Drug rehab refers to structured treatment programs designed to help people reduce or stop their use of addictive substances. These programs combine detoxification, counselling, behavioral therapy, medical care, and aftercare support. Drug rehab addresses physical dependence as well as psychological and social factors contributing to addiction. The goal is to equip individuals with tools to sustain recovery, prevent relapse, and improve overall functioning, not only to achieve short-term abstinence.
The effectiveness of drug rehab varies widely. Drug rehab reduces drug use, lowers criminal involvement, improves health, and helps rebuild relationships. The success of drug rehab depends heavily on the person, the substance involved, the duration and quality of treatment, and post-treatment support. Relapse rates within a year often fall in the 40–60 % range, similar to those of many chronic illnesses. In 2022, New Jersey recorded 85,266 admissions and 84,437 discharges in substance use programs, showing strong engagement in drug rehab.
What is the Effectiveness of Drug Rehab?
The effectiveness of drug rehab includes helping individuals recover from substance use through structured medical care, counseling, and emotional support. Rehab focuses on treating both the body and mind to build long-term sobriety. Its success depends on the quality of treatment, the person’s involvement, and continued care after the program ends.
Here is the effectiveness of drug rehab.
- Personal Commitment: People who stay focused and follow their recovery plan achieve better outcomes.
- Comprehensive Treatment: A mix of detox, therapy, and social support increases the chance of lasting recovery.
- Duration of Treatment: Longer participation in rehab often leads to stronger and more stable results.
- Aftercare and Support Networks: Continued guidance through counseling or support groups helps prevent relapse.
- Tailored Programs: Individualized treatment plans work better than general approaches.
- Medical and Mental Health Care: Addressing both addiction and mental health issues improves recovery success.
What is the Success Rate of Drug Rehab?
The success rate of drug rehab depends on factors such as addiction type, treatment quality, and individual commitment. According to the National Institute on Drug Abuse, about 40–60% of people remain sober one year after treatment. According to the New Jersey Substance Abuse Monitoring System (NJSAMS), 64.8% of individuals in rehab were free from drug or alcohol use by the time of discharge, and 53.2% completed their treatment plans.
Nationally, 89% of those who complete alcohol treatment stay sober for at least one month, and 85–95% maintain recovery for up to nine months after rehab. Detox programs show a success rate of about 68%, while some states like Florida report up to 70% completion rates. These figures show that rehab programs lead to significant improvements in sobriety and quality of life when individuals receive consistent care and support.
Why is Drug Rehab Treatment not Successful?
Drug rehab treatment is not successful because many individuals face barriers such as limited access to quality care, financial constraints, and reluctance to seek help. Social and economic disparities prevent equal access to treatment services. In some cases, people leave rehab early or do not receive proper aftercare, which increases the risk of relapse.
According to the National Institutes of Health, relapse rates for addiction are similar to those of chronic illnesses like asthma or hypertension. It shows that recovery requires long-term management. Success improves when treatment is continuous, adaptive, and supported by programs like 12-step groups that provide structure and community support.
How Is Success In Drug Rehab Addiction Treatment Determined and Measured?
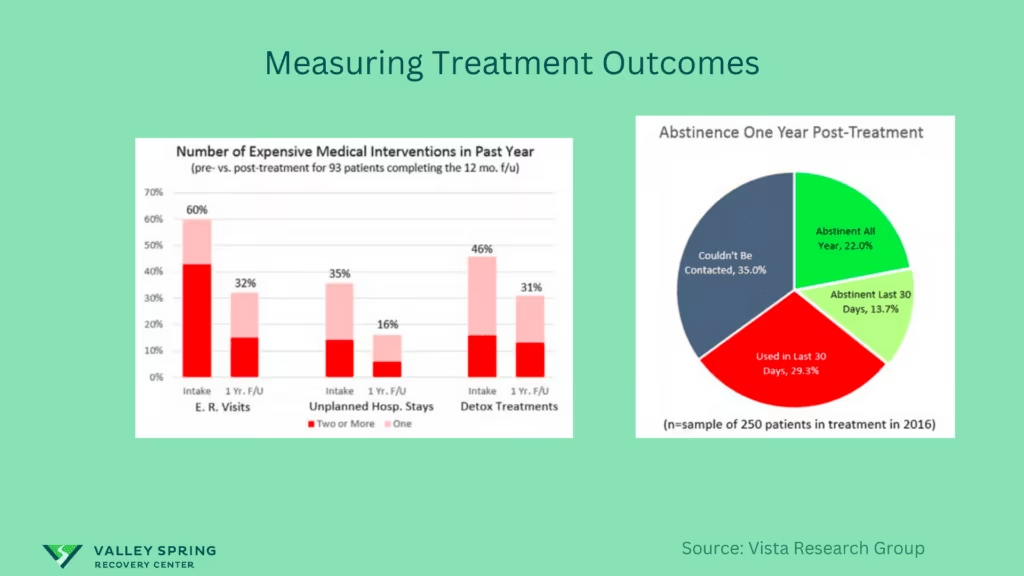
Success in drug rehab addiction treatment is determined and measured includes improvements in mental health, stable employment, better relationships, and reduced criminal behavior. According to the CDC, these outcomes reflect overall recovery and quality of life. Organizations like Vista Research Group measure success by following up with patients one, six, and twelve months after treatment to assess continued sobriety and life stability. This approach shows that true success in rehab is about lasting change and personal growth.
Is 30 Days Enough Time To Recover From Substance Use Disorder?
No, 30 days is generally not enough time to fully recover from a substance use disorder; it is enough to begin detox, stabilization, assessment, and initial skill-building if followed by ongoing care. Best outcomes come from a continuum of care lasting at least several months, including step-down treatment (intensive outpatient or outpatient), medications for alcohol/opioid use disorders when indicated, peer support, family involvement, and structured relapse-prevention planning. Duration should match substance type, severity, co-occurring conditions, and support network, with sustained recovery typically requiring long-term follow-up and continuing care.
How Does Relapse Affect Drug Rehab Effectiveness?
Relapse affects drug rehab effectiveness by showing that recovery is an ongoing process that requires adjustments in treatment. It does not mean failure but indicates the need for continued support or a different approach to care. According to SAMHSA, about 50% of individuals experience at least one relapse after treatment. It highlights that addiction involves setbacks before long-term recovery is achieved.
What is the Success Rate of Inpatient or Outpatient Drug Rehab?
The success rate of inpatient or outpatient drug rehab depends on the level of care, addiction severity, and individual commitment. Inpatient programs show higher success rates because they offer 24/7 medical and emotional support, structured routines, and fewer external distractions. According to the National Institute on Drug Abuse, inpatient rehab programs help about 50–65% of participants maintain sobriety during and shortly after treatment, especially when followed by strong aftercare and counseling.
Outpatient rehab also leads to positive results, particularly for individuals with mild addictions or strong home support systems. Success rates range from 35–50%, depending on participation consistency and the availability of follow-up care. While inpatient rehab provides intensive support for initial recovery, outpatient programs are effective when combined with therapy, support groups, and lifestyle changes. Both approaches work well when matched to the person’s unique recovery needs.
What Is The Difference Between Inpatient vs Outpatient Drug Rehab?
The difference between inpatient and outpatient drug rehab includes the level of care, environment, and treatment intensity each program provides. Choosing between the two depends on factors such as addiction severity, personal responsibilities, and available resources.
Here are some differences between the two;
- Severity of Addiction: Inpatient care suits severe or long-term addiction, while outpatient care works for mild to moderate cases.
- Personal Obligations: Outpatient programs fit those balancing work, school, or family duties.
- Support System: A strong home environment supports outpatient recovery; inpatient is better for unstable surroundings.
- Financial Considerations: Inpatient treatment costs more due to residential and 24/7 care.
- Commitment Level: Outpatient rehab requires high self-discipline and consistent participation.
- Professional Guidance: Consulting an addiction specialist helps determine which program best fits recovery needs.
Does The Outpatient Drug Rehab Work?
Yes, the outpatient treatment model works, especially as a follow-up to inpatient rehab. It helps individuals maintain sobriety, continue therapy, and adjust to daily life while receiving ongoing medical and emotional support. According to SAMHSA, outpatient rehab programs like the IOP serve a large portion of patients in addiction care and show positive outcomes in sustaining recovery and preventing relapse.
What Can Improve the Success Rate of Addiction Recovery in Rehabs?
Incorporating personalized treatment plans and individual behavioral therapy can improve the success rate of addiction recovery in rehabs. Behavioral therapy helps individuals identify and change harmful thoughts and actions, supporting long-term sobriety. Participation in 12-step meetings and peer support groups provides emotional encouragement and accountability, which are vital for maintaining recovery and preventing relapse.
What Should I Do After Completing a Drug Rehab Program?
After completing a drug rehab program, recovery continues beyond treatment and requires dedication, structure, and ongoing support. Staying connected to professional care and positive environments helps maintain sobriety and prevent relapse. Building a healthy lifestyle, managing stress, and engaging in meaningful activities are key parts of long-term recovery.
Here’s what you should do after completing a drug rehab;
- Continuous Support: Stay connected with family, friends, and support groups like AA or NA.
- Regular Check-ins: Meet with therapists or counselors to track progress and adjust goals.
- Medication Management: Follow prescribed treatments to control cravings and withdrawal symptoms.
- Healthy Lifestyle: Eat well, exercise regularly, and get enough sleep to support mental health.
- Meaningful Activities: Engage in work or hobbies that provide purpose and stability.
- Coping Strategies: Practice skills learned in therapy to handle stress and avoid relapse triggers.
What are the Other Things You Think About When Researching Drug Rehab Options?
The other things you think about when researching drug rehab options include the facility’s accreditation, treatment methods, and staff qualifications. You must check success rates, patient reviews, and whether the program offers personalized care plans. Location, cost, and aftercare support also play a major role in choosing the right rehab for drug addiction.
How Do You Identify an Effective Treatment Facility?
You identify an effective treatment facility by ensuring it is accredited and staffed with certified healthcare professionals. Accreditation from organizations like the Joint Commission or CARF shows that the center meets high standards of care and safety. You must review patient testimonials, success rates, and treatment approaches to confirm they use evidence-based methods. A good facility offers personalized treatment plans, medical supervision, and strong aftercare support to help patients maintain long-term recovery.
What are Alcohol Rehab Success Rates?
The alcohol rehab success rate is about 50–60%, according to the National Institute on Alcohol Abuse and Alcoholism (NIAAA). Success depends on factors such as program duration, treatment quality, and ongoing support after rehab. Individuals who continue therapy and participate in support groups are more likely to maintain long-term sobriety.

