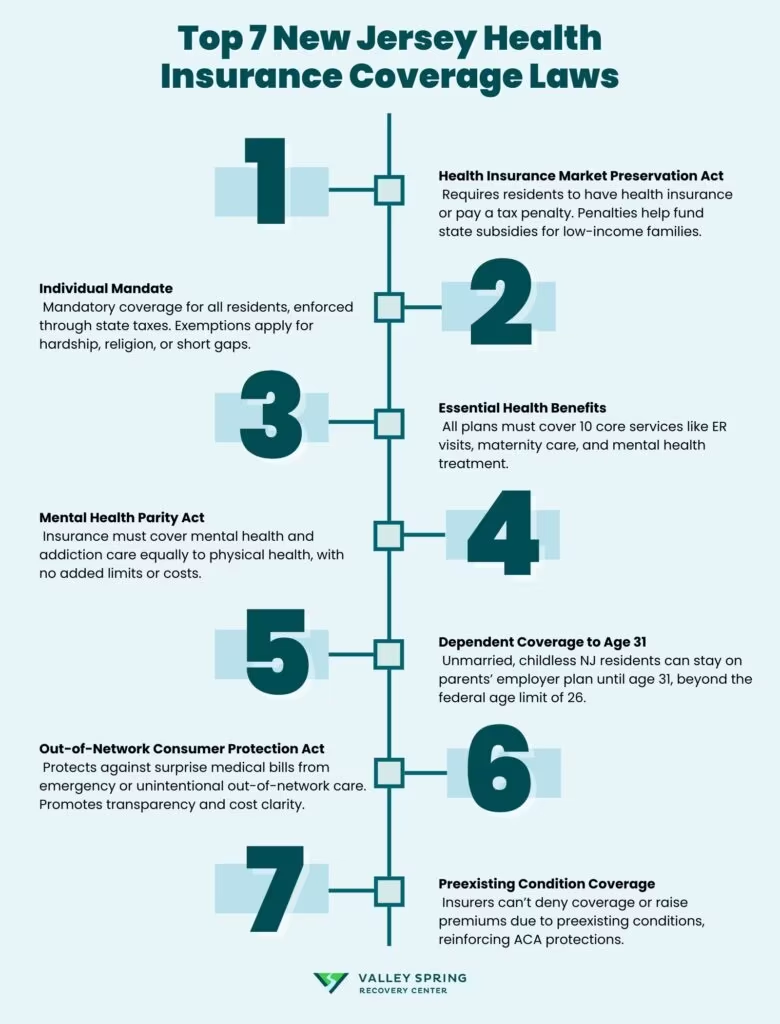
New Jersey has enacted some of the strongest insurance protections for substance use disorder and mental health treatment in the United States. Understanding these laws is important for anyone seeking addiction treatment — and for anyone who has been denied coverage or faced unreasonable barriers to care. This page provides an overview of New Jersey's key insurance mandates, parity laws, and patients' legal rights when navigating coverage for addiction treatment.
Valley Spring Recovery Center at 830 Broadway, Norwood, NJ 07648 is in-network with 17+ major NJ insurance plans. Our admissions team conducts free insurance verification and can help patients understand their rights under NJ and federal law when pursuing coverage. Call (855) 924-5320 for a free benefits check.
1. New Jersey Mental Health Parity and Addiction Equity Act
The New Jersey Mental Health Parity and Addiction Equity Act is one of the most important laws for people seeking addiction treatment coverage in NJ. This state law mirrors and strengthens the federal Mental Health Parity and Addiction Equity Act (MHPAEA, 2008) within New Jersey-regulated insurance plans.
What the law requires: Insurers must provide coverage for mental health and substance use disorder (SUD) treatment on par with coverage for physical health conditions. Specifically, insurers cannot:
- Impose stricter limits on the number of covered sessions or days of treatment for SUD than for comparable medical or surgical conditions
- Charge higher copays, deductibles, or coinsurance for SUD treatment than for equivalent medical services
- Apply more restrictive prior authorization requirements or step-therapy protocols to SUD services than to medical services
- Apply narrower network standards to behavioral health providers than to medical providers
Who it applies to: NJ-regulated individual and group health insurance plans, including fully-insured employer-sponsored plans. Self-funded employer plans are governed by the federal MHPAEA rather than state law, though the parity requirements are substantially parallel.
Enforcement: The New Jersey Department of Banking and Insurance (NJDOBI) enforces state parity compliance within NJ-regulated plans. New Jersey has produced consent decrees against insurers found to have limited SUD coverage in violation of MHPAEA. NJ residents who believe their insurer has violated parity requirements can file a complaint with NJDOBI at dobi.nj.gov. Independent External Reviews are also available for coverage denials.
Practical significance: If your insurer requires prior authorization for outpatient addiction treatment but does not require equivalent prior authorization for outpatient physical health services, this may constitute a parity violation. Similarly, if your plan caps SUD outpatient visits but does not cap equivalent medical visits, a parity violation may have occurred. Valley Spring's admissions team can identify potential parity issues during the benefits verification process and can assist clients in filing complaints or appeals when coverage has been improperly denied or restricted.
2. New Jersey Health Insurance Market Preservation Act (Individual Mandate)
The New Jersey Health Insurance Market Preservation Act, enacted in 2018 and effective January 1, 2019, reestablished a state-level individual health insurance mandate after the federal ACA mandate penalty was reduced to zero. Under this law, most NJ residents must maintain qualifying health coverage or pay a state tax penalty known as the Shared Responsibility Payment.
The penalty is calculated as the greater of: 2.5% of household income (above the filing threshold) or a flat amount per uninsured individual in the household. Revenue from the penalty funds New Jersey's state-based premium assistance programs, helping to make coverage more affordable for lower-income residents.
Exemptions from the mandate are available for financial hardship, religious beliefs, short gaps in coverage (under three months), certain immigration statuses, and situations where the lowest-cost available plan exceeds 8.05% of household income. Exemptions are claimed on the NJ state tax return or through the NJ Health Insurance Marketplace.
Why this matters for addiction treatment: Maintaining health insurance under this mandate is directly relevant to addiction treatment access. Most major NJ insurance plans are required to cover SUD treatment under ACA essential health benefits requirements and NJ parity laws. Individuals who are uninsured may face both the penalty and significantly higher out-of-pocket costs for treatment. The free insurance verification service at Valley Spring can help confirm what any specific plan covers before treatment begins.
3. ACA Essential Health Benefits: SUD Treatment as a Required Benefit
Under the federal Affordable Care Act (ACA), mental health and substance use disorder services are designated as one of ten Essential Health Benefits (EHBs). This means all ACA-marketplace plans, Medicaid expansion plans, and small-group employer plans must include SUD treatment coverage. New Jersey implements and enforces EHB requirements within NJ-regulated plans through NJDOBI.
New Jersey's EHB benchmark plan includes specific SUD services such as:
- Medically supervised detoxification (inpatient and outpatient)
- Residential rehabilitation
- Partial hospitalization / partial care programs (PC)
- Intensive outpatient programs (IOP)
- Standard outpatient counseling
- Medication-Assisted Treatment (MAT) including buprenorphine, methadone, and naltrexone
- Dual diagnosis / co-occurring disorder treatment
Plans may not exclude these services, impose annual or lifetime dollar limits on EHBs, or apply cost-sharing that is inconsistent with parity requirements. Whether Valley Spring's specific services are covered under a given plan's EHB benefits depends on the plan's specific terms, and coverage details are confirmed during the free insurance verification process.
4. New Jersey Opioid Antidote Act and Harm Reduction Protections
New Jersey's Opioid Antidote Act (N.J.S.A. 24:6J-1 et seq.) requires pharmacies licensed in New Jersey to dispense naloxone (brand name Narcan) without a prescription, under a standing order issued by the NJ Commissioner of Health. This law is a critical harm reduction measure that has contributed to NJ's 27% decline in overdose deaths from 2024 to 2025 (NJ Office of the Chief State Medical Examiner / NJ Cares, 2025).
Under the Opioid Antidote Act and related NJ regulations:
- Naloxone is available without a prescription at most NJ pharmacies
- Health insurance plans in NJ are required to cover naloxone with no cost-sharing when dispensed under the standing order
- NJ Connect for Recovery (1-855-652-3737) and local health departments offer free naloxone training and distribution throughout the state
- The NJ Good Samaritan Law (N.J.S.A. 2C:35-30) provides limited immunity from drug possession charges for individuals who call 911 during an overdose — both the person calling and the person experiencing the overdose are protected
These laws collectively reduce the mortality risk associated with opioid use disorder and create a safer environment for people to seek treatment. Valley Spring incorporates information about naloxone access and NJ's Good Samaritan Law into safety planning for relevant clients.
5. Dependent Coverage Extension to Age 31
New Jersey law extends dependent coverage on a parent's employer-sponsored health insurance plan to age 31, compared to the federal ACA limit of age 26. To qualify, the young adult must be unmarried, childless, a New Jersey resident, and ineligible for other employer-sponsored group health coverage.
This extension is particularly relevant to addiction treatment access because young adults aged 26–31 are in a high-risk period for substance use disorder — often balancing new financial independence, career transitions, and social pressures without the stable employer health coverage that comes later in life. The NJ extension ensures that this age group can access parental insurance coverage during these transitional years.
6. Out-of-Network Consumer Protection Act (Surprise Billing Protections)
New Jersey's Out-of-Network Consumer Protection, Transparency, Cost Containment, and Accountability Act protects insured patients from surprise medical bills in several contexts:
- Emergency services at in-network hospitals must be billed at in-network rates, even if the treating provider is out-of-network
- Non-emergency services at in-network facilities must include upfront disclosure of the network status of all providers involved
- A binding arbitration mechanism resolves disputes between providers and insurers when billing conflicts arise
For addiction treatment specifically, this law is relevant when a patient is treated at an in-network facility but may encounter out-of-network providers such as consulting physicians, laboratory services, or specialist evaluators. Patients have the right to receive advance notice of any out-of-network component and to dispute unexpected bills through the state's arbitration process.
7. Preexisting Condition Coverage Guarantee
New Jersey law prohibits insurers from denying coverage or charging higher premiums based on preexisting medical conditions, including substance use disorder and mental health diagnoses. This protection applies to all individual and group insurance plans regulated by NJ.
Critical implication for SUD: A prior substance use disorder diagnosis or prior addiction treatment cannot be used by an NJ-regulated insurer to deny coverage, restrict benefits, or increase premiums. This protection is particularly important because stigma and discrimination against people with addiction histories have historically limited their access to health insurance. HIPAA further protects SUD treatment records — under 42 CFR Part 2, records of substance use disorder treatment at federally assisted programs receive even stronger confidentiality protections than general medical records, and cannot be shared without explicit written consent.
Patients' Rights When Coverage Is Denied
New Jersey residents whose insurance claims for addiction treatment have been denied have several rights and remedies:
Internal Appeal
All NJ health insurance plans must provide an internal appeals process for coverage denials. When a claim is denied, the insurer must provide a written explanation stating the specific clinical or policy basis for the denial. The patient or provider may submit additional clinical documentation to support medical necessity, and the insurer must review the appeal within defined timeframes (typically 30 days for standard appeals, 72 hours for urgent/concurrent care appeals).
External Independent Review
After exhausting internal appeals (or simultaneously for urgent care denials), NJ patients may request an Independent External Review through NJDOBI. The external review is conducted by an independent organization — not the insurer — and the result is binding on the insurance company. External review is available for medical necessity denials and experimental/investigational treatment denials.
Parity Violation Complaint
If the denial appears to be based on stricter requirements for SUD treatment than for comparable medical care, a formal parity violation complaint can be filed with NJDOBI. The department has the authority to investigate, require corrective action, and impose penalties on insurers found to have violated parity requirements.
SAMHSA and Federal Enforcement
For self-funded employer plans (which are governed by federal ERISA law rather than state insurance law), parity violation complaints can be filed with the U.S. Department of Labor's Employee Benefits Security Administration (EBSA) or with the Centers for Medicare and Medicaid Services (CMS).
Which NJ Insurance Plans Cover SUD Treatment at Valley Spring?
Most New Jersey insurance providers are required to cover substance use disorder treatment under federal and state parity law and ACA essential health benefits requirements. Valley Spring Recovery Center is in-network with more than 17 major plans including Horizon BCBS NJ, AmeriHealth NJ, Aetna, Cigna, UnitedHealthcare, Anthem, NYSHIP, Oscar, EmblemHealth, Fidelis, and others.
Coverage details — including specific benefits, prior authorization requirements, deductible status, and out-of-pocket costs — vary by plan and by individual policy. Exact coverage should always be verified before treatment begins. Valley Spring's admissions team provides free insurance verification with a written cost estimate returned within one business hour for in-network plans. Call (855) 924-5320 or complete the online verification form to get started — no commitment required to receive the benefits check.
Individuals who believe their insurer has improperly denied or restricted addiction treatment coverage — whether through parity violations, improper prior authorization denials, or network inadequacy — are encouraged to contact Valley Spring's admissions team, which can help navigate the appeals and complaint process alongside the clinical assessment.
