterns, mental health symptoms, and family background. Clinicians use diagnostic tools, such as the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), to assess the presence of both a mental health disorder and a substance use disorder. Medical professionals also conduct physical exams, blood tests, and psychological assessments to rule out any underlying medical conditions or brain injuries. Accurate diagnosis often requires collaboration between psychiatrists, psychologists, and addiction specialists to ensure that both conditions are identified and properly addressed.
What Are The Dual Diagnosis Statistics Across Different Demographics?
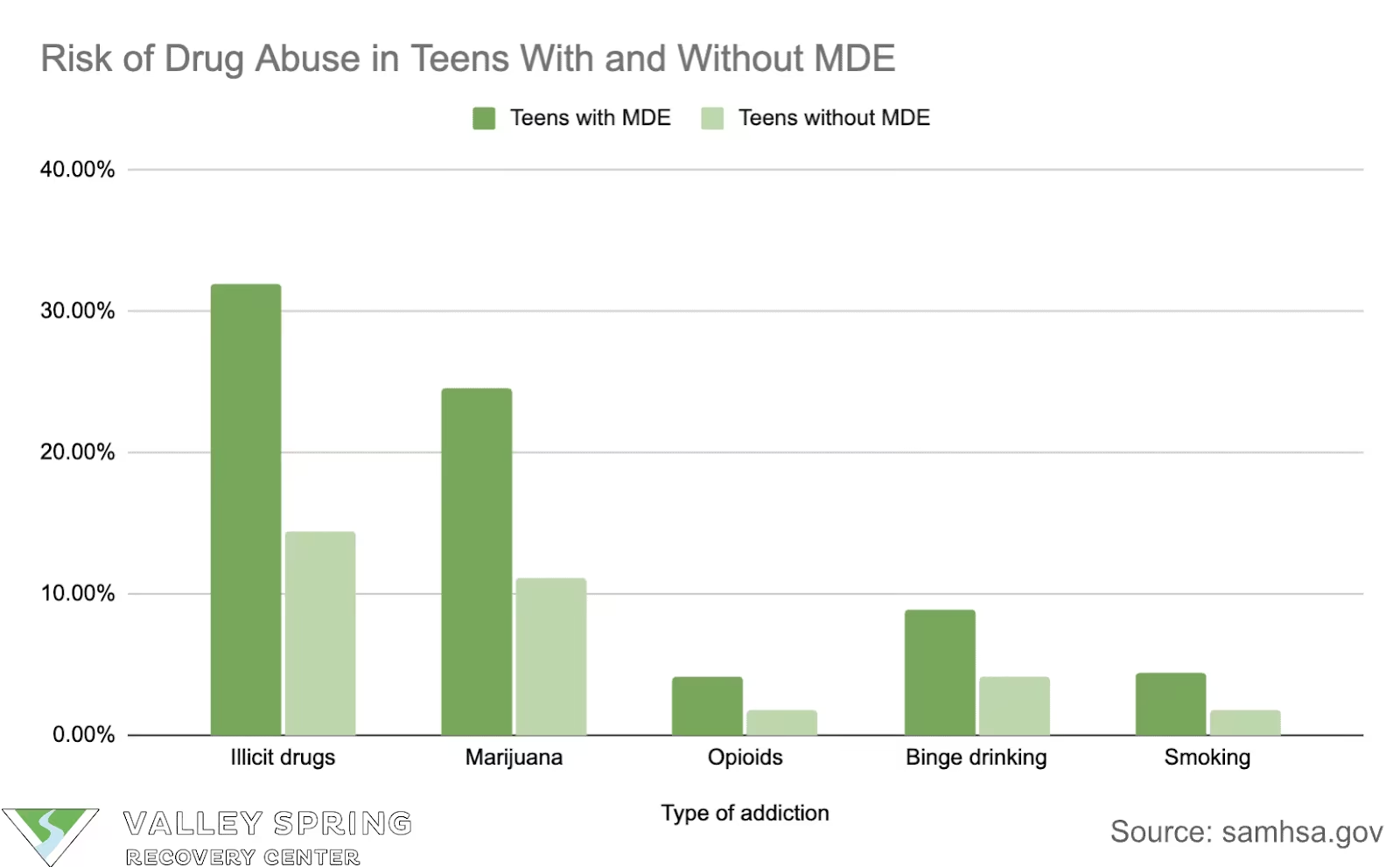
The occurrence of dual diagnosis varies significantly across different demographic groups. Age, gender, ethnicity, and socioeconomic status all play a role in the prevalence, presentation, and access to treatment for individuals struggling with both a mental health condition and a substance use disorder.
- In 2021, 13.5% of young adults aged 18 to 25 experienced both a substance use disorder and a mental illness within the past year.
- In a survey, nearly one-third of all adults had either a substance use disorder or a mental illness within the past year.
- 46% of young adults aged 18-25 experienced either a substance use disorder or a mental illness.
- The proportion of adults aged 18 or older meeting criteria for both a mental illness and a substance use disorder within the past year was higher among multiracial adults.
- In 2021, Asian adults were less likely than adults in most other racial or ethnic groups to have experienced both Any Mental Illness (AMI) and a substance use disorder within the past year.
- Teens with a major depressive episode (MDE) were more likely to use drugs compared to teens without MDE between 2018 and 2019.
- Adults with a Serious Mental Illness (SMI) or AMI in the past year were more likely to use substances compared to adults with no mental illness.
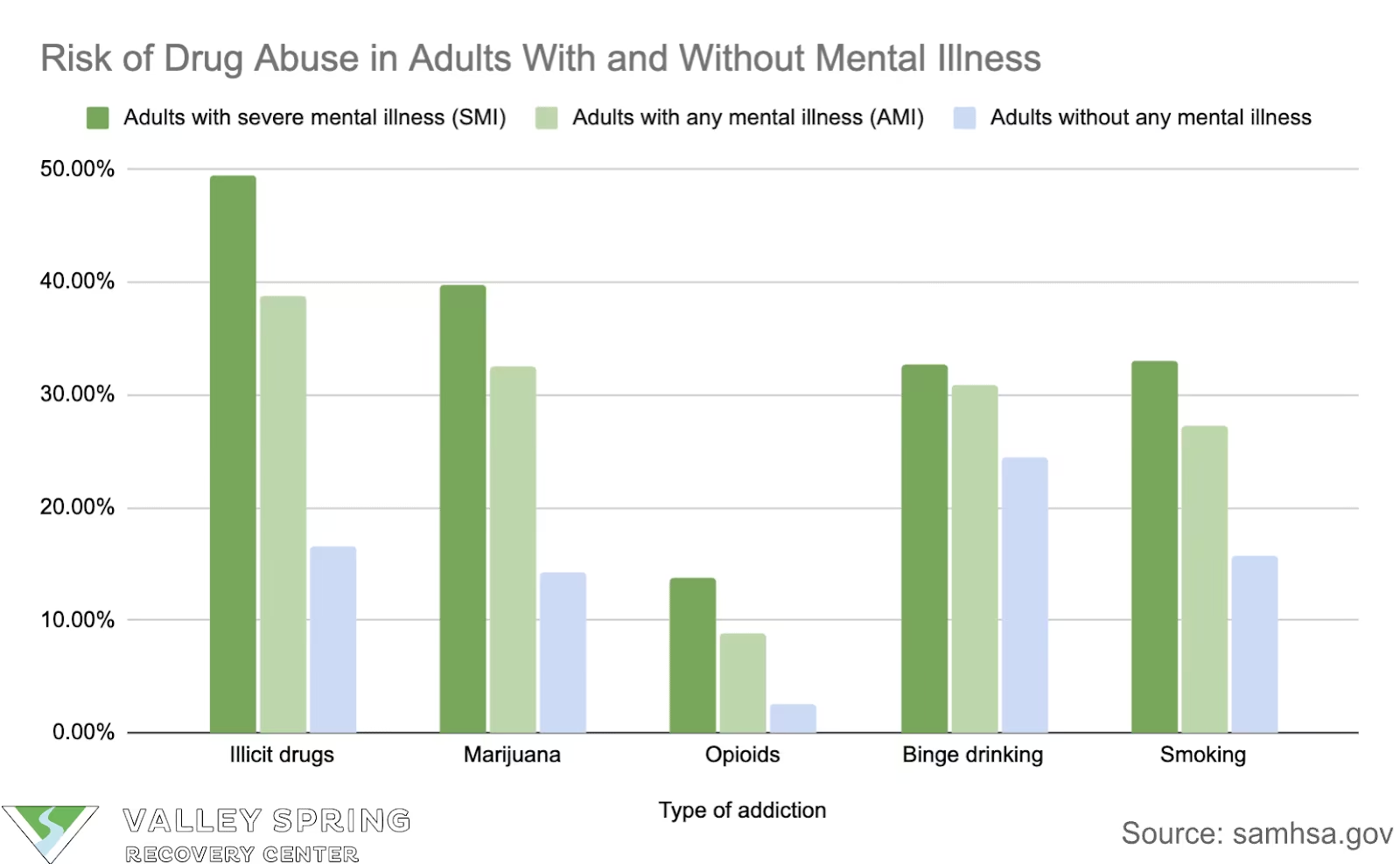
Dual Diagnosis Treatment Statistics
Despite the high prevalence of dual diagnosis, many individuals don't receive the integrated treatment they need. Here are some key dual diagnosis treatment statistics:
- Among the 397,000 adolescents aged 12 to 17 in 2019 who experienced both a Substance Use Disorder (SUD) and a co morbid mental disorder within the past year.
- 66.3%, or 263,000 individuals, received either substance use treatment at a specialty facility or mental health services within the past year.
- 62.5%, or 249,000 individuals, received only mental health services.
- 2.4%, or 10,000 individuals, received only substance use treatment at a specialty facility.
- Of the 9.5 million adults aged 18 or older in 2019 who encountered both a SUD and AMI within the previous year:
- 48.6%, or 4.6 million individuals, received either substance use treatment at a specialty facility or mental health services within the past year.
- 38.7%, or 3.7 million individuals, received only mental health services.
- 7.8%, or 742,000 individuals, received both substance use treatment at a specialty facility and mental health services.
- Out of the 3.6 million adults aged 18 or older in 2019 who suffered from both a SUD and SMI during the previous year:
- 66.6%, or 2.4 million individuals, received either substance use treatment at a specialty facility or mental health services within the past year.
- 52.0%, or 1.9 million individuals, received mental health services only.
- 12.7%, or 452,000 individuals, received both substance use treatment at a specialty facility and mental health services.
- 1.9%, or 68,000 individuals, received only substance use treatment at a specialty facility.
[bricks_template id="690"]

What are the treatment options for Dual Diagnosis disorders?
Treatment options for dual diagnosis disorder are Behavioral Therapies, Medication, Support Groups, and Rehabilitation Centers.
Below are the details of these treatment options:
- Behavioral Therapies: Behavioral therapies, such as Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT), are crucial for treating dual diagnosis disorders. They focus on identifying and changing negative thought patterns and behaviors linked to mental health and substance use issues. Through structured sessions, individuals learn coping strategies and emotional regulation skills, helping to prevent relapse. These therapies are effective but require commitment and regular attendance, typically spanning several months with ongoing sessions tailored to individual needs.
- Medication: Medications are essential in dual diagnosis treatment, helping to stabilize mood and reduce cravings. Options include antidepressants, anti-anxiety medications, and addiction-specific treatments like methadone. The main advantage is immediate symptom relief, enhancing daily functioning. However, side effects and the risk of dependency require careful monitoring by healthcare professionals. The duration of medication may vary, depending on individual response and progress.
- Support Groups: Support groups play a crucial role in the treatment of dual-diagnosis disorders, as they provide emotional and social support that can significantly improve recovery outcomes. According to the research Support, Mutual Aid and Recovery from Dual Diagnosis by Alexandre B. Laudet, combining peer social support with proper management can lead to fewer crisis events and hospitalizations, as well as improvements in overall quality of life. For example, a pilot study conducted among dually-diagnosed clients found that those who participated in peer support groups experienced enhanced physical and emotional well-being. These groups offer a space for individuals to share experiences, gain encouragement, and develop coping strategies, making them an essential component of complete care.
- Rehabilitation Centers: Rehabilitation centers offer structured programs that combine medical treatment, counseling, and support for dual diagnosis, giving individuals a much-needed sense of safety and guidance. These facilities create a nurturing environment for detoxification and therapy, addressing both mental health and substance use issues. The main advantage lies in the personalized, 24/7 care they provide.This journey can be challenging, as these programs can be expensive and require stepping away from daily life for 30 to 90 days, followed by ongoing outpatient support. These options help individuals heal completely.
What are the Limitations of Treating Co-occurring Disorders Separately?
The limitations of treating co-occurring disorders separately are incomplete understanding, risk of relapse, less effective treatment, missed opportunities, and longer recovery.
Below are the details of these limitations:

- Incomplete Understanding: Treating co-occurring disorders separately often leads to an incomplete understanding of how these conditions interact and influence each other. Mental health issues can exacerbate substance use disorders and vice versa. When treatment focuses on one disorder without considering the other, healthcare providers may miss crucial connections, which can hinder the overall effectiveness of the treatment.
- Risk of Relapse: When co-occurring disorders are addressed in isolation, there is a heightened risk of relapse. For instance, if a mental health condition is untreated, individuals may turn to substances as a coping mechanism, undermining their recovery from either disorder. This cycle of relapse can become self-perpetuating, making sustained recovery more challenging.
- Less Effective Treatment: Treating each disorder independently often results in less effective treatment outcomes. Integrated approaches that address both mental health and substance use issues simultaneously are generally more effective in achieving long-term recovery. Separate treatments may not adequately equip individuals with the necessary skills to manage both conditions, leading to suboptimal results.
- Missed Opportunities: By focusing on one disorder at a time, healthcare providers may miss opportunities for comprehensive care that could benefit the individual. Integrated treatment can capitalize on the strengths and insights gained from addressing both disorders together, promoting a more holistic approach that can improve overall health and recovery.
- Longer Recovery: Treating co-occurring disorders separately can extend the duration of recovery. Individuals may find themselves cycling through multiple treatment programs, each targeting a single disorder. This fragmented approach often results in a longer and more complicated recovery journey, as underlying issues may remain unaddressed, prolonging the overall healing process.
How to Prevent Dual Diagnosis Disorders?
To prevent dual-diagnosis disorders, you should learn about your family history, avoid drugs and alcohol, pay attention to your mental health, and engage in daily workouts.
Below are the details of the these prevention measures:

- Learn About Your Family History: Understanding your family history of mental health and substance use disorders is a crucial first step in prevention. Genetic factors can increase your risk, so being aware of any predispositions allows you to take proactive measures. Knowledge of family patterns can also help you recognize early warning signs in yourself and seek help when necessary.
- Avoid Drugs and Alcohol: Steering clear of drugs and alcohol is essential for preventing dual diagnosis disorders. Substance use can trigger or exacerbate underlying mental health issues, leading to a cycle of dependency and worsening symptoms. By avoiding these substances altogether, you reduce the risk of developing both substance use and mental health disorders.
- Pay Attention to Your Mental Health: Regularly monitoring your mental health is vital for early intervention. This includes recognizing signs of stress, anxiety, or depression and seeking professional help when needed. Staying engaged with your mental well-being helps you address issues before they escalate, thereby reducing the likelihood of developing a dual diagnosis.
- Engage in Daily Workouts: Incorporating daily physical activity into your routine has numerous mental health benefits. Exercise can reduce stress, anxiety, and depression while improving mood and overall well-being. Engaging in regular workouts promotes a healthier lifestyle and serves as a protective factor against the development of mental health issues and substance use disorders.
What are the Most Common Dual-Diagnosis Disorders?
The most common dual-diagnosis disorders typically involve a combination of substance use disorders and various mental health conditions. Alcohol use disorder frequently co-occurs with depression and anxiety disorders, as individuals may turn to alcohol as a coping mechanism. Similarly, opioid use disorder is often seen alongside mood disorders, including bipolar disorder and major depressive disorder. Additionally, individuals with post-traumatic stress disorder (PTSD) may struggle with substance use as a way to manage their symptoms. Other prevalent combinations include cannabis use disorder with anxiety disorders and eating disorders with substance abuse, highlighting the interaction between mental health and substance use that characterizes dual diagnosis disorders.

Can bipolar disorder coincide with substance use disorder?
Yes, bipolar disorder can coincide with substance use disorder, often leading to a complex interplay between mood swings and substance-related behaviors. Individuals with bipolar disorder may use substances as a form of self-medication to cope with the highs and lows of their condition. This can result in increased risk for drug addiction, as the pursuit of temporary relief may lead to unhealthy patterns of use. The combination of these disorders complicates treatment and recovery, emphasizing the need for integrated approaches to address both conditions effectively.
Can anxiety coincide with substance use disorder?
Yes, anxiety can coincide with substance use disorder, creating a challenging cycle for those affected. Individuals often turn to substances as a way to alleviate feelings of anxiety, seeking temporary relief from their symptoms. However, this self-medication can lead to increased reliance on drugs or alcohol, ultimately worsening both the anxiety and the risk of addiction. The overlap of these conditions complicates treatment, highlighting the importance of addressing both anxiety disorder and substance use concurrently for effective recovery.
Can depression coincide with substance use disorder?
Yes, depression can coincide with substance use disorder, often creating a complex relationship between the two. Individuals struggling with depression may use substances to escape their feelings or to find temporary relief from their symptoms. However, this can lead to a cycle of increased dependence on drugs or alcohol, which further worsens the depressive symptoms. The intertwining of these conditions complicates treatment and recovery, underscoring the need for a comprehensive approach that addresses both depression and substance use simultaneously.
Where To Get Treatment For Co-Occurring Disorders Near Me?
The treatment of co-occurring disorders requires a comprehensive and integrated approach, considering the interplay between mental health and substance use. Two highly effective techniques for addressing these complex conditions are Integrated Dual Diagnosis Treatment (IDDT) and Cognitive-Behavioral Therapy (CBT). The key to effective treatment for co-occurring disorders is that it must be personalized to the individual’s unique needs, considering the severity and type of the mental health disorder as well as the substance use disorder. Coordinated care that addresses all aspects of a person’s life, including psychological, physical, social, and environmental factors, is the most effective way to recover.
IDDT emphasizes the coordination of mental health and substance use treatment, providing a holistic framework for care. CBT, on the other hand, targets both cognitive and behavioral aspects, empowering individuals to challenge negative thoughts and develop healthier behaviors.
Dual Diagnosis treatment in New Jersey is available at Valley Spring Recovery Center for individuals struggling with mental health issues and drug addiction. Contact us today to speak to one of our compassionate admissions counselors who are standing by 24/7.
