Drug Overdose Statistics by Type, State, and Demographic

Deaths by drug overdose spiked by 30% during the COVID-19 pandemic.
Dr Nora Volkow, the director of the National Institute of Drug Abuse at the National Institutes of Health expected drug overdose cases to reduce after the pandemic. Unfortunately, overdose deaths continue to rise—now owing to stress and excessive use of opioids.
In this post, let’s take a look at important drug overdose statistics by type, state, and demographic.
KEY TAKEAWAYS
- In September 2023, there were 105,879 reported overdose deaths, marking a significant rise from the 88,879 recorded in September 2020. This reflects a 19.12% increase over the three years.
- 92% of the total drug overdose deaths are preventable with timely naloxone administration, better prescription, or close monitoring.
- According to the Centers for Disease Control and Prevention (CDC), the COVID-19 pandemic led to a 30% increase in deaths by drug overdose from 2019 to 2020. The leading causes of drug overdose during this time were depression, anxiety, financial strain, or stress about COVID-19.
- Opioids emerge as the foremost culprit in both fatal and non-fatal drug overdoses.
- Deaths by drug overdose significantly increased in Washington, Oregon, Alaska, and Nevada between 2022 and 2023.
- Deaths by drug overdose significantly reduced in North Carolina, Wisconsin, Florida, and Georgia between 2022 and 2023.
- Middle-aged men are more than twice as likely to die from a drug overdose as compared to women.
- The highest number of drug overdose deaths among women occurs within the age range of 44 to 54 years old.
What Are The Non-fatal Drug Overdose Statistics?
Not all drug overdose cases result in death, many end up in hospitalization. Non-fatal drug overdose statistics reveal prevalent opioid overdoses with a significant presence of fentanyl, gender and age disparities in overdose rates, and notable variations in regional emergency department visits and hospitalizations due to heroin and stimulant use according to data collected by the CDC Drug Overdose Surveillance and Epidemiology (DOSE) system.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
Opioids
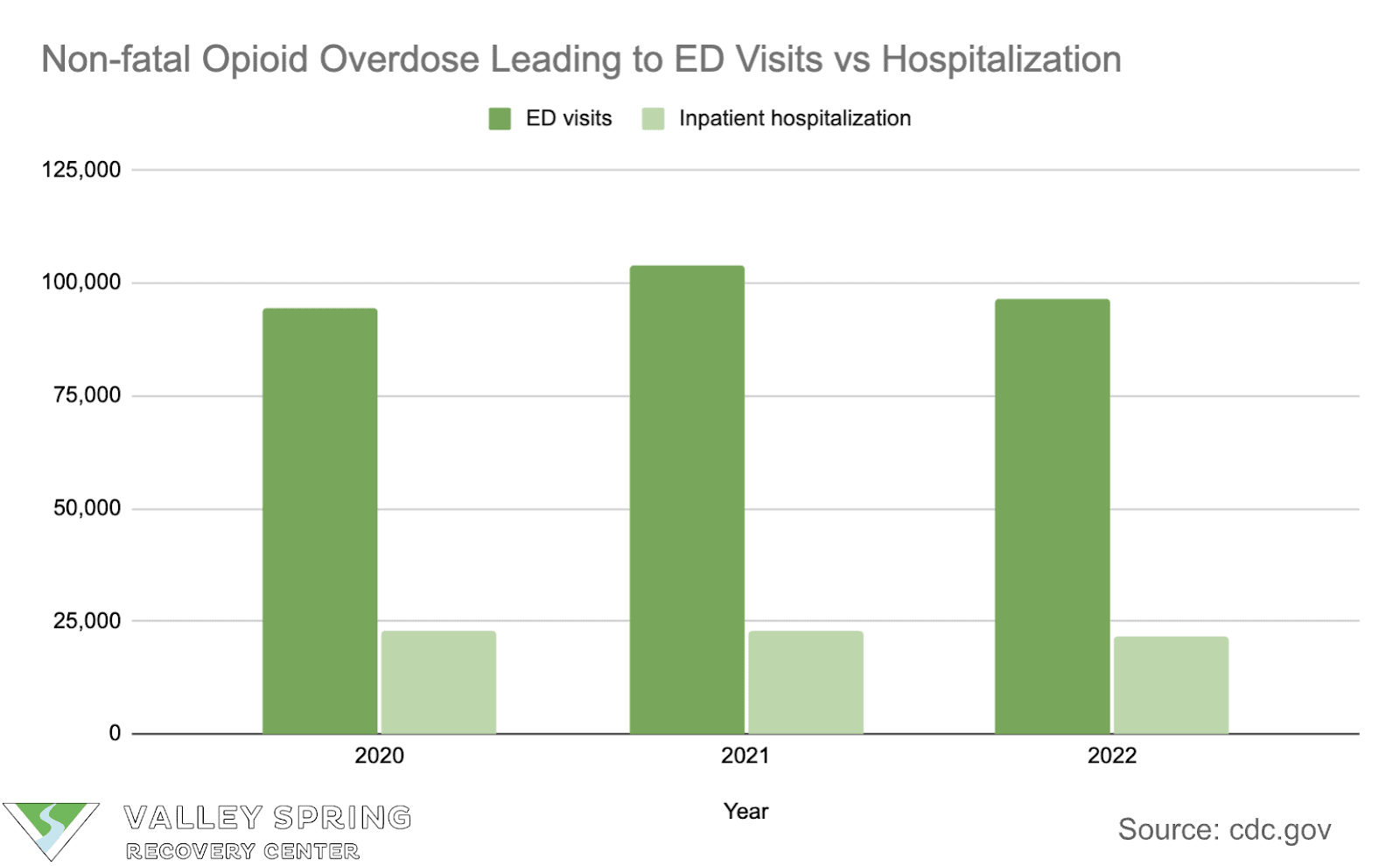
- Non-fatal opioid overdoses are much more common than fatal opioid overdoses.
- According to a CDC survey, 78% of non-fatal opioid overdose cases tested from 2020 to 2023 had traces of fentanyl or fentanyl analogs in their blood specimen.
- Methadone (42%) and tramadol (32%) are the primary prescription opioids associated with overdose.
- Overdosed individuals can be discharged one hour after administration of naloxone.
- A study conducted in 2020 by JAMA looked at 20,312 commercially insured U.S. youths aged 11 to 24 years who experienced a nonfatal opioid overdose. The results indicated:
- Females had a higher incidence of overdose compared to males between ages 11-16. Most of the females had a mood/anxiety disorder.
- Males had a higher incidence of overdose compared to females after age 17.
- The annual count of ED visits for opioid abuse by men is twice as much as that of women.
- Men and women aged 35-54 are more likely to face opioid overdose as compared to other age groups.
- Seven states—namely Washington, Oregon, Nevada, Colorado, Arizona, Illinois, and New Jersey—witnessed a significant increase in opioid abuse between 2022 and 2023.
Heroin
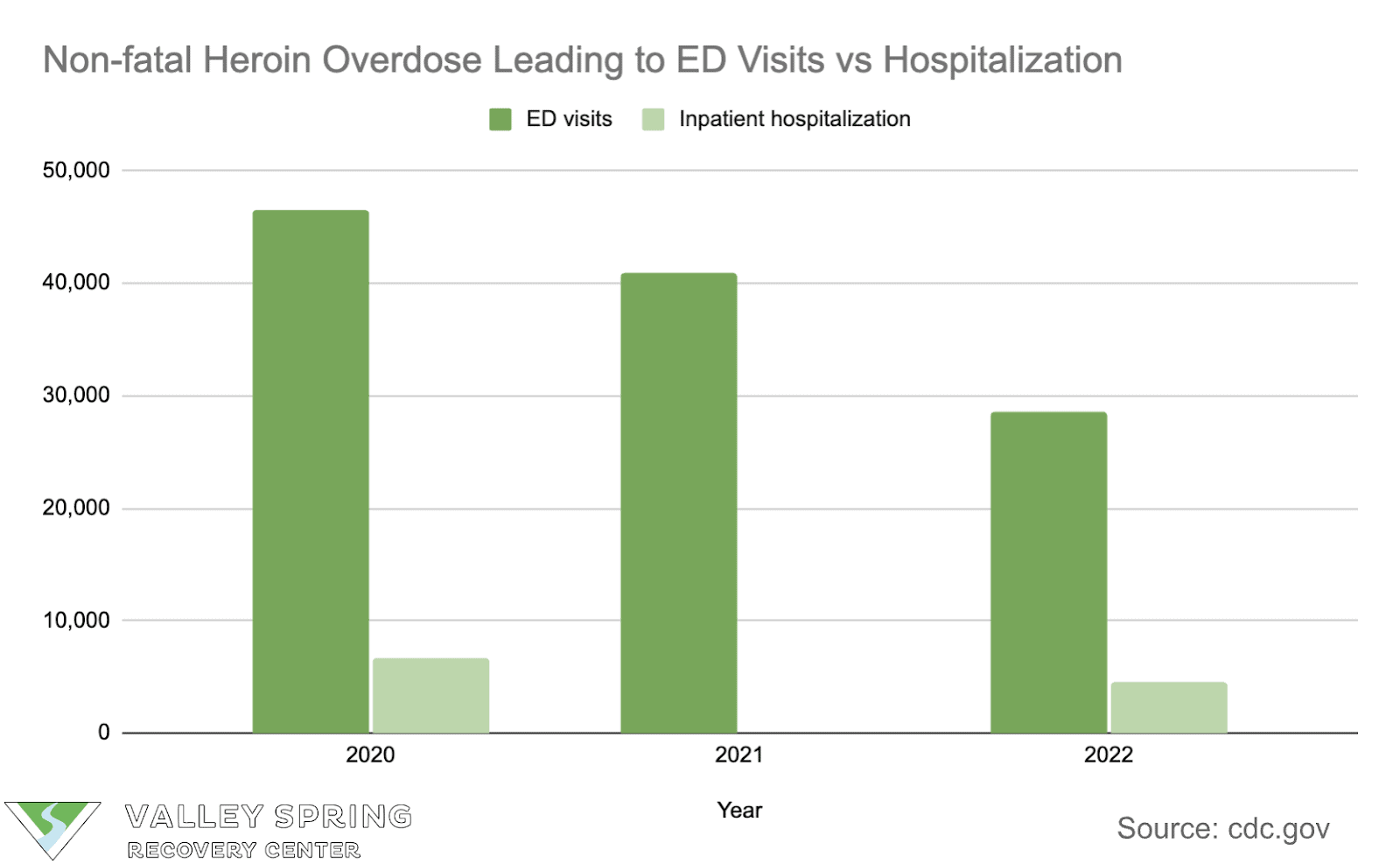
Non-fatal heroin overdose statistics reveal a pattern where men across all age groups are more likely than women to visit emergency departments, with school-aged children also impacted, and states like Illinois, Delaware, and New York experiencing the highest rates in 2022.
- Most people who use heroin first misuse prescription opioids.
- Men across all age groups (above 14) are prone to consuming heroin at a rate double that of women, leading to more frequent visits to the emergency department and hospitalizations.
- Heroin usage is seen among school-going children. 2% of high school students have used heroin at least once in their lifetime.
- In 2022, Illinois, Delaware, and New York had the highest rate of non-fatal heroin overdose cases.
- In the same year, Colorado and Kansas had the lowest rate of non-fatal heroin overdose cases.
Heroin addiction statistics have changed over the years as a result of new drugs being introduced to the market including fentanyl and xylazine which have contributed to increased overdose rates.
Stimulants
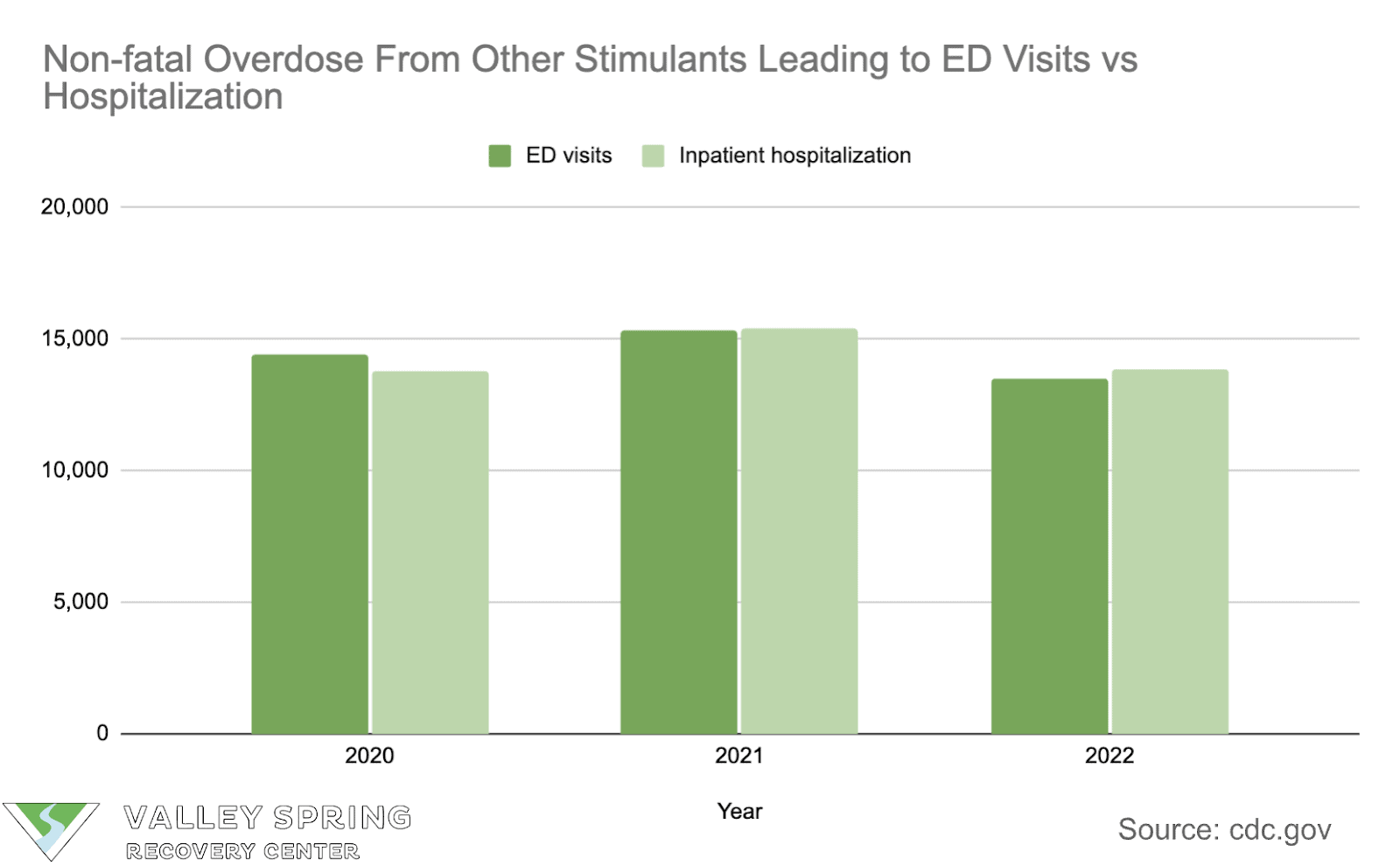
Stimulants including methamphetamine, and cocaine affect different demographics greatly where men above the age of 14 have twice the emergency department visits and hospitalizations as women. The non-fatal stimulant addiction statistics are listed below according to the CDC.
- Men of all age groups (above 14) experience double the annual number of emergency department visits and inpatient hospitalizations following a stimulant drug overdose compared to women.
- In 2022, Oregon, New York, and North Carolina had the highest rate of non-fatal stimulant drug overdose.
- Nebraska and Utah had the lowest rate of non-fatal stimulant drug overdose cases in 2022.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your drug addiction journey, we are here to help.
What Are The Fatal Drug Overdose Statistics by Drug Type?
Fatal drug overdose statistics indicate opioids as the predominant cause of drug-related deaths, with significant contributions from stimulants such as methamphetamine and cocaine. Additionally, emerging trends data from the CDC show an increase in fatalities associated with synthetic opioids like fentanyl and a variation in overdose deaths by geographic region, reflecting local drug availability and usage patterns.
Opioids
- Opioids are responsible for 67.8% of all drug overdose deaths.
- From 2018 to 2019, the rise in opioid overdose deaths was 6.99%. However, during the pandemic (2019 – 2020), opioid overdose deaths spiked by up to 41%.
- The percentage change from 2020 to 2021 decreased to 18%, suggesting a smaller rise in opioid overdose deaths. However, the actual number of deaths in 2021 exceeded that of 2020, indicating an ongoing upward trend.
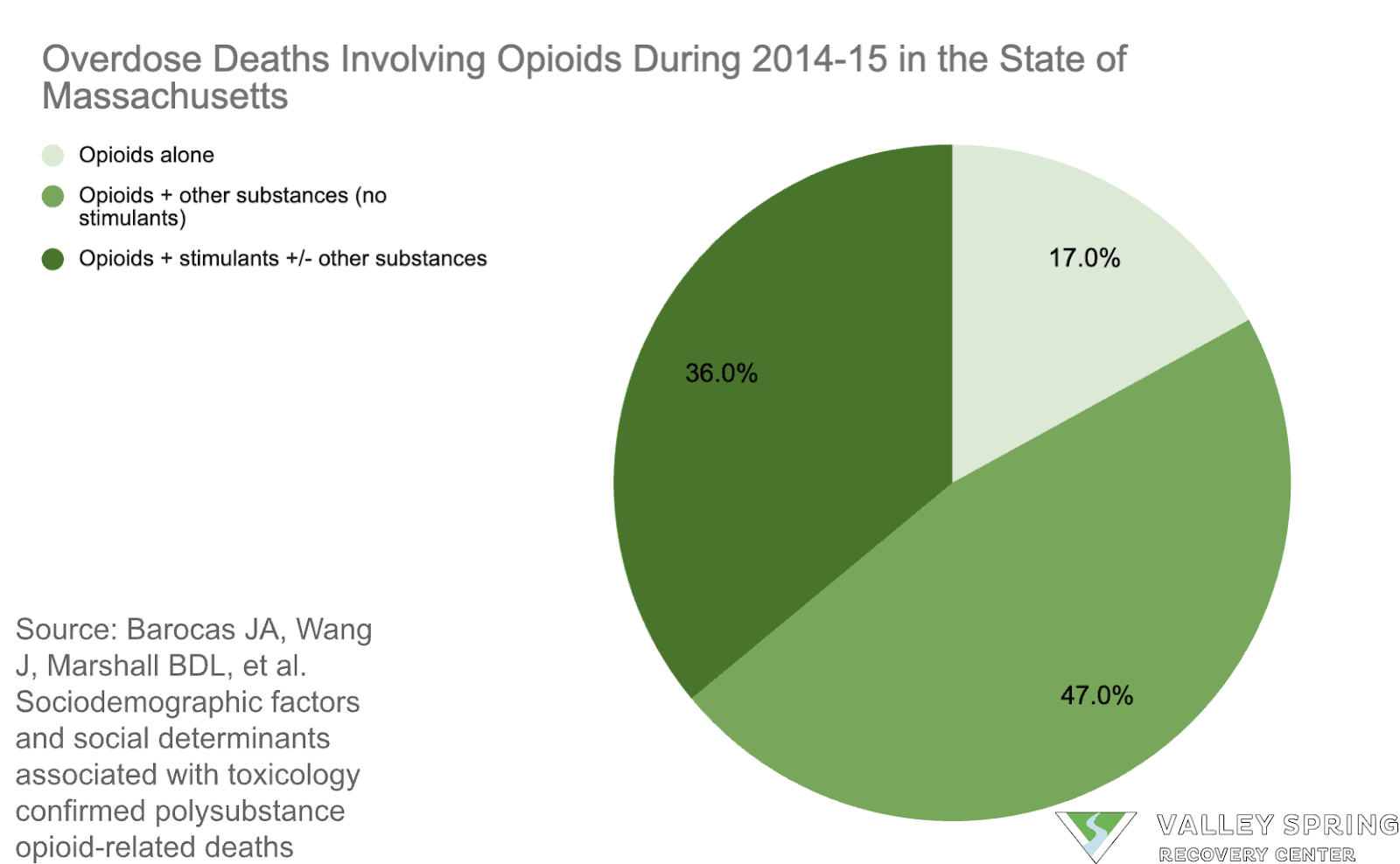
- Following 2021, the primary cause of overdose deaths has moved away from prescription opioids alone. Now, synthetic opioids or opioids combined with other stimulants account for approximately 88% of opioid-related overdose deaths.
Heroin
- Nearly 14,000 Americans die every year due to heroin overdose.
- Deaths caused by heroin overdose peaked in 2017 with about 15,482 reported deaths. The trend declined over the years with 9,173 heroin overdose deaths in 2021.
Stimulants
The count of psychostimulant overdose deaths increased by 37% from 2020 to 2021. The key facts about stimulants that lead to overdose are listed below.
- Rising Rates of Stimulant Overdoses: According to the U.S. Centers for Disease Control and Prevention (CDC), the rate of drug overdose deaths involving stimulants such as methamphetamine (commonly listed under “psychostimulants with abuse potential”) has seen a significant increase. In 2020, there were approximately 24,576 overdose deaths involving psychostimulants, marking a nearly 180% increase from 2015.
- Co-involvement with Opioids: Data from the National Institute on Drug Abuse (NIDA) in 2019 indicates that many stimulant-related overdoses also involve opioids. Approximately 50% of methamphetamine-related overdose deaths also involve opioids, highlighting the dangerous trend of polysubstance use.
- Geographical Variation: The impact of stimulant overdoses varies significantly by region. For instance, the Western United States has experienced the highest rates of methamphetamine-related deaths, correlating with the higher availability and use of methamphetamines in these areas.
- Demographic Disparities: According to research from the Substance Abuse and Mental Health Services Administration (SAMHSA), stimulant overdose rates tend to be higher among middle-aged adults aged 35 to 54. This demographic accounted for the largest proportion of methamphetamine admissions to emergency departments.
- Emergency Department Visits: A 2021 report from SAMHSA noted that emergency department visits related to stimulant use (including methamphetamine) increased by 3% annually from 2016 to 2019. The majority of these visits were due to serious medical outcomes, including overdose.
These statistics underscore the growing public health issue of stimulant use and the complex nature of drug overdose crises, often involving multiple substances and affecting a wide range of populations.
Cocaine
- Cocaine-involved overdose death rates increased by nearly 22% from 2020 to 2021.
- More than 24,000 Americans died in 2021 from an overdose involving cocaine. This means cocaine accounted for nearly 23% of all overdose deaths in 2021.
Methamphetamine
- In 2020, 2.5 million Americans aged 12 or older reported having used methamphetamine in the past year.
- As per the National Institute on Drug Abuse (NIDA), there was an almost threefold increase in methamphetamine-related overdose fatalities among individuals aged 18-64 between 2015 and 2019.
- There was a 37% rise in the count of Americans diagnosed with a substance use disorder (SUD) linked to methamphetamine from 2015 to 2019.
- In 2019, fentanyl caused 31% of all meth-related overdose deaths, showing an increase of more than fourfold compared to its proportion in 2015.
- Adults with limited income, those on Medicaid, the uninsured, those with lower education, males, middle-aged adults, and people who live in rural areas are at increased risk for methamphetamine use.
Rediscover Life at Valley Spring Recovery Center
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.
Verify Benefits
Alcohol
- Alcohol contributed to around 7.1% of ED visits and 17.4% of fatalities resulting from opioid overdose in 2020.
- Excessive alcohol use leads to over 140,000 deaths annually, with approximately 97,000 males and 43,000 females affected. This positions alcohol as one of the leading preventable causes of mortality in the United States.
- Analysis of death records between 2019 and 2020 revealed a notable surge in alcohol-related deaths, soaring from approximately 79,000 to over 99,000 fatalities. This marks a 25.5% increase.
- Leading causes of alcohol-related deaths from chronic conditions in the United States between 2015 and 2019 include liver disease, cardiovascular disease, cancer, and alcohol use disorder (AUD).
- In 2021, fatalities resulting from alcohol-impaired driving amounted to 13,384 deaths, accounting for 31% of total driving fatalities.
- The CDC reports that 21.0% of individuals who died by suicide had blood alcohol concentrations of 0.1% or higher.
- Among individuals who take their own lives, AUD stands as the second most prevalent disorder, contributing to approximately 25% of suicide deaths.
Cannabis
- At least 35 people experienced serious heart problems shortly after using cannabis according to the study ‘Cannabis as a cause of death’ from Forensic Science International.
- At least 13 deaths from a cardiovascular mechanism have been reported from cannabis use, although this figure is likely underestimated.
- As reported by the American Association of Poison Control Centers (AAPCC), in 2014, there was just a single fatality linked to cannabis exposure out of 2,047 calls received by poison control centers.
What Are The Fatal Drug Overdose Statistics by State?
The top four cities with the most overall drug use are listed below according to data from the CDC are listed below.
- Wichita, Kansas
- Tulsa, Oklahoma
- Oklahoma City, Oklahoma
- Mesa, Arizona
In 2022, the top five cities with the most heroin use are listed below.
- Omaha, Nebraska—3.4% of the population used heroin
- Indianapolis, Indiana—3.4% of the population used heroin
- Columbus, Ohio—3.3% of the population used heroin
- Nashville, Tennessee—3.2% of the population used heroin
- Oklahoma City, Oklahoma—3.1% of the population used heroin
- In Oregon, the total reported overdose deaths by September 2023 were about 1758. The previous annual count was 1242, suggesting a percentage rise of 41.55%.
- Washington experienced a 41.40% rise in annual drug overdose deaths. The total number of overdose deaths reported between September 2021 and September 2022 was 2,483, while the total reported deaths between September 2022 and September 2023 reached 3,511.
The following four states had the highest count of deaths by overdose from 2022-2023.
- Ohio (5103 reported cases by September 2023)
- Texas (5831 reported cases by September 2023)
- Florida (7669 reported cases by September 2023)
- California (12,823 reported cases by September 2023)
- With only 79 deaths per year, Wyoming has the lowest number of drug overdose deaths out of all states.
Are you covered for treatment?
Valley Spring Recovery Center is an approved provider for Blue Cross Blue Shield and Cigna, while also accepting many other major insurance carriers.
Check Coverage Now!What Are The Fatal Drug Overdose Statistics by Demographic?
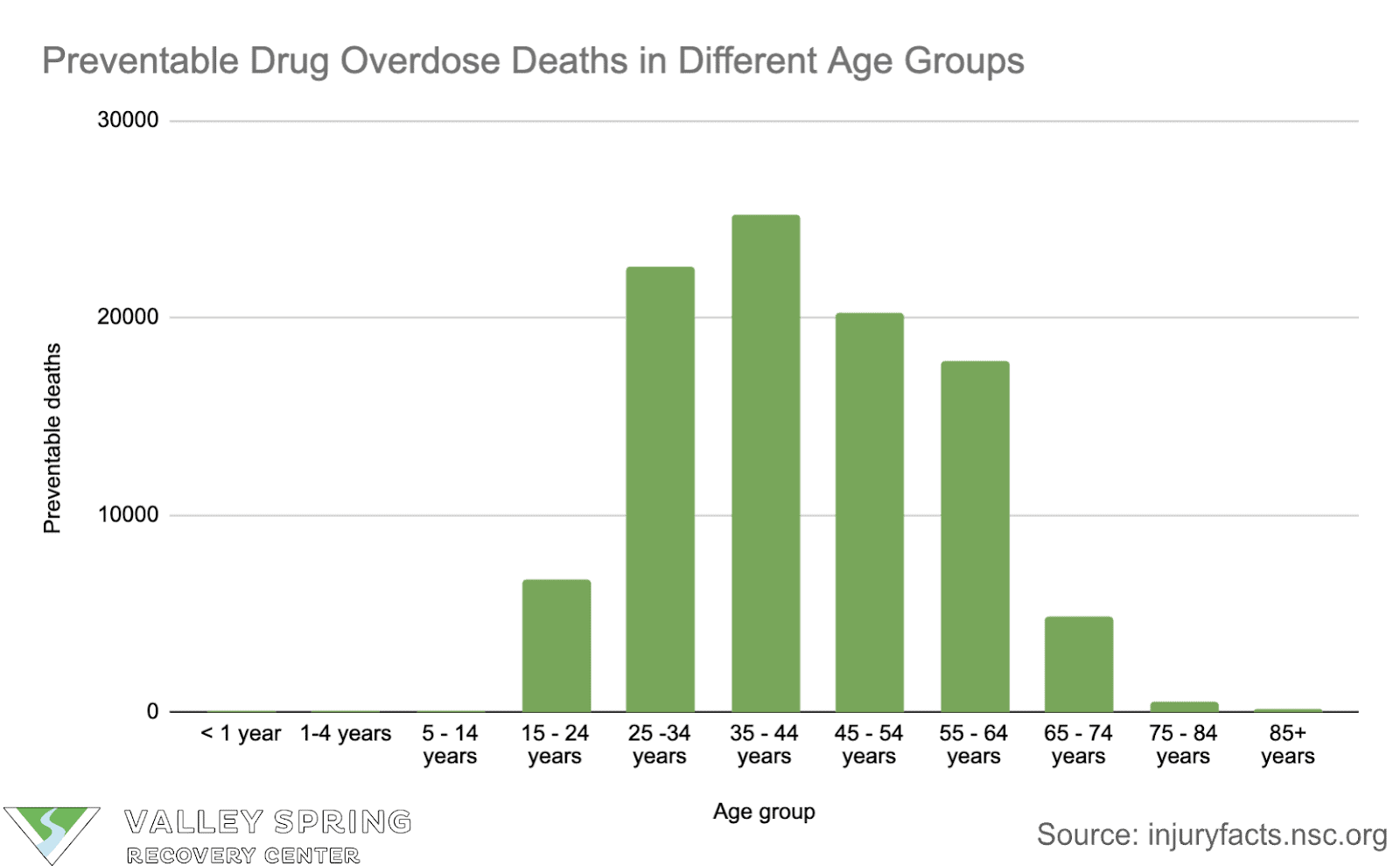
Demographics play an important role in determining the risk of drug overdose. Here are a few key statistics:
- The rate of preventable drug overdose deaths was highest for the age group 35 – 44, for both genders and all drugs. Here’s a breakdown:
- In 2021, drug overdose death rates were the highest for non-Hispanic American Indian or Alaska Native (AIAN) people, at 56.6 deaths per 100,000 population.
- Non-Hispanic Asian people had the lowest drug overdose death rates in both 2020 and 2021, with 4.6 deaths and 4.7 deaths per 100,000 population, respectively.
- Non-Hispanic Native Hawaiian or Other Pacific Islander individuals saw a 47% increase in drug overdose death rates from 2020 to 2021, rising from 13.7 deaths to 20.1 deaths per 100,000 population.
- Non-Hispanic AIAN people experienced a 33% increase in drug overdose death rates during the same period, with rates climbing from 42.5 deaths to 56.6 deaths per 100,000 population.
- In the case of females, American Indians and Alaskan Natives are the most likely to die from a drug overdose.
- In the case of males, African Americans are the most likely to die from a drug overdose.
What Are Opioids?
Opioids are a class of drugs used for pain relief. Despite their effectiveness in managing pain, opioid addiction is high risk and can cause dependence, and overdose, which has led to three waves of opioid overdose deaths since the 1990s. Studies have revealed the overdose rate for opiates increases after relapse due to changes in tolerance.
Which Age Group Is the Most Affected by Drug Overdose?
In both males and females, the age group 35 – 44 is the most affected by drug overdose. This is true for all drug types.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
What Are Some Signs of a Potential Drug Overdose?
Some signs of potential drug overdose include shallow or labored breathing, confusion, unconsciousness, pinpoint pupils, pale or clammy skin, vomiting, and seizures. If someone exhibits these symptoms, seek immediate medical help.
How do overdose rates correlate with state policies for treatment funding and harm reduction?
Research suggests that the policies of a state can influence overdose rates, such as the availability of naloxone, the implementation of prescription drug monitoring programs, the regulation of opioid prescriptions, and the support for substance use disorder treatment programs have all been associated with variations in overdose rates. States with robust public health strategies and harm reduction policies often report different outcomes compared to those with less comprehensive approaches.
Share This Post















